Category: Guides
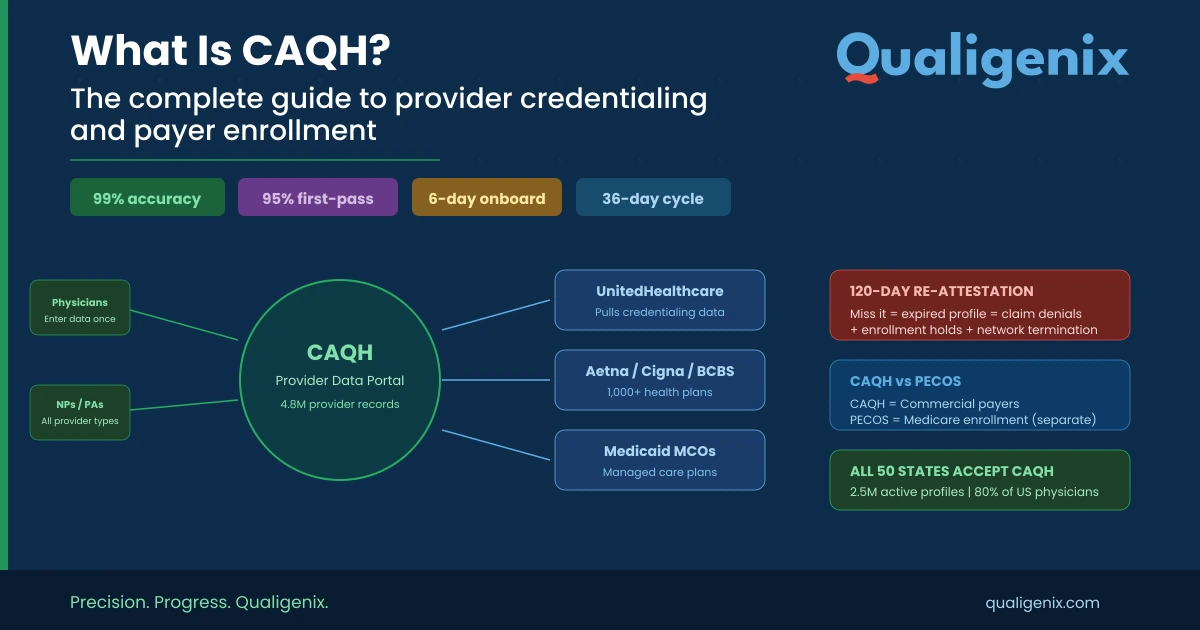
What Is CAQH? The Complete Guide to Provider Credentialing, ProView Setup, and Payer Enrollment
Summary: CAQH (Council for Affordable Quality Healthcare) is a nonprofit that operates the most widely used provider credentialing...

What is the Provider Enrollment Process? Step-by-Step Guide
Ever wonder why claims sit unpaid even after credentialing is complete? In many cases, the real bottleneck is the...

How to Appeal an Insurance Claim Denial: Step-by-Step Guide
A provider treats a patient, documents the visit carefully, and submits a clean claim. Two weeks later, the payer...

Prior Authorization in Healthcare: How to Reduce Delays
Prior authorization in healthcare has become one of the biggest operational challenges that providers face today. What was once...

Revenue Integrity in Healthcare: 8 Key Components Explained
A patient completes a procedure and leaves satisfied, yet the payment never arrives because the service was documented incorrectly....

Home Health Billing Guidelines: Complete Compliance Guide 2026
Home health agencies are functioning in an environment of unprecedented scrutiny. Medicare audits are on the rise, documentation reviews...

DME Revenue Cycle Management: All You Need to Know (2026)
Durable Medical Equipment (DME) billing is among the most complex and tightly controlled areas of the healthcare revenue cycle...

What Is the Denial Management Process? 5 Steps That Are a Must
Claim denials are no longer an occasional interruption in the process of medical billing. In 2026, they are a...

What is the Physician Credentialing Process? Step-by-Step
Every day a physician sits uncredentialed is a day of lost appointments, delayed payments, and growing frustration for your...