CAQH Credentialing and Payer Enrollment: How One Expired Profile Blocks Every Application Behind It
The Qualigenix Editorial Team consists of certified billing and coding experts with over 40 years of experience across 38+ medical specialties. Our content is rigorously researched against CMS, AMA, and payer-specific guidelines to ensure total compliance and accuracy. We apply the same elite standards to our resources as we do our client work, consistently delivering high claim accuracy and significant reductions in AR days.
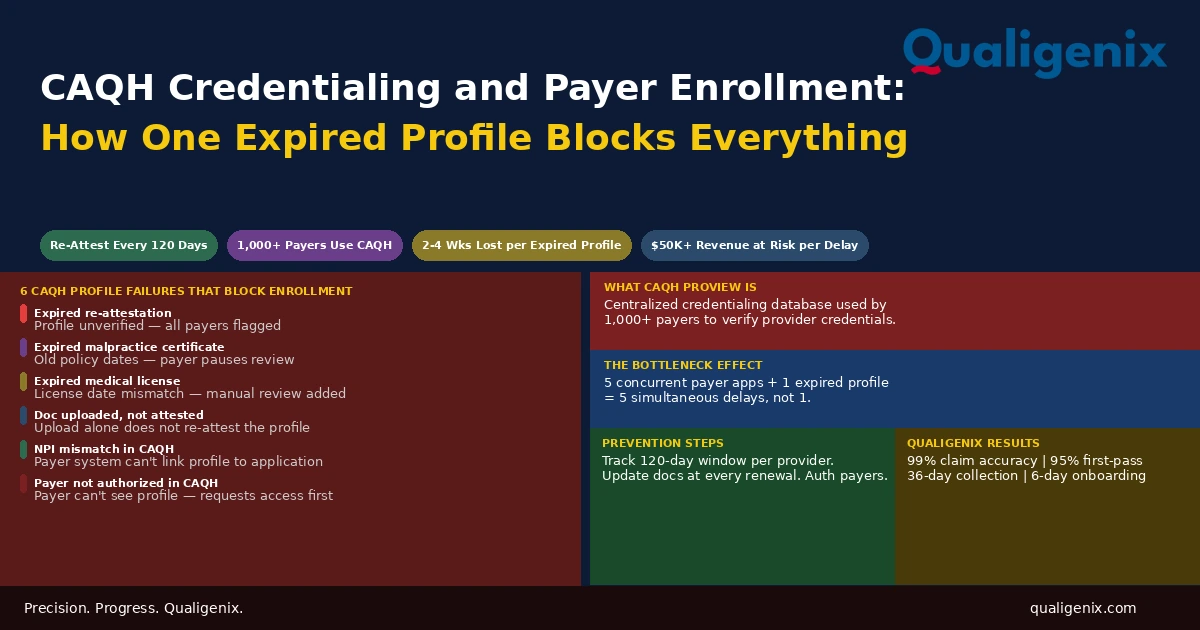
CAQH credentialing is the process of building and maintaining a provider’s profile in the CAQH ProView database, which over 1,000 commercial payers use to verify credentials during enrollment and recredentialing reviews. A profile that is expired, incomplete, or contains an outdated document doesn’t just slow the application in progress. It blocks every payer application that depends on it until the provider updates and re-attests. The delay costs practices weeks of enrollment time and, depending on the provider’s patient volume, tens of thousands of dollars in revenue that can’t be recovered.
Most practices understand that provider credentialing takes time. What fewer practices understand is that a significant portion of that time isn’t spent on payer review. It’s spent waiting for a CAQH profile issue to be identified, communicated to the practice, corrected by the provider, and re-verified before the payer resumes review. That waiting period is silent. The application isn’t denied. It isn’t progressing. It’s simply sitting in a queue because the CAQH data the payer needed to move forward wasn’t there when they looked.
CAQH ProView was designed to eliminate credentialing paperwork duplication. One profile, maintained in one place, accessible to every participating payer. In practices where the profile is current and well-maintained, it delivers exactly that efficiency. In practices where it isn’t, it becomes the bottleneck that delays every enrollment application running through it simultaneously.
This blog explains what CAQH credentialing is, how payers use it during enrollment, what causes profiles to fail at exactly the wrong moment, and what it costs when the problem surfaces during a live enrollment application rather than before it was submitted.
CAQH credentialing is the process of building and maintaining a provider’s profile in the CAQH ProView database so that participating insurance payers can verify the provider’s qualifications during enrollment and recredentialing reviews. The profile must be fully completed, contain current non-expired documents, and be re-attested every 120 days. An expired or incomplete CAQH profile delays every payer enrollment application that queries it, adding two to four weeks to each affected timeline.
CAQH Credentialing and Payer Enrollment: Key Numbers
| Metric | Data Point | Source |
|---|---|---|
| CAQH re-attestation requirement | Every 120 days | CAQH ProView requirements |
| Health plans and hospital systems using CAQH ProView | Over 1,000 | CAQH Index Report |
| Providers registered in CAQH ProView | Over 2 million | CAQH ProView data |
| Weeks added to enrollment by expired CAQH profile | 2 to 4 weeks per affected application | Credentialing operations benchmarks |
| Commercial payer enrollment timeline | 90 to 120 days | Payer credentialing benchmarks |
| Time to build a complete new CAQH profile | 1 to 2 weeks | Credentialing operations data |
| Revenue lost per enrollment delay month | $15,000 to $60,000+ depending on specialty | Practice revenue benchmarks |
| Most common expired document in CAQH profiles | Malpractice insurance certificate | Credentialing audit data |
| Multi-provider practices with at least one expired profile | Estimated 25% to 35% at any given time | Healthcare credentialing surveys |
| Days between profile expiration and practice awareness | Typically 14 to 30 days | Credentialing workflow studies |
| Qualigenix first-pass acceptance rate | 95% | Qualigenix performance data |
| Qualigenix claim accuracy rate | 99% | Qualigenix performance data |
| Qualigenix average collection cycle | 36 days | Qualigenix performance data |
| Qualigenix client onboarding time | 6 days | Qualigenix operations data |
What CAQH Credentialing Actually Is
CAQH ProView is a centralized credentialing data repository operated by the Council for Affordable Quality Healthcare, a non-profit alliance whose membership includes most of the major commercial health plans operating in the United States. The system was built to solve a specific and costly inefficiency: every time a provider sought enrollment with a new payer or went through recredentialing, they had to submit the same documentation to every payer separately. The same license copies, the same malpractice certificates, the same work history forms, all submitted individually to each payer’s credentialing department.
CAQH ProView consolidates this. The provider builds one profile containing all their credentialing information, uploads their supporting documents, and authorizes each payer to query the database. When a payer initiates a credentialing review, they pull the provider’s CAQH data directly rather than requesting documents from the practice. The practice doesn’t have to send the same documents ten times. The payer doesn’t have to manage ten separate document collections. The efficiency only exists when the profile is current.
CAQH ProView is not a credentialing authority. It does not approve or deny provider applications. It is a data infrastructure that payers use to access provider qualification information quickly. Its value to both providers and payers depends entirely on the accuracy and currency of the data in it. A profile that is technically in CAQH but contains expired documents or unattested information provides no efficiency benefit and actively delays the applications that depend on it.
Over 1,000 health plans and hospital systems participate in CAQH ProView. For most commercial payer enrollments, a CAQH profile is not optional. It is the mechanism through which the payer conducts their review. A provider without a CAQH profile, or with a profile in a state the payer can’t use, will be asked to build or correct it before enrollment can proceed regardless of how complete the rest of their application is.
How Payers Use CAQH During Enrollment and Recredentialing
When a provider submits a credentialing or enrollment application to a participating payer, the payer’s credentialing team queries CAQH ProView as part of their review process. They’re looking for the provider’s current license, DEA registration, malpractice insurance, board certifications, work history, and attestation answers. If the profile is complete, current, and attested, the payer can proceed with their review using the CAQH data as a verified source.
The payer’s use of CAQH data varies slightly by organization. Some payers use CAQH as their primary verification source and proceed through their review using only CAQH data. Others use CAQH as a starting point and request supplemental documentation for specific items they want to verify independently. Most conduct primary source verification, confirming the medical license directly with the state licensing board and the DEA registration directly with the DEA, using CAQH as the reference that initiates those checks.
For recredentialing specifically, payers typically run an updated CAQH query at the start of the renewal review to confirm the provider’s credentials are still current. If the profile has expired since the last credentialing cycle, the recredentialing review cannot proceed using stale data. The payer sends a notification requesting profile update, and the recredentialing clock pauses while waiting for the provider to re-attest.
The 120-Day Re-attestation Requirement: The Most Missed Deadline in Credentialing
CAQH requires providers to re-attest their profile every 120 days. Re-attestation is the act of logging into CAQH ProView, reviewing all profile sections and uploaded documents for accuracy, and confirming that the information is current. It resets the 120-day clock. If re-attestation doesn’t happen before the 120-day window closes, the profile status changes from Active to Expired.
An expired profile doesn’t mean the data disappears. It means the data is no longer certified as current by the provider. Payers querying an expired profile see the expiration flag and treat the data as unverified. For an enrollment in progress, the payer contacts the practice requesting re-attestation. For a recredentialing review, the payer pauses the review pending profile update. In both cases, the application timeline extends by the time it takes the practice to identify the issue, contact the provider, have them log in and re-attest, and confirm the updated profile status with the payer.
Warning: CAQH sends re-attestation reminders to the email address on file in the provider’s CAQH account. If that email address is the provider’s personal email rather than a practice administrative email, the reminder may never reach the team responsible for managing credentialing. Practices should confirm that their credentialing coordinator’s email is listed as an additional contact on each provider’s CAQH account so that re-attestation reminders reach the right person, not an inbox the provider checks once a week.
For practices with a single provider, the 120-day window is a manageable calendar event. For practices with 10 or 15 providers, each with their own CAQH account on their own re-attestation cycle, the windows are staggered across the year. One provider re-attests in January. Another in February. Another in April. Without a central tracker that shows every provider’s next re-attestation date, some will lapse without anyone noticing until a payer flags a live application.
What an Expired CAQH Profile Actually Blocks
When a CAQH profile expires, it doesn’t block one thing. It blocks every payer application running through CAQH that involves that provider. This is the distinction most practices miss. The assumption is that a CAQH problem affects one application at a time. In reality, if a practice has a new provider with applications pending at five commercial payers simultaneously, and that provider’s CAQH profile expires during the review period, all five applications encounter the same flag at approximately the same time.
Each payer independently queries CAQH, independently finds the expired profile, and independently sends a request for update. The practice receives five similar requests, must coordinate a single re-attestation action with the provider, confirm the updated profile with each payer separately, and track each application back into active review status. The administrative effort is multiplied by the number of concurrent applications. The delay is multiplied by the same factor.
A 90-to-120-day commercial payer enrollment has the CAQH verification step embedded in its timeline. When CAQH is current at the time of application, the verification step proceeds without delay and the overall timeline holds. When CAQH expires mid-review, the verification step produces a pause that adds time to the back end of the timeline. A four-week delay on a 90-day enrollment becomes a 120-day enrollment. The provider can’t bill as in-network at that payer for those additional four weeks. That revenue is not recoverable once the enrollment completes.
The Six CAQH Profile Failures That Block Payer Enrollment Most Often
Profile expiration from a missed re-attestation is the most common CAQH issue. But several other profile failures produce the same result: a payer unable to complete its verification and an application that stalls. Each has a specific cause and a specific prevention.
1. Expired Malpractice Insurance Certificate
The most frequently expired document in CAQH profiles is the malpractice insurance certificate. Malpractice policies renew annually. The certificate in the CAQH profile reflects the policy that was in force when it was uploaded. If the provider renews their malpractice coverage and doesn’t update the CAQH profile with the new certificate, the profile contains an expired document. Payers verifying malpractice coverage find the old certificate, flag the discrepancy, and pause the review pending an updated certificate upload.
This happens consistently in practices where the administrative team manages billing and operations but isn’t looped into the provider’s annual malpractice renewal. The renewal happens. The new certificate arrives. Nobody uploads it to CAQH. The old certificate sits in the profile until a payer finds it during an enrollment review.
2. Expired Medical License
A medical license that has expired and been renewed by the provider must be updated in CAQH immediately upon renewal. Payers verifying licensure through CAQH see the expiration date on the license in the profile. If that date has passed and the new license hasn’t been uploaded, the payer flags the application. State licensing boards are the primary source verification target for licensure. If CAQH shows an expired license, the primary source check will reflect the current status, but the mismatch between CAQH data and primary source data adds a manual review step that extends the timeline.
3. Profile Not Attested After Document Update
Uploading a new document to CAQH does not automatically re-attest the profile. The provider must separately complete the attestation step confirming the updated profile is accurate. Practices that upload a new malpractice certificate or license renewal but don’t complete the attestation step leave the profile in an incomplete or unattested state. Payers querying an unattested profile encounter the same delay as with an expired profile because the data hasn’t been certified as current by the provider.
4. Missing or Incorrect NPI
The National Provider Identifier in the CAQH profile must match the NPI the practice uses on payer enrollment applications and claims. An NPI discrepancy, whether from a data entry error during profile creation or a change in billing structure that altered which NPI the practice uses, causes the payer’s enrollment system to fail to match the CAQH profile to the application. The mismatch requires manual resolution and pauses automated verification processes.
5. Incomplete Work History
CAQH requires a complete work history covering the past 10 years. Gaps in work history, missing employer addresses or dates, or failure to include all practice locations where the provider currently practices are common profile incompletions. Payers reviewing work history for credentialing purposes may request clarification on gaps or missing entries before proceeding with the application.
6. Payer Authorization Not Granted
This is the CAQH failure that surprises practices most often. A provider builds a complete, fully attested CAQH profile. An enrollment application is submitted to a new payer. The payer queries CAQH and can’t access the profile. The reason is that the provider never authorized that payer to view their data within the CAQH system. CAQH requires explicit per-payer authorization. A profile that authorizes 10 payers is not visible to an 11th payer until the 11th payer is specifically authorized by the provider inside CAQH.
When a practice submits a new enrollment application, confirming that the relevant payer is authorized in CAQH takes two minutes. Discovering it wasn’t authorized after the payer contacts the practice requesting access takes two to three additional weeks of processing time.
The Revenue Cost of CAQH-Driven Enrollment Delays
CAQH profile problems are administrative in nature. The financial impact, however, is clinical-scale. Every week a provider can’t bill a payer as in-network because enrollment hasn’t completed due to a CAQH delay is a week of revenue either lost entirely or billed out-of-network at reduced rates.
For a primary care physician seeing 18 patients per day, with 25% of their panel on a specific commercial payer, a four-week CAQH-driven enrollment delay represents approximately 90 uncompensated or out-of-network encounters at that payer. At an average in-network rate of $150 to $200 per visit, that’s $13,500 to $18,000 in lost or deferred revenue from a single profile issue at a single payer. For a specialist with higher per-visit reimbursement, the number scales proportionally.
The math changes when the CAQH issue affects multiple payers simultaneously, which it does whenever a profile expires during a period when multiple applications are in concurrent review. Four payers, each delayed four weeks, each representing 20% to 30% of the provider’s eventual patient panel, compound the revenue impact significantly. None of this revenue is recoverable once enrollment completes. Payers don’t pay retroactively for the enrollment gap period.
| CAQH Failure Type | How It Surfaces | Delay Added | Prevention |
|---|---|---|---|
| Expired re-attestation | Payer flags profile as unverified mid-review | 2 to 4 weeks | Track 120-day window per provider |
| Expired malpractice certificate | Payer finds old policy dates during verification | 1 to 3 weeks | Upload new certificate at every annual renewal |
| Expired medical license | License date mismatch triggers manual review | 1 to 3 weeks | Update CAQH immediately upon license renewal |
| Document uploaded but not attested | Profile shows incomplete or unattested status | 1 to 2 weeks | Complete attestation step after every upload |
| NPI mismatch | Payer system fails to match profile to application | 2 to 4 weeks | Confirm NPI consistency across all systems |
| Payer not authorized in CAQH | Payer cannot access profile, requests authorization | 2 to 3 weeks | Authorize new payer in CAQH before submitting application |
| Incomplete work history | Payer requests clarification on gaps | 1 to 3 weeks | Complete 10-year work history at profile creation |
CAQH and Medicare Enrollment: What’s Different
CAQH ProView is used by commercial payers. Medicare enrollment runs through a completely separate CMS system called PECOS, the Provider Enrollment, Chain, and Ownership System. A provider’s CAQH profile does not replace or substitute for Medicare enrollment through PECOS. These are parallel processes that must both be completed for a provider to bill both commercial payers and Medicare.
However, the CAQH and PECOS processes should run simultaneously, not sequentially. Practices that complete CAQH first and then start PECOS enrollment add the Medicare timeline on top of the commercial timeline rather than running both in parallel. For a new provider, this means a longer total gap before they can bill any payer in-network. Starting both CAQH profile building and PECOS enrollment on the same day a hire is confirmed is the operational standard that minimizes the billing gap.
CAQH does play an indirect role in Medicare Advantage enrollment. Medicare Advantage plans are administered by private commercial insurers, many of which participate in CAQH. Enrolling with a Medicare Advantage plan follows the commercial payer credentialing process, which means a current CAQH profile is as important for Medicare Advantage enrollment as for any other commercial payer application.
Building a CAQH Profile Maintenance System That Doesn’t Miss the Window
The operational solution to CAQH credentialing failures is not complicated. It requires two things: a tracking system and an owner. Most practices that consistently miss re-attestation deadlines or discover expired documents during live enrollments have neither.
The CAQH Tracking Component
Every active provider needs a CAQH record in the practice’s credentialing tracker that shows the last attestation date, the next re-attestation due date, the expiration dates of each major document in the profile (malpractice certificate, license, DEA registration), and the list of payers currently authorized to access the profile. The tracker generates a reminder 30 days before each re-attestation deadline and 60 days before each document expiration.
This is not a complex system. It can be maintained in a spreadsheet for small practices. For practices with five or more providers, a dedicated credentialing management tool is more reliable. The key requirement is that the tracker is reviewed monthly and the reminders are acted on by someone with both access to CAQH and authority to coordinate with the provider for re-attestation.
The Ownership Component
CAQH profile maintenance must have a named owner in the practice. Not the physician. Not whoever has time that week. A named administrative or credentialing staff member who is responsible for tracking re-attestation windows, coordinating with providers before deadlines, uploading new documents when credentials renew, and confirming payer authorizations when new applications are submitted. Without named ownership, the task drifts and the first signal the practice receives that something went wrong is a payer notice asking about an expired profile on a live application.
How Qualigenix Manages CAQH Credentialing for Practices
At Qualigenix, CAQH profile management is not a separate service from provider credentialing and payer enrollment. It’s built into the same operational process. When a new provider joins a practice we serve, we build their CAQH profile as the first step, before any payer applications are submitted. We confirm every section is complete, every document is current, every payer that needs access is authorized, and the initial attestation is completed before we submit a single application.
We maintain a re-attestation calendar for every active provider across every client. When a provider’s 120-day window approaches, we coordinate with the practice to ensure re-attestation happens before the deadline, not after a payer notices the expiration. When a malpractice certificate renews, we update CAQH. When a license renews, we update CAQH. When a new payer application is submitted, we verify authorization before submission rather than discovering it was missing after the payer requests it.
We also manage the parallel processes: PECOS enrollment for Medicare, payer applications across all commercial payers, and recredentialing renewals. For practices that have been managing credentialing reactively, meaning they respond to payer requests rather than staying ahead of deadlines, we often find multiple CAQH profiles in need of immediate remediation when we onboard a new client. We address these as the first priority because every other credentialing activity depends on them being clean.
Our results reflect a process built on this foundation: 99% claim accuracy rate, 95% first-pass acceptance rate, and an average 36-day collection cycle. We onboard new clients in as few as 6 days.
Related services: CAQH Profile Management | Provider Credentialing | Payer Enrollment | Re-credentialing Services
CAQH Credentialing Health Checklist
- CAQH profile built and fully completed before any payer enrollment applications are submitted
- All profile sections completed including 10-year work history, all practice locations, and attestation questions
- Malpractice insurance certificate in CAQH reflects current policy with non-expired dates
- Medical license in CAQH is current with up-to-date renewal date
- DEA registration in CAQH is current and not expired
- NPI in CAQH matches NPI used on payer applications and claims
- Attestation completed after every document upload or profile update
- Every active payer authorized to access the profile in CAQH settings
- New payers authorized in CAQH before enrollment application is submitted to them
- Re-attestation tracked per provider with 30-day advance reminder before 120-day deadline
- Credentialing team email listed as additional contact on every provider’s CAQH account
- CAQH profile status confirmed Active before submitting any recredentialing application
Frequently Asked Questions: CAQH Credentialing
What is CAQH credentialing?
CAQH credentialing is the process of building and maintaining a provider’s profile in the CAQH ProView database so that participating insurance payers can verify qualifications during enrollment and recredentialing reviews. Over 1,000 health plans use CAQH ProView to access provider data rather than collecting separate documentation from each practice. A complete, attested, and current CAQH profile is a prerequisite for most commercial payer enrollment applications and recredentialing renewals.
What is CAQH ProView?
CAQH ProView is the centralized credentialing database operated by the Council for Affordable Quality Healthcare, used by over 1,000 health plans and hospital systems to retrieve provider qualification data. Providers store their credentials once in CAQH and authorize each payer to query the database during enrollment review. The efficiency gain only exists when the profile is current, complete, and attested. An expired or incomplete profile creates the same delays it was designed to eliminate.
How often does a CAQH profile need to be re-attested?
CAQH requires re-attestation every 120 days. If re-attestation is not completed within that window, the profile status changes to expired and any payer querying it during a live enrollment review will flag the application for update. In multi-provider practices, each provider has their own 120-day window on their own cycle. Without a central tracker showing every provider’s next re-attestation date, some will expire without anyone noticing until a payer flags a live application.
What happens when a CAQH profile expires?
When a CAQH profile expires, payers querying it during credentialing or recredentialing review find unverified data and flag the application for follow-up, adding two to four weeks to the processing timeline per affected payer. The profile data isn’t deleted. It’s no longer certified as current. Every payer with a live application depending on that profile sends an independent request for re-attestation. The practice must coordinate re-attestation and confirm updated status with each payer separately before review resumes.
What information must be in a CAQH profile for payer enrollment?
A complete CAQH profile must include the provider’s NPI, current medical license with renewal date, DEA registration, malpractice insurance certificate with current policy dates, board certification, 10-year work history, education and training records, hospital privileges, and attestation answers about adverse actions and malpractice claims. All uploaded documents must be current. An expired malpractice certificate or lapsed license in the profile causes the payer to pause the review until a current version is uploaded and the profile re-attested.
How does an expired CAQH profile affect payer enrollment?
An expired CAQH profile delays every concurrent payer enrollment application that queries it, adding two to four weeks per payer to an enrollment timeline that is already 90 to 120 days long. Revenue lost during this extended window is not recoverable retroactively. For a physician with multiple payers in simultaneous review, one expired profile can produce simultaneous delays at all of them, compounding the total revenue impact significantly.
Do all payers use CAQH for credentialing?
Most major commercial payers use CAQH ProView, including UnitedHealth, Aetna, Cigna, Humana, and Blue Cross Blue Shield plans in most states. Medicare enrollment runs through CMS PECOS, not CAQH. State Medicaid agencies use their own portals. A CAQH profile does not replace Medicare enrollment through PECOS. Both processes must be completed in parallel for a new provider to bill Medicare and commercial payers. Medicare Advantage plans, however, are administered by commercial insurers and do use CAQH for their credentialing reviews.
Can a new provider start billing before their CAQH profile is complete?
No. A provider cannot bill commercial payers as in-network until payer enrollment completes, and most commercial enrollments cannot complete without a verified CAQH profile. Building the CAQH profile is the first step in the enrollment process. Practices that submit payer applications before the CAQH profile is complete will see those applications stall at the CAQH verification stage, extending the total enrollment timeline beyond what the payer’s own review process requires.
What is the financial impact of a delayed CAQH profile on payer enrollment?
A CAQH issue that adds four weeks to a commercial payer enrollment can cost $13,500 to $50,000+ in unrecoverable revenue depending on the provider’s specialty, patient volume, and what percentage of their panel is on that payer. When the same expired profile delays multiple concurrent applications simultaneously, the revenue impact multiplies. None of this revenue is recoverable after enrollment completes. The payer will not pay retroactively for the gap period.
Should practices outsource CAQH profile management?
Most practices benefit from outsourcing CAQH profile management because the 120-day re-attestation cycle, document expiration tracking, and multi-provider profile maintenance require consistent follow-through that in-house staff managing other responsibilities rarely sustain reliably. A credentialing partner maintains current profiles for every provider, tracks document expiration dates, sends re-attestation reminders in advance, updates profiles when credentials renew, and confirms payer authorizations before application submission. The cost of this service is a fraction of the revenue lost in a single CAQH-driven enrollment delay.
Related Resources from Qualigenix
Expired CAQH Profiles Cost More Than the Fix. We Keep Them Current.
Qualigenix manages CAQH profiles for every provider in your practice, tracking re-attestation windows, document renewals, and payer authorizations so that no enrollment application stalls on a profile issue we could have prevented.
Our team delivers 99% claim accuracy, a 95% first-pass acceptance rate, an average 36-day collection cycle, and a 30% reduction in AR days. We onboard in as few as 6 days.
Precision. Progress. Qualigenix.


