Medicare Physician Fee Schedule 2026: What Every Practice Must Know
The Qualigenix Editorial Team consists of certified billing and coding experts with over 40 years of experience across 38+ medical specialties. Our content is rigorously researched against CMS, AMA, and payer-specific guidelines to ensure total compliance and accuracy. We apply the same elite standards to our resources as we do our client work, consistently delivering high claim accuracy and significant reductions in AR days.

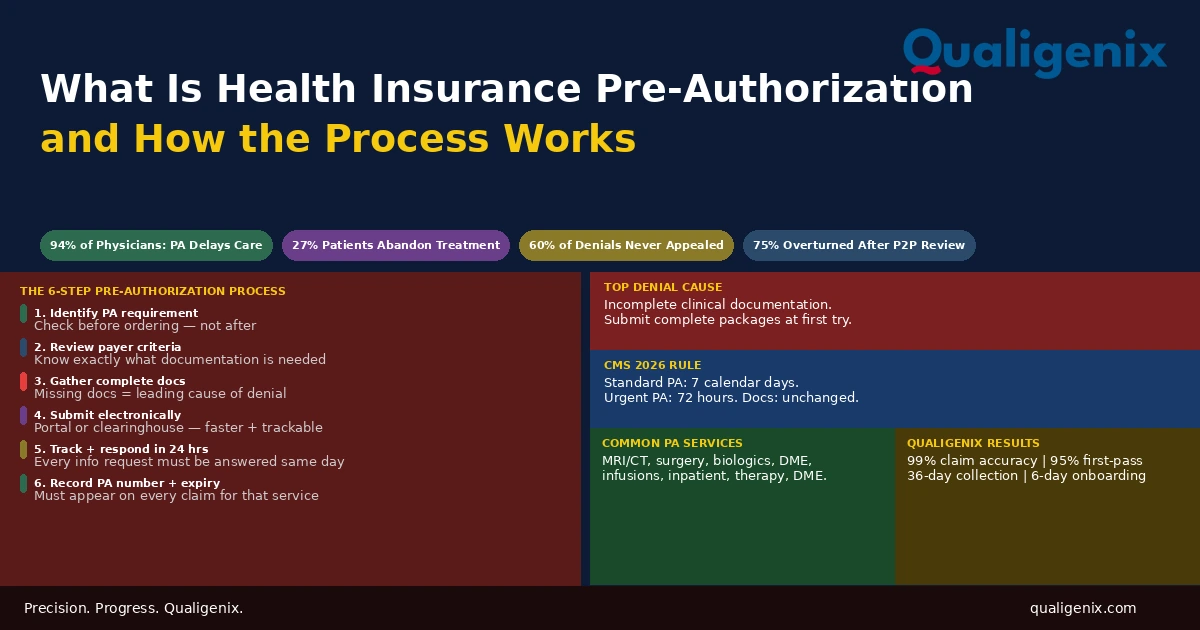
The 2026 Medicare Physician Fee Schedule (CMS-1832-F) introduces two separate conversion factors for the first time: $33.57 for qualifying APM participants and $33.40 for all other providers. A -2.5% efficiency adjustment cuts Work RVUs for surgical, imaging, and procedural codes. Primary care and behavioral health gain ground. Telehealth rules are now permanently expanded. Every practice billing Medicare Part B needs to act on these changes now — they took effect January 1, 2026.
If you bill Medicare Part B, the Physician Fee Schedule controls exactly how much you get paid. It sets the reimbursement rate for nearly every professional service — office visits, surgical procedures, diagnostic imaging, and telehealth consultations. The CY 2026 Medicare Physician Fee Schedule Final Rule (CMS-1832-F) is one of the most significant structural changes to physician payment in recent memory. For the first time, there are two distinct conversion factors. There’s also a -2.5% efficiency cut that will hit certain specialties harder than the headline pay increase suggests.
At Qualigenix, we work with practices across 38+ specialties. What we see consistently is that the practices most affected by fee schedule changes are the ones that weren’t prepared. Charge masters not updated. QPP status not tracked. Telehealth code libraries not expanded. The financial damage compounds quietly — and it’s usually discovered 60–90 days later in an AR review.
This guide breaks down every element of the 2026 MPFS your billing team needs to act on: conversion factors, RVU methodology, the efficiency adjustment, telehealth permanence, QPP changes, and exactly how to protect your revenue cycle before gaps widen.
The 2026 Medicare Physician Fee Schedule sets two conversion factors for the first time: $33.57 for qualifying APM participants (QPs) and $33.40 for non-qualifying providers. A -2.5% Work RVU efficiency adjustment applies to non-time-based procedural codes. Time-based codes — E&M, behavioral health, care management, and telehealth — are fully exempt. All changes are effective January 1, 2026, under CMS-1832-F.
2026 Medicare Physician Fee Schedule — Key Numbers at a Glance
| Metric | Value / Detail |
|---|---|
| CY 2026 QP Conversion Factor | $33.57 (+3.77% from 2025) |
| CY 2026 Non-QP Conversion Factor | $33.40 (+3.26% from 2025) |
| CY 2025 Conversion Factor (single) | $32.35 |
| Efficiency Adjustment (non-time-based Work RVUs) | -2.5% |
| Statutory Pay Increase (One Big Beautiful Bill Act) | 2.5% one-time increase built into 2026 CF |
| QP Statutory Update (MACRA) | 0.75% permanent annual update |
| Non-QP Statutory Update (MACRA) | 0.25% permanent annual update |
| Telehealth Originating Site Fee (2026) | $31.85 (up from $31.01 in 2025) |
| BCA Sequestration (still in effect) | -2% post-adjudication (through FY2032) |
| ASM payment adjustment at launch (2029) | +/-9%, scaling to +/-12% by 2033 |
| CY 2024 Conversion Factor | $33.29 |
| CY 2023 Conversion Factor | $33.07 |
| Qualigenix claim accuracy rate | 99% |
| Qualigenix first-pass acceptance rate | 95% |
| Qualigenix average collection cycle | 36 days |
| Qualigenix average onboarding time | 6 days |
What Is the Medicare Physician Fee Schedule?
The Medicare Physician Fee Schedule is the CMS-administered payment system that reimburses physicians and other healthcare professionals for services covered under Medicare Part B. It’s been governing physician payment since 1992 and covers every enrolled clinician — from private practices and hospital outpatient departments to ASCs, skilled nursing facilities, hospices, and home settings.
The payment formula has three components. Every covered service gets assigned Relative Value Units (RVUs) — standardized scores representing relative work and resource use. Those RVUs are multiplied by a Conversion Factor and adjusted for geographic cost differences using Geographic Practice Cost Indices (GPCIs). The result is your Medicare allowed amount.
CMS updates the schedule every year — new RVU values for specific codes, revised GPCIs, and a new Conversion Factor calculated to keep Medicare Part B spending budget-neutral unless Congress intervenes. In 2026, Congress did intervene, and the result is the most structurally significant update to the fee schedule in years.
The Three RVU Components: What They Are and What Changed
Work RVUs
Work RVUs capture physician effort — preservice time, intraservice time, and postservice follow-up. They make up the largest share of total RVUs for most services. The 2026 rule introduces a -2.5% efficiency adjustment to Work RVUs for non-time-based codes. CMS’s rationale: technology and workflow standardization have made certain procedures faster, but historical payment rates haven’t reflected those productivity gains. The AMA disagrees with this reasoning — and the specialty societies hit hardest have legitimate cause for concern.
Practice Expense RVUs
Practice Expense RVUs reflect the overhead of running a practice: staff salaries, medical supplies, equipment, and facility costs. The 2026 rule finalizes a revised methodology for indirect PE RVUs in facility settings, using auditable OPPS data rather than older AMA survey inputs. For practices in facility settings, this change warrants a close review.
Malpractice RVUs
Malpractice RVUs cover professional liability insurance and vary significantly by specialty. CMS used updated premium data from state insurance rate filings for 2026, maintaining the budget-neutral rescaling framework. These are generally the smallest RVU component, but specialty-specific changes can still affect net payment meaningfully for high-risk procedure categories.
What Changed in the 2026 Medicare Physician Fee Schedule Final Rule
The CY 2026 PFS Final Rule isn’t a routine update. It introduces structural reforms that have been debated for years. Here’s what your billing team needs to understand and act on immediately.
Two Separate Conversion Factors — For the First Time
Starting January 1, 2026, Section 1848(d)(1)(A) of the Social Security Act requires CMS to maintain two distinct Conversion Factors. This stems from MACRA and the One Big Beautiful Bill Act (OBBBA, H.R. 1):
- Qualifying APM Conversion Factor: $33.57. Applies to clinicians who meet the threshold requirements for Advanced Alternative Payment Model participation (QPs). This is a 3.77% increase over the 2025 CF of $32.35.
- Non-Qualifying APM Conversion Factor: $33.40. Applies to all other enrolled clinicians — the majority of independent practices. A 3.26% increase over the 2025 CF.
The $0.17 difference per allowed unit sounds small. Multiply it across thousands of claims annually and the cumulative revenue gap compounds fast. If your practice isn’t currently tracking QPP participation status, that audit needs to happen now.
How is the 2026 conversion factor calculated?
CMS applies a budget neutrality requirement mandated by statute — any RVU increases for specific codes must be offset elsewhere to keep total Part B spending flat. The 2026 CF increase reflects a statutory 2.5% increase from the One Big Beautiful Bill Act, a 0.75%/0.25% MACRA update depending on QP status, and a +0.49% budget neutrality adjustment for Work RVU changes. Note that the 2% BCA sequestration is applied post-adjudication and isn’t reflected in the CF figure itself.
The -2.5% Efficiency Adjustment: Who Gets Hit
This is the provision drawing the sharpest pushback from specialty societies. CMS finalized a -2.5% efficiency adjustment to Work RVUs for non-time-based services. The affected categories are: surgical procedures, diagnostic imaging interpretation, outpatient interventional services, interventional pain management, and orthopedic procedures.
Time-based codes are fully exempt: E&M services, care management, behavioral health, services on the Medicare Telehealth Services List, and maternity codes with a global MMM period are all protected.
Watch out for this: For specialties like interventional radiology, orthopedics, and pain management, the -2.5% efficiency reduction can fully or partially offset the headline 3.26% CF increase. The net effect for high-volume procedure specialties may be a payment decrease, not an increase — even before sequestration is applied. Run a specialty-specific impact model before assuming the 2026 update is favorable for your practice.
Primary Care and Behavioral Health Get a Boost
CMS is explicitly repositioning this rule as a shift toward preventive, primary care-centered health. Behavioral health integration services, chronic care management add-ons, and advanced primary care management codes get favorable treatment in 2026. New behavioral health integration and psychiatric collaborative care management add-on services are now included in the definition of primary care services for MSSP beneficiary assignment — which means they count toward shared savings calculations in ways they didn’t before.
A new Ambulatory Specialty Model (ASM) also launches in January 2027, targeting heart failure and low back pain care. Payment adjustments run from -9% to +9% at launch (scaling to +/-12% by 2033). Practices serving these patient populations should review their data and clinical workflows now — before the model takes effect.
Telehealth Expansions Are Now Permanent
Several telehealth flexibilities that started during the COVID-19 public health emergency are now permanently codified. These changes provide the billing stability needed to build sustainable telehealth revenue lines:
- Direct supervision via real-time audio/video: Permanently allowed — no in-person presence of the supervising physician required.
- Teaching physician virtual presence: Permanently adopted for billing services involving residents across all teaching settings.
- Frequency limits removed: Subsequent inpatient visits, subsequent nursing facility visits, and critical care consultations no longer have frequency limitations.
- Telehealth Originating Site Fee: Increased to $31.85 for CY 2026 (from $31.01 in 2025).
- Rural Health Clinics and FQHCs: Extended ability to bill for telehealth services through 2026.
Conversion Factor Comparison: 2023–2026
| Factor | CY 2023 | CY 2024 | CY 2025 | CY 2026 |
|---|---|---|---|---|
| Conversion Factor (Non-QP) | $33.07 | $33.29 | $32.35 | $33.40 |
| QP Conversion Factor | N/A | N/A | N/A | $33.57 |
| Efficiency Adjustment | None | None | None | -2.5% (non-time-based) |
| Congressional Intervention | Yes (CARES Act) | Yes (Consol. Approps.) | Partial | Yes (OBBBA H.R. 1) |
How the 2026 MPFS Changes Your Revenue Cycle
Fee schedule changes don’t operate in isolation. They cascade through every layer of your RCM — charge capture, coding accuracy, claim submission, payer adjudication, and AR management. Here’s where the 2026 changes create specific billing risks and opportunities.
Charge Capture Risk From the Efficiency Adjustment
The -2.5% Work RVU reduction applies at the code level, not the claim level. If your charge master hasn’t been updated to reflect 2026 RVU values for affected procedure codes, you’re billing based on inflated expected payments — and variance reports later in the year will be an unpleasant surprise. Every CPT code in your surgical, imaging, and procedural lines needs to be revalidated against the 2026 PFS RVU database.
Coding Accuracy With Dual Conversion Factors
For the first time, a clinician’s QP status determines which CF applies to every single claim they submit. If your billing system doesn’t correctly identify and flag QP vs. non-QP providers, you risk either under-billing or creating compliance exposure. This requires a coordinated update across credentialing, billing system configuration, and QPP tracking workflow. It’s not a billing-team-only fix.
Does the efficiency adjustment apply to every practice?
No. The -2.5% adjustment applies only to non-time-based services and only to Work RVUs — not Practice Expense or Malpractice RVUs. Time-based codes (E&M, behavioral health, care management, telehealth) are fully exempt. Primary care-focused practices will feel minimal impact. The sharpest pain falls on high-volume surgical specialties and procedure-heavy outpatient practices.
Telehealth Billing Expansion Creates Untapped Revenue
Permanent removal of frequency limits for subsequent inpatient and nursing facility visits opens a significant revenue opportunity for hospitalists, intensivists, and SNF-affiliated practices. If your billing workflow hasn’t been updated to support telehealth variants of these codes, you’re leaving reimbursable encounters uncaptured. Qualigenix’s RCM team regularly identifies 8–12% revenue uplift just from telehealth code optimization when onboarding new clients who haven’t updated their telehealth billing libraries.
2026 Medicare Physician Fee Schedule Compliance Checklist
Use this 10-step checklist to confirm your practice is operationally ready for the 2026 MPFS changes:
- ☐ Audit QPP participation status: Confirm whether each enrolled provider qualifies as QP or non-QP for 2026 — the correct CF ($33.57 vs. $33.40) must be applied to every claim
- ☐ Update charge master: Revalidate all CPT codes against 2026 PFS RVU values, especially for surgical, imaging, and procedural services affected by the efficiency adjustment
- ☐ Configure billing system for dual CFs: Your billing software must distinguish QP vs. non-QP providers for correct claim adjudication
- ☐ Review E&M coding accuracy: E&M codes are exempt from the efficiency adjustment — ensure coders are capturing the correct service level to maximize allowed amounts
- ☐ Expand telehealth billing workflows: Update code libraries for permanent telehealth additions and remove frequency-limit flags from subsequent inpatient and SNF visit codes
- ☐ Audit behavioral health integration codes: New add-on codes for behavioral health and psychiatric collaborative care management now count toward MSSP primary care definitions
- ☐ Review GPCI adjustments: CMS updated GPCIs for 2026 — confirm geographic locality settings are current in your practice management system
- ☐ Brief clinical staff on documentation: The efficiency adjustment shouldn’t change documentation completeness — maintain full clinical documentation for every encounter
- ☐ Run a specialty-specific impact model: Use 2026 PFS RVU data to model projected payment changes for your top 20 CPT codes by volume before assuming the update is positive
- ☐ Engage an RCM partner for a free AR assessment: Quantify where fee schedule gaps are costing your practice before they compound through the year
How Qualigenix Helps Practices Manage Medicare Fee Schedule Changes
Fee schedule updates aren’t a one-time event — they’re an annual disruption cycle that requires proactive RCM infrastructure to manage without losing revenue. At Qualigenix, we’ve built our entire service model around anticipating these changes before a single claim is filed incorrectly.
When CMS issues a final rule in October, our team models the impact on every specialty we serve and begins updating client billing systems before January 1. That’s why our 99% claim accuracy rate and 95% first-pass acceptance rate hold year over year — including through structural changes like the 2026 dual CF introduction.
Here’s what we bring to this specific update:
- Medical Coding Services: Our specialty-trained coding team ensures every CPT code is assigned at the correct 2026 RVU value with documentation supporting the level of service claimed. We handle the charge master revalidation so your team doesn’t have to.
- Charge Entry Services: We configure charge capture workflows to reflect 2026 RVU changes and QP status flags — so the right CF is applied to every claim from day one.
- Denial Management Services: Fee schedule transitions are a leading cause of claim edits and denials. Our denial team catches and resolves these issues at the payer level — not 90 days later in your AR aging report.
- Healthcare Performance Reporting: Our analytics dashboards track conversion factor shifts, payer mix performance, and AR aging in real time. You always know where you stand.
- AR Follow-Up Services: Our dedicated AR team monitors outstanding Medicare claims and follows up proactively on adjudication issues tied to fee schedule mismatches.
How quickly can Qualigenix update a practice’s billing workflows for the 2026 MPFS changes?
We onboard new clients in as few as 6 days, beginning with a comprehensive AR assessment that quantifies exactly where the 2026 fee schedule is affecting your specific payer mix and specialty profile. Billing system updates for dual CF configuration and charge master revalidation are completed during onboarding — before the first claim under the new structure is filed.
Frequently Asked Questions: Medicare Physician Fee Schedule 2026
What is the 2026 Medicare Physician Fee Schedule conversion factor?
There are two for 2026: $33.57 for qualifying Alternative Payment Model participants (QPs) and $33.40 for all other enrolled clinicians (non-QPs). This is the first year CMS has maintained two separate CFs by statute, stemming from MACRA and the One Big Beautiful Bill Act. The QP rate is a 3.77% increase and the non-QP rate is a 3.26% increase from the 2025 CF of $32.35.
Who is exempt from the -2.5% efficiency adjustment?
All time-based codes are exempt: E&M services, care management, behavioral health services, services on the Medicare Telehealth Services List, and maternity codes with a global MMM period. The -2.5% applies only to non-time-based procedural codes — surgical procedures, diagnostic imaging, outpatient interventions, and interventional pain management.
Does Medicare sequestration still apply on top of the new conversion factors?
Yes. The 2% Budget Control Act sequestration reduction stays in effect through FY2032 and is applied post-adjudication, after all other reductions. The CF figures in the 2026 final rule don’t include sequestration. A potential additional PAYGO sequestration of up to 4% was waived by Congress in November 2025 but may return in future legislative cycles.
When do the 2026 Medicare Physician Fee Schedule changes take effect?
All provisions of CMS-1832-F took effect January 1, 2026, for dates of service on or after that date. The dual conversion factor structure, efficiency adjustments, telehealth permanence provisions, and QPP updates all apply to claims billed for services rendered from January 1, 2026 forward.
What is a Relative Value Unit (RVU) and why does it matter?
An RVU is the standardized measure of relative work and resource use assigned to each CPT-coded service. Work RVUs capture physician effort; Practice Expense RVUs cover overhead; Malpractice RVUs cover liability insurance costs. Total RVUs multiplied by the conversion factor and GPCI equal your Medicare allowed amount. Changes to RVUs — including the 2026 efficiency adjustment — directly change your reimbursement per claim, independent of the CF update.
How does the 2026 MPFS affect small independent practices?
Independent practices face dual pressure. The -2.5% efficiency adjustment hits procedure-heavy specialties hard, while practice expense methodology changes may not fully capture the real overhead costs of running an independent office. The AMA has flagged that independent practices are especially vulnerable at a time of rising input costs and increasing consolidation pressure. Proactive charge master updates, QPP status audits, and real-time denial monitoring are critical for independent financial stability in 2026.
What telehealth changes are permanent in the 2026 MPFS?
The 2026 rule permanently codifies: direct supervision via real-time audio/video (no in-person supervising physician required), teaching physician virtual presence for resident billing across all teaching settings, and removal of frequency limits on subsequent inpatient visits, subsequent nursing facility visits, and critical care consultations. The telehealth originating site fee increased to $31.85 for CY 2026.
What is the Ambulatory Specialty Model launching in 2027?
The ASM is a new mandatory Alternative Payment Model finalized in the 2026 PFS rule. It launches January 2027, targets heart failure and low back pain care, and runs for five years. Payment adjustments start in 2029 at +/-9%, scaling to +/-12% by 2033. Practices serving patients in these care categories should start reviewing their clinical workflows and outcome data now.
Related Qualigenix Resources
Service Pages:
- Medical Coding Services
- Charge Entry Services
- Denial Management Services
- AR Follow-Up Services
- Healthcare Performance Reporting
- Medical Accounts Receivable Services
- Revenue Cycle Management Services
Blog Guides:
- What Are RCM KPIs — The Metrics That Actually Matter
- Revenue Cycle Management Trends 2026
- How to Reduce Medical Claim Denials: Your 2025 Guide
- Outpatient Coding for High-Volume Practices: Keeping Accuracy at Scale
- Denial Management in Medical Billing: 7 Common Causes
Ready to Protect Your Medicare Revenue in 2026?
The 2026 Medicare Physician Fee Schedule is already in effect. Practices that haven’t updated their charge masters, configured dual CF workflows, and expanded telehealth billing are losing money right now. Qualigenix offers a free AR assessment that quantifies exactly where your revenue gaps are — and closes them fast.
Our team delivers 99% claim accuracy, a 95% first-pass acceptance rate, a 30% reduction in AR days, and an average 36-day collection cycle. We onboard in as few as 6 days.
Precision. Progress. Qualigenix.