Revenue Integrity in Healthcare: 8 Key Components Explained
The Qualigenix Editorial Team comprises certified medical billing professionals, CPC-credentialed coders, prior authorization specialists, and revenue cycle consultants with more than 40 years of combined hands-on experience serving solo physicians, group practices, hospitals, and ASCs across 38+ specialties in the United States. Every guide, article, and resource published on the Qualigenix blog is researched against current CMS guidelines, Federal Register notices, AMA policy updates, and payer-specific billing rules — and reviewed for compliance accuracy before publication. Our content reflects the same standards we apply to our client work: 99% claim accuracy, 95% first-pass acceptance, and a 30% average reduction in AR days.

A patient completes a procedure and leaves satisfied, yet the payment never arrives because the service was documented incorrectly. This scenario happens every day across healthcare systems. Payers now apply tighter audits and stricter reimbursement reviews, while operating margins continue to shrink. These pressures explain why revenue integrity in healthcare has become a critical operational discipline. Healthcare revenue integrity ensures that each service provided is captured accurately, coded with compliance, and billed under financial compliance healthcare standards. Strong charge capture accuracy prevents missed revenue.
Clinical documentation improvement supports coding compliance and payer reimbursement accuracy. When revenue cycle controls are applied at the point of care, organisations prevent revenue leakage and protect long term financial stability.
What Is Revenue Integrity in Healthcare?
Revenue integrity in healthcare acts as the bridge between patient care and payment accuracy. Imagine a hospital visit where a diagnostic test is performed, documented clearly by the clinician, coded correctly by the billing team, and submitted with full compliance. The claim moves smoothly through payer systems and reimbursement arrives without delay. This is the core purpose of revenue integrity. It aligns clinical documentation improvement, coding compliance, and billing compliance controls to protect payer reimbursement accuracy.
The framework also reduces undercoding risks and overcoding risks, which often trigger audits and payment disputes. Revenue integrity does not wait for denials to appear. It works upstream to protect revenue before money is lost.
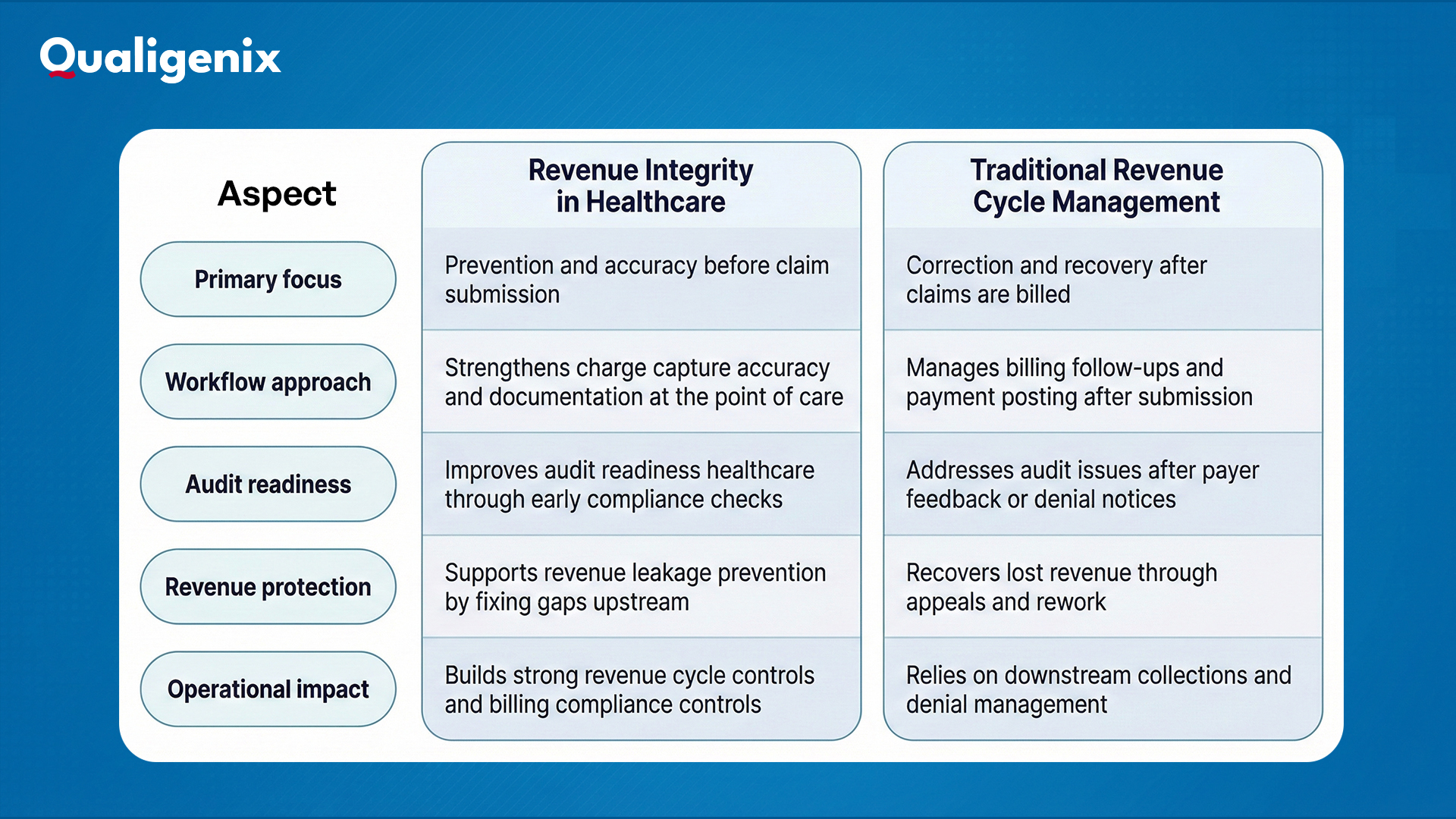
Revenue Integrity vs Traditional Revenue Cycle Management
The table below highlights the key operational differences between revenue integrity in healthcare and traditional revenue cycle management.
Why Healthcare Revenue Integrity Matters in 2026
Payers in the United States now use advanced claim analytics and real time audits to monitor billing behavior. Value based care contracts also tie payment to documentation quality and clinical accuracy. At the same time, labor costs and supply expenses continue to rise, which puts pressure on operating margins. These trends explain why healthcare revenue integrity has become a leadership priority in 2026. Strong revenue cycle controls protect payer reimbursement accuracy and support audit readiness in healthcare. Organizations that focus on prevention reduce revenue leakage and strengthen financial compliance in healthcare. This approach creates stable cash flow and long term sustainability.
Financial and Compliance Risks of Poor Revenue Integrity
The most common financial and compliance risks of poor revenue integrity are as follows:
Undercoding and Missed Revenue
A provider delivers complex care but documents limited details. Coding teams then assign lower value codes. This creates undercoding risks that reduce reimbursement and weaken charge capture accuracy. The organisation loses earned revenue without noticing the gap.
Overcoding and Audit Exposure
A claim is submitted with unsupported codes. Payers flag the claim and request documentation. Overcoding risks increase audit exposure and lead to payment reversals. These errors damage compliance standing and payer trust.
Denials and Payment Take Backs
Incomplete documentation triggers claim denials. Post payment audits also lead to take backs when billing compliance controls fail. These actions increase rework and delay cash flow.
Revenue Integrity in Healthcare: Eight Key Components Explained
Revenue integrity in healthcare works best when multiple controls operate together. Each component strengthens a different part of the revenue flow. When one control fails, revenue leakage often follows. These eight elements form the foundation of healthcare revenue integrity and protect financial compliance healthcare standards across the care continuum.
1. Accurate Charge Capture
Accurate charge capture ensures that every billable service is recorded without duplication or omission. A nurse administers an injectable medication during an outpatient visit. The service appears in the clinical record but never reaches the billing system. This gap reduces charge capture accuracy and creates hidden revenue loss. Automated charge entry tools and standardized workflows help teams capture services at the point of care.
2. Clinical Documentation Alignment
Provider documentation must clearly support every billed service. A surgeon performs a complex procedure but writes limited operative notes. Coding teams cannot justify the full service level. Clinical documentation improvement programs train providers to document medical decision making, treatment complexity, and patient risk. This alignment protects payer reimbursement accuracy.
3. Coding Accuracy and Compliance
Correct code selection drives compliant billing. Coding teams must apply CPT, ICD, and modifier rules accurately. A coder assigns a procedure code without the required modifier. The claim fails payer edits and delays payment. Strong coding compliance reduces errors and supports billing compliance controls.
4. Medical Necessity Validation
Payers reimburse only services that meet medical necessity criteria. A diagnostic test is ordered without documented clinical justification. The payer denies the claim. Medical necessity validation ensures that diagnoses support procedures and that documentation explains why care was required. This step protects reimbursement approval.
5. Denial Prevention Controls
Denial prevention strategies rely on historical denial data. A clinic notices repeated rejections for missing authorization. The revenue team updates intake workflows and verification steps. These denial prevention strategies reduce repeat errors and improve first pass payment success.
6. Audit Readiness and Monitoring
Internal audits prepare organizations for payer reviews. Compliance teams sample claims and identify documentation gaps before external audits occur. Strong audit readiness healthcare practices reduce takebacks and protect regulatory standing. Continuous monitoring also strengthens revenue cycle controls.
7. Payer Contract and Rule Adherence
Each payer applies different billing rules. A service covered by one insurer may require prior authorization under another plan. Teams must apply payer-specific policies accurately. Proper rule adherence protects payer reimbursement accuracy and limits avoidable denials.
8. Data Governance and Reporting
Revenue integrity depends on clear performance data. Reporting systems track billing accuracy metrics, denial trends, and revenue leakage prevention indicators. Leaders use this data to identify undercoding risks and overcoding risks. Strong data governance improves financial compliance, healthcare outcomes and long term stability.
Common Revenue Integrity Gaps in Healthcare Organizations
Many healthcare systems invest in advanced billing tools but still lose revenue because operational gaps remain unresolved. These breakdowns usually occur at the handoff points between care delivery and revenue teams. When communication weakens or documentation standards vary, even strong revenue cycle controls fail to protect reimbursement accuracy. Two of the most common gaps appear below.
Disconnected Clinical and Billing Teams
A physician completes a complex procedure and documents it in clinical language that billing teams cannot interpret easily. Coders then guess or submit lower level codes to avoid compliance risk. This communication gap reduces charge capture accuracy and increases undercoding risks. Regular collaboration between clinical staff and revenue teams closes this gap and improves healthcare revenue integrity.
Inconsistent Documentation Practices
One provider documents every clinical detail while another uses short generic notes for similar visits. Coding teams face inconsistent data quality. Claims become harder to support during audits. This variability weakens clinical documentation improvement efforts and raises denial risk. Standard documentation templates help restore consistency and financial compliance healthcare standards.
How Revenue Integrity Impacts Cash Flow and AR
Revenue integrity directly shapes how fast money moves through accounts receivable. A clinic strengthens documentation and coding controls before claims are sent. The result is fewer errors and faster payments. Strong integrity creates measurable financial improvements:
- Higher clean claim rates lead to quicker payer acceptance and fewer billing delays.
- Lower denial volumes reduce rework and staff follow-ups.
- Shorter AR cycles improve monthly cash flow and financial predictability.
When teams focus on prevention instead of correction, revenue reaches the organization faster. This approach stabilizes operating budgets and supports long term growth.
How Qualigenix Helps With Revenue Integrity in Healthcare

Qualigenix strengthens revenue integrity in healthcare through targeted controls that prevent revenue loss before claims reach payers. The focus stays on accuracy, compliance, and financial stability.
Documentation Alignment
Qualigenix aligns clinical documentation improvement with coding compliance so billed services reflect provider intent. This improves charge capture accuracy, supports medical necessity validation, and reduces audit risk.
Payer Rule Control
Payer specific billing rules and contract requirements are applied during claim preparation. This protects payer reimbursement accuracy and lowers claim rejection rates.
Denial Prevention
Denial analytics identify recurring billing errors and root causes. Process corrections strengthen revenue cycle controls and reduce repeat denials before submission.
Develop Revenue Integrity Into Daily Operations!
Revenue integrity in healthcare is not a one time audit or a quarterly review. It functions as a continuous control system that protects revenue every day. When organizations embed documentation standards, coding accuracy, and payer rule checks into daily workflows, they reduce payer friction and improve reimbursement reliability. Strong healthcare revenue integrity also supports audit readiness and financial compliance healthcare goals. Teams that focus on prevention avoid costly rework and payment delays. This approach builds stable cash flow and long term operational confidence.
FAQs
1. What does revenue integrity mean in healthcare?
Revenue integrity means aligning clinical documentation, coding, charge capture, and billing processes so services provided are accurately recorded, compliant, and reimbursed without payment delays or compliance risk.
2. How is revenue integrity different from RCM?
Revenue integrity focuses on preventing billing errors before claims are submitted, while traditional revenue cycle management corrects denials and payment issues after claims are already processed.
3. What departments are involved in revenue integrity?
Clinical teams provide documentation, coding teams ensure accuracy, compliance teams monitor regulations, and billing teams apply payer rules. All groups work together to protect reimbursement accuracy.
4. How does revenue integrity reduce denials?
Revenue integrity identifies root causes, such as documentation gaps or authorization errors and fixes them early. This prevents repeat claim failures and improves first pass payment success.
5. Can revenue integrity improve audit outcomes?
Yes. Strong billing compliance controls and documentation standards improve audit readiness healthcare and reduce payment takebacks during payer reviews and regulatory inspections.
6. Is revenue integrity relevant for small practices?
Small practices benefit through standardized workflows, better charge capture accuracy, fewer denials, and stronger cash flow, even without large revenue cycle teams or complex systems.