What Is CAQH? The Complete Guide to Provider Credentialing, ProView Setup, and Payer Enrollment
The Qualigenix Editorial Team comprises certified medical billing professionals, CPC-credentialed coders, prior authorization specialists, and revenue cycle consultants with more than 40 years of combined hands-on experience serving solo physicians, group practices, hospitals, and ASCs across 38+ specialties in the United States. Every guide, article, and resource published on the Qualigenix blog is researched against current CMS guidelines, Federal Register notices, AMA policy updates, and payer-specific billing rules — and reviewed for compliance accuracy before publication. Our content reflects the same standards we apply to our client work: 99% claim accuracy, 95% first-pass acceptance, and a 30% average reduction in AR days.
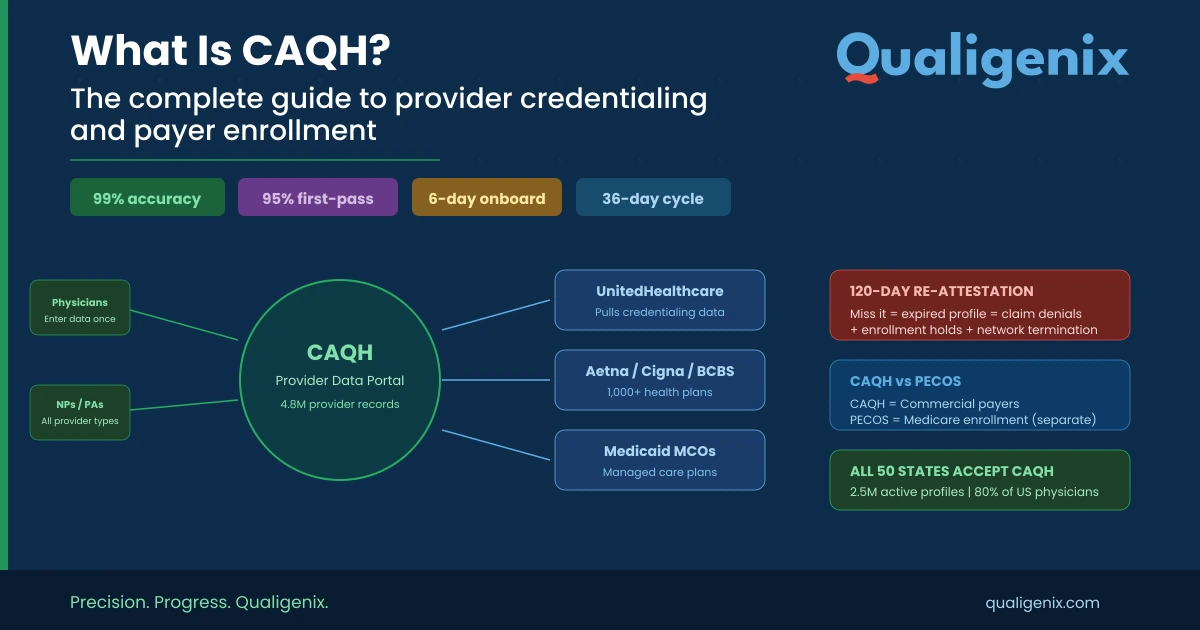
| Summary: CAQH (Council for Affordable Quality Healthcare) is a nonprofit that operates the most widely used provider credentialing database in the United States. Its flagship platform, CAQH ProView (now called the CAQH Provider Data Portal), allows healthcare providers to enter their credentialing information once and share it with multiple health plans. With 4.8 million provider records, 2.5 million active profiles, and participation from over 1,000 health plans covering 300+ million Americans, CAQH is the de facto standard for commercial payer credentialing. This guide covers what CAQH is, how to set up and maintain your profile, the 120-day attestation requirement, and how Qualigenix’s credentialing services speed the entire process. |
If you’re a healthcare provider trying to get credentialed with insurance plans, the question what is CAQH is one of the first you’ll encounter. Almost every commercial health plan in the country requires a CAQH profile as part of the credentialing and enrollment process. Without one, you can’t join payer networks, you can’t bill insurance, and you can’t get reimbursed.
Yet CAQH is one of the most misunderstood pieces of the provider enrollment puzzle. Many providers think completing a CAQH profile automatically enrolls them with health plans—it doesn’t. Others let their profile lapse past the 120-day attestation window and wonder why claims start getting denied. The gap between what CAQH does and what providers think it does costs practices weeks of delayed reimbursement and thousands in lost revenue.
This guide explains exactly what CAQH is, how the Provider Data Portal works, what information you need to complete your profile, the critical 120-day attestation rule, and how CAQH fits into the broader provider credentialing and payer enrollment process. We’ll also cover how Qualigenix’s medical credentialing services manage the entire CAQH lifecycle so your team can focus on patient care instead of administrative paperwork.
What Is CAQH?
| CAQH stands for the Council for Affordable Quality Healthcare, a nonprofit alliance founded by leading U.S. health plans to simplify healthcare administration. Its flagship product, the CAQH Provider Data Portal (formerly CAQH ProView), is a centralized online database where providers enter their credentialing information once and authorize health plans to access it. Over 1,000 health plans use CAQH, and all 50 states accept its credentialing application as a standard form. |
CAQH was established over 20 years ago to solve a specific problem: providers were filling out essentially the same credentialing application dozens of times for different insurance companies. Each payer had its own forms, its own requirements, and its own timeline. CAQH created a single, standardized repository where providers enter their information once—demographics, education, training, licensure, malpractice history, practice locations—and then authorize specific payers to pull that data directly.
Today, 80% of U.S. physicians have a complete CAQH profile, and 2.5 million providers actively maintain their data in the system. CAQH saves the healthcare industry an estimated $2 billion annually in administrative costs by eliminating redundant paperwork (per CAQH annual reports). For providers, a complete and current CAQH profile is the gateway to faster payer credentialing, faster enrollment, and faster time-to-revenue.
CAQH: Key Stats at a Glance
| Metric | Value / Source |
| Provider records in CAQH database | 4.8 million (CAQH) |
| Providers actively maintaining profiles | 2.5 million (CAQH) |
| Health plans using CAQH | 1,000+ (CAQH) |
| Americans covered by CAQH-participating plans | 300+ million (CAQH) |
| U.S. physicians with complete CAQH profiles | 80% (Relias 2026) |
| States accepting CAQH credentialing application | All 50 states |
| Re-attestation frequency required | Every 120 days (CAQH policy) |
| Credentialing time reduction with timely CAQH maintenance | Up to 40% (CAQH 2025 Solutions Suite) |
| Estimated annual industry savings from CAQH | $2 billion (CAQH) |
| Average time to complete initial CAQH profile | 1–2 hours (CAQH User Guide) |
| Average time for CAQH profile to become active | 3–10 business days |
How Does the CAQH Provider Data Portal Work?
The CAQH Provider Data Portal (formerly CAQH ProView) functions as a centralized credential repository. Here’s the workflow from registration to payer access:
Step 1 — Register and obtain your CAQH ID: Visit proview.caqh.org and self-register. You’ll enter your name, NPI, SSN, DEA number, license information, and practice address. CAQH assigns you a unique CAQH ID—this is the identifier you’ll provide to every payer going forward.
Step 2 — Complete your full profile: The CAQH application covers demographics, education and training history, work history, licensure, board certifications, hospital privileges, malpractice history, insurance details, and practice locations. Completing the initial profile typically takes 1–2 hours if your documents are prepared in advance (per CAQH Provider User Guide Version 43).
Step 3 — Upload supporting documents: Scan and upload your current medical license, DEA registration, board certificates, malpractice insurance face sheet, CV, and any specialty certifications. Use PDF format and label files clearly (e.g., StateLicense_NY_2026.pdf). Expired or illegible documents will pause processing.
Step 4 — Authorize payers to access your profile: Select the health plans you want to share your data with. Without authorization, payers cannot access your CAQH information—even if your profile is 100% complete. This is a step many providers overlook.
Step 5 — Attest and submit: Review all information for accuracy and submit your attestation. Your attestation is legally binding—you’re certifying that everything in your profile is true and current. CAQH typically processes and activates profiles within 3–10 business days.
Step 6 — Re-attest every 120 days: This is the most frequently missed step. CAQH requires providers to log in and confirm their data accuracy every 120 days (every 180 days for Illinois providers). If you miss the deadline, your profile status changes to “Expired” and payers lose access to your data—which can trigger claim denials, enrollment freezes, and even network termination.
Does Completing a CAQH Profile Automatically Enroll You with Insurance Plans?
No. CAQH is a data repository, not a credentialing or enrollment service. Completing your profile makes your data accessible to payers you’ve authorized, but each health plan still runs its own credentialing process—including primary source verification, committee review, and contract execution. You must separately apply to each payer for network enrollment.
This is one of the most common misconceptions. Your CAQH profile accelerates the process by eliminating redundant paperwork, but it does not replace payer-specific enrollment applications. Qualigenix’s medical credentialing services manage both the CAQH profile and the individual payer applications in parallel to compress timelines.
What Is the Difference Between CAQH and PECOS?
Providers frequently confuse CAQH with PECOS (Provider Enrollment, Chain, and Ownership System). They serve different purposes in the credentialing ecosystem:
| Factor | CAQH Provider Data Portal | PECOS (Medicare) |
| What it is | Centralized credentialing data repository for commercial payers | Medicare’s official provider enrollment system |
| Who maintains it | CAQH (nonprofit alliance of health plans) | CMS (Centers for Medicare & Medicaid Services) |
| Required for | Most commercial payer credentialing and enrollment | Medicare enrollment and reimbursement |
| Coverage | 1,000+ commercial health plans across all 50 states | Medicare Parts A and B only |
| Re-attestation | Every 120 days | Revalidation every 3–5 years (per CMS schedule) |
| Enrollment effect | Does NOT enroll providers—only stores data for payer access | Directly enrolls providers in Medicare |
| Cost to providers | Free | Free |
| Relationship | Separate from Medicare—CAQH data doesn’t flow to PECOS |
Separate from CAQH—PECOS data does not flow to CAQH
|
Providers need both: CAQH for commercial insurance credentialing and PECOS for Medicare enrollment. Some Medicaid managed care plans also use CAQH, but state Medicaid fee-for-service programs typically have their own portals. Qualigenix manages all three tracks—CAQH, PECOS, and state Medicaid—through our medical credentialing services and recredentialing services.
What Information Does CAQH Require in Your Provider Profile?
The CAQH Provider Data Portal collects comprehensive professional data. Here are the major sections:
Personal demographics: Legal name, date of birth, SSN, NPI, gender, contact information
Education and training: Medical/professional school, residency, fellowship, internship—with dates, institution names, and addresses
Licensure: All current state licenses with license numbers, issue dates, and expiration dates
Board certifications: Certifying board, specialty, certification dates, and recertification schedule
DEA registration: DEA number, state, schedule authorization, and expiration date
Work history: Current and past practice locations, employment history (typically 5–10 years)
Hospital privileges: All current and past hospital affiliations, privilege status, and any restrictions or limitations
Malpractice history: All claims, suits, settlements, and judgments—even if resolved in the provider’s favor
Professional liability insurance: Current carrier, policy number, coverage amounts, and expiration date
Practice information: Office locations, hours, accessibility, languages spoken, accepting new patients status
Disclosure questions: Sanctions, disciplinary actions, loss of privileges, criminal history, substance abuse history
What Happens If Your CAQH Profile Expires?
If you miss the 120-day re-attestation deadline, your CAQH profile status changes to “Expired” or “Not Current.” Payers can no longer access your data, which may trigger claim denials for services rendered during the lapsed period, hold credentialing applications, or initiate network termination proceedings. Some payers treat an expired attestation as a voluntary withdrawal from the network.
The fix is straightforward—log in, review your data, update any changes, and re-attest. But the downstream revenue impact of even a brief lapse can be significant. Set automated reminders 2–3 weeks before every 120-day deadline.
What Are the Most Common CAQH Profile Mistakes That Delay Credentialing?
These errors account for the majority of CAQH-related enrollment delays:
Missing the 120-day re-attestation: The single most common mistake. Your profile goes to “Expired” status, payers lose access, and claims start getting denied. Set calendar reminders or use credentialing software with automated alerts.
Incomplete profile sections: Leaving any mandatory field blank (marked with red asterisks in the portal) prevents payers from pulling your data. Common gaps include missing malpractice history, incomplete work history, and expired documents.
Expired uploaded documents: Uploading a medical license or DEA certificate that has already expired flags your profile for review and pauses processing. Always check expiration dates before uploading.
Data mismatches across systems: Your CAQH name, NPI, and license details must exactly match your NPPES registry, your state license, and your payer applications. Even minor discrepancies (e.g., middle initial vs. full middle name) cause primary source verification failures.
Forgetting to authorize payers: Your profile can be 100% complete, but if you haven’t authorized specific payers to access it, they can’t pull your data. Review your authorization list whenever you apply to a new plan.
Archiving practice locations prematurely: Removing a practice location from your CAQH profile signals to payers that you’ve left that location—which can trigger de-credentialing for that site. Never archive a location without confirming the impact with your credentialing team.
Is CAQH Required for All Healthcare Providers?
CAQH is not federally mandated, but it is functionally required for most providers seeking commercial insurance credentialing. The vast majority of commercial health plans—including UnitedHealthcare, Aetna, Cigna, Humana, BCBS, and their regional affiliates—require an active CAQH profile as a prerequisite for network enrollment. CAQH is free for providers to use. Medicare uses PECOS instead, and some state Medicaid programs have their own portals.
How Does Qualigenix Streamline CAQH Credentialing and Payer Enrollment?
Managing CAQH profiles, tracking attestation deadlines, and coordinating with dozens of payers simultaneously is a full-time job. That’s why providers across 38+ specialties trust Qualigenix to handle the entire credentialing lifecycle.
Complete CAQH profile setup: Our credentialing team creates your CAQH profile from scratch, ensuring every section is complete, every document is current, and every authorization is set before submission.
120-day attestation management: We track every provider’s attestation deadline and re-attest on schedule—no lapses, no expired profiles, no claim denials from missed deadlines.
Parallel payer enrollment: While CAQH is being processed, we simultaneously submit applications to individual payers—compressing the total time from CAQH completion to first billable claim. Our 6-day average onboarding reflects this parallel approach.
Primary source verification coordination: We proactively follow up with licensing boards, medical schools, and certification bodies to ensure verification responses don’t become bottlenecks.
PECOS and Medicaid enrollment: Our Medicare revalidation services and Medicaid enrollment support cover the full spectrum—not just commercial plans.
Recredentialing management: Our recredentialing services handle payer recredentialing cycles every 2–3 years, ensuring you never lose network status due to missed renewal deadlines.
| “Seamless and stress-free credentialing… saved valuable time.”
— Abdul M., Orion Home Health |
| “Game-changer… tailored solutions that streamlined our operations.”
— Dr. Martha H., DPM |
| “Within months, our outstanding balances decreased, and we finally had visibility and control over our revenue.”
— Jennifer H., CNP |
CAQH Profile Maintenance Checklist for Providers
Use this checklist to keep your CAQH profile compliant and avoid credentialing delays:
- CAQH ID obtained: Self-registration completed at proview.caqh.org and unique CAQH ID received
- Profile 100% complete: All mandatory fields filled (no red asterisks remaining) across all sections
- Documents current: Medical license, DEA, board certs, malpractice insurance all uploaded with valid expiration dates
- Data matches across systems: Name, NPI, and license details match NPPES, state licensing board, and payer applications exactly
- Payer authorizations set: All target health plans authorized to access your CAQH data
- Attestation current: Re-attestation completed within the 120-day window (180 days for Illinois providers)
- Reminders set: Automated alerts configured 2–3 weeks before each 120-day attestation deadline
- Practice locations accurate: All current locations listed; no active locations archived without credentialing team confirmation
- PECOS enrollment separate: Medicare enrollment completed through PECOS independently of CAQH
- Credentialing partner engaged: Professional credentialing services (e.g., Qualigenix) managing ongoing profile maintenance and payer applications
Frequently Asked Questions About CAQH
What does CAQH stand for?
CAQH stands for the Council for Affordable Quality Healthcare. It is a nonprofit alliance of leading U.S. health plans that operates the CAQH Provider Data Portal—a centralized credentialing database used by over 1,000 health plans and containing 4.8 million provider records.
How long does CAQH credentialing take?
Creating your initial CAQH profile takes 1–2 hours if documents are prepared. Profile activation takes 3–10 business days. However, CAQH is only one step—full payer credentialing (including primary source verification and committee review) typically takes 60–120 days per plan. Timely CAQH maintenance can reduce this by up to 40%.
How often do you need to attest in CAQH?
CAQH requires re-attestation every 120 days (approximately every 4 months). Illinois providers have a 180-day window. Missing the deadline changes your profile to “Expired” status, which blocks payer access and can trigger claim denials and enrollment holds.
Is CAQH the same as PECOS?
No. CAQH is used for commercial payer credentialing. PECOS is CMS’s Medicare-specific enrollment system. They are completely separate platforms with no data exchange between them. Providers need both: CAQH for commercial plans and PECOS for Medicare.
Is CAQH free for providers?
Yes. The CAQH Provider Data Portal is free for healthcare providers. Health plans pay CAQH for access to the data. There is no cost to create, maintain, or attest your profile. Third-party credentialing services (like Qualigenix) charge fees for managing the process on your behalf.
What happens if my CAQH profile expires?
If your re-attestation window passes, your profile status changes to “Expired” or “Not Current.” Payers lose access to your data, which can delay or block credentialing, trigger claim denials, and in some cases initiate network termination. Log in, update your information, and re-attest to restore access.
Who needs a CAQH profile?
Most healthcare providers seeking commercial insurance credentialing need a CAQH profile. This includes physicians, nurse practitioners, physician assistants, CRNAs, therapists, registered dietitians, behavioral health providers, respiratory therapists, and many other clinical and allied health professionals. Check with your target payers to confirm their CAQH requirements.
How does Qualigenix help with CAQH?
Qualigenix creates and maintains CAQH profiles, manages 120-day re-attestation cycles, coordinates primary source verification, and runs parallel payer enrollment applications. Our 6-day average onboarding and 99% claim accuracy rate reflect our end-to-end approach to credentialing and revenue cycle management.
Related Qualigenix Resources
Service Pages:
- Medical Credentialing Services
- Recredentialing Services
- Medicare Revalidation Services
- Insurance Eligibility Verification Services
- Medical Billing Outsourcing Services
- Revenue Cycle Management Services
Blog Guides:
- Provider Enrollment Process Step by Step Guide
- What Is the Physician Credentialing Process? Step-by-Step
- How Payer Enrollment Services Speed Credentialing
- Top Provider Enrollment and Credentialing Services (2026)
- Healthcare Billing Process Explained
- What Is Revenue Cycle Management? A Beginner’s Guide
- Best RCM Companies in the USA
Stop Losing Weeks to Credentialing Delays — Book a Free Consultation
Every day your CAQH profile sits incomplete, every missed attestation deadline, and every payer application stuck in queue is revenue your practice isn’t earning. Whether you’re a solo provider setting up CAQH for the first time or a group practice managing hundreds of profiles, Qualigenix has the credentialing infrastructure to get you enrolled faster.
Our team delivers 6-day average onboarding, 99% claim accuracy, and a 95% first-pass acceptance rate. We manage CAQH profiles, PECOS enrollment, and individual payer applications simultaneously—compressing months of credentialing into weeks.


