What is a Clean Claim Rate? Benchmarks & Best Practices
The Qualigenix Editorial Team consists of certified billing and coding experts with over 40 years of experience across 38+ medical specialties. Our content is rigorously researched against CMS, AMA, and payer-specific guidelines to ensure total compliance and accuracy. We apply the same elite standards to our resources as we do our client work, consistently delivering high claim accuracy and significant reductions in AR days.

Medical practices in the United States face a formidable challenge in 2026. Payers are deploying increasingly sophisticated algorithms to scrutinize every submission. Recent data suggests that initial denial rates are climbing, creating a significant bottleneck for provider cash flow. This environment makes understanding what a clean claim is absolutely critical for financial stability.
Revenue cycle teams can no longer rely on volume to cover up inefficiencies. They must prioritize precision. A claim that requires manual intervention or rework costs the practice valuable time and money. It also delays the reimbursement cycle. Mastery of claim accuracy prevents these operational stalls. This guide explores the mechanics of claim purity, defines industry benchmarks and also outlines actionable strategies to ensure your claims pass the first gate every time.
What Is a Clean Claim?
A clean claim is a medical claim that includes complete and accurate information and meets all payer claim requirements at the time of submission. The claim passes automated edits and moves directly into payment processing without rejection or manual review. This includes correct patient details, valid diagnosis and procedure codes, proper modifiers, and accurate provider identifiers. A strong, clean claim rate reflects reliable billing accuracy metrics and steady revenue cycle performance. Errors such as missing data or incorrect coding lower the claim acceptance rate and delay reimbursement. Clean claims reduce rework and speed up payment cycles. This makes them essential for a predictable cash flow.
How Payers Define a Clean Claim
Payers evaluate submissions against a strict set of criteria. They view a claim as “clean” only if it meets specific operational standards.
- Data Accuracy: All patient demographics must match the payer’s file exactly.
- Coding Validity: Current CPT and ICD-10 codes must be used without conflict.
- Eligibility Status: The patient must have active coverage on the date of service.
- Timeliness: The claim must arrive within the contractual filing limit.
Any deviation from these rules strips the claim of its “clean” status. It instantly becomes a “dirty” or rejected claim. This rejection forces the provider to correct and resubmit the file.
What Is a Clean Claim Rate and Why Does It Matter?
The clean claim rate serves as a vital barometer for billing health. It measures the percentage of claims that pass internal edits and clearinghouse scrubs on the very first attempt. This metric reveals the efficiency of your front-end and coding processes.
A high rate indicates a streamlined operation. It means your staff captures data correctly at intake, which means your coding team understands payer nuances. A low rate signals systemic problems. It suggests that your team spends excessive time fixing errors that should not exist. This rework delays payment and increases administrative costs. Improving this metric is the fastest way to accelerate cash flow.
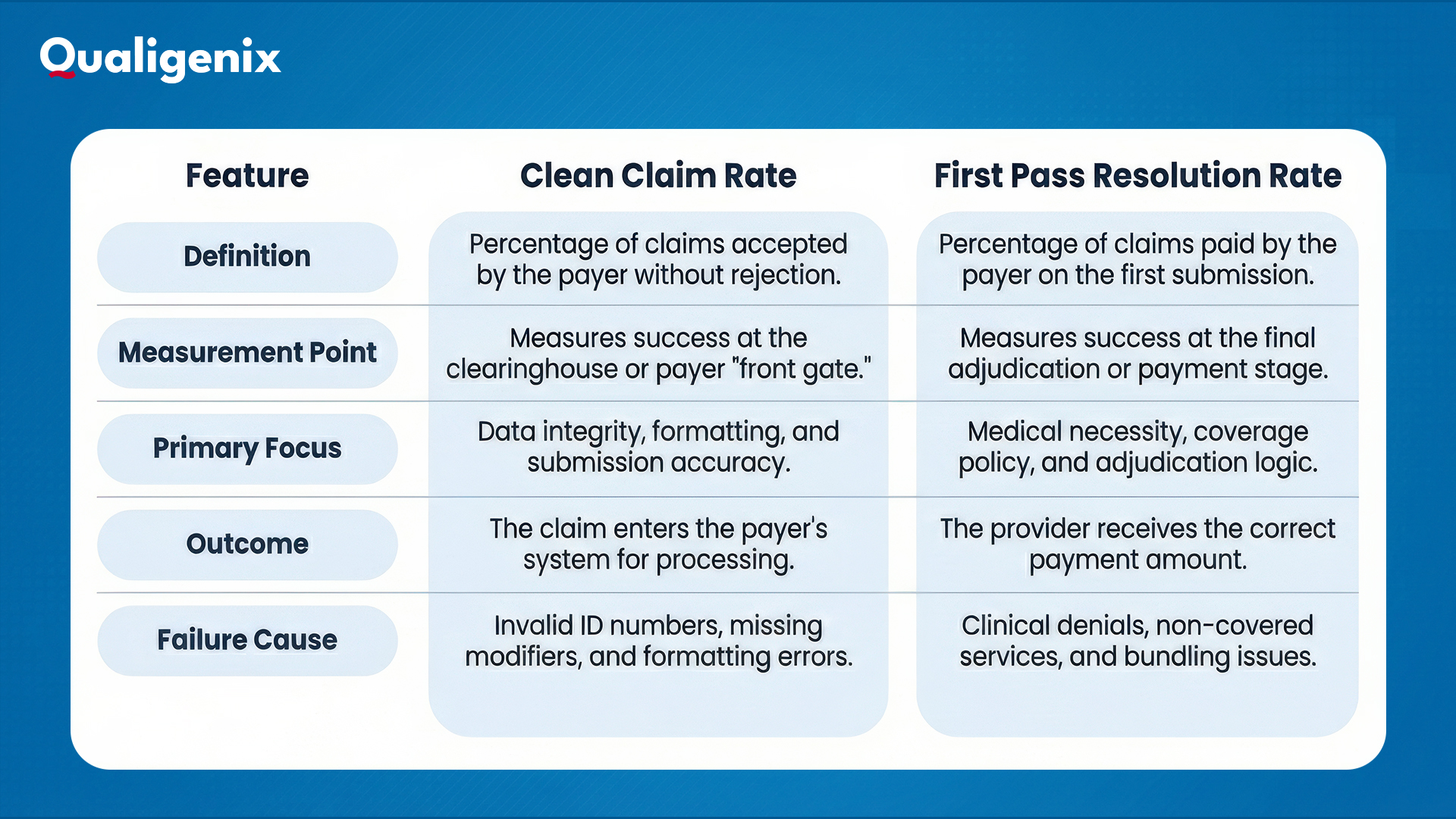
Clean Claim Rate vs First Pass Resolution Rate
Many professionals confuse these two metrics. They are related but distinct. Here are the key differences in diagnosing revenue cycle issues:
Clean Claim Rate Benchmarks Across Medical Practices
You cannot manage what you do not measure. Comparing your performance against industry standards is essential. Medical billing benchmarks provide a target for your team. They help you understand if your rejection volume is normal or problematic.
What Is Considered a Healthy Clean Claim Rate
High-performing medical practices typically achieve a clean claim rate between 95% and 99%. This range indicates that the vast majority of submissions move effortlessly into the adjudication phase.
- 95% or Higher: This is the standard. It implies robust internal controls and effective claim scrubbing.
- 90% to 95: This range is acceptable but leaves room for improvement. It suggests minor process gaps.
- Below 90%: This level indicates significant operational failure. Cash flow is likely suffering due to preventable delays.
Specialty nuance matters here. Complex fields like cardiology or oncology may see slightly lower rates due to intricate coding rules. Primary care often sees higher rates due to repetitive visit types.
Warning Signs of a Low Clean Claim Rate
A dropping rate rarely happens in isolation. It usually triggers a cascade of negative financial indicators.
- Rising Rejections: The clearinghouse reports show a spike in failed transmissions.
- Payer Edits: Staff spend more time logging into payer portals to fix simple errors.
- Delayed Payments: The average days in accounts receivable (AR) begin to climb.
These signs demand immediate investigation. Ignoring them leads to a bloated AR and a backlog of claim rejection rate issues that become harder to fix over time.
Common Reasons Claims Fail to Be Clean
Most claim failures are not malicious. They are mechanical, as they stem from small operational oversights that compound into major bottlenecks. Identifying these root causes is the first step toward denial prevention strategies.
Eligibility and Patient Data Errors
The most frequent culprit is simple data entry. A front desk staff member might transpose a digit in the policy number. They might misspell the patient’s last name. Eligibility verification impact is profound here. If the insurance plan on file is inactive or incorrect, the claim stops immediately. These errors are entirely preventable with diligent intake processes.
Coding and Modifier Mistakes
Medical coding requires precision. A mismatch between the diagnosis code and the procedure code triggers a rejection. This is often called a lack of medical necessity. Claim scrubber tools usually catch these, but some slip through.
Missing or invalid modifiers also cause failures. A payer might require a specific modifier to unbundle a service. If the coder omits it, the system rejects the line item. Frequent updates to CPT manuals mean that coders must stay educated to maintain a high first pass resolution rate.
Missing Authorizations or Referrals
Managed care plans protect their costs through prior authorizations. They require permission before a provider performs a specific test or procedure. Failing to include the authorization number on the claim is a fatal error.
Referrals work similarly. A specialist cannot see an HMO patient without a referral from the primary care physician. If the claim lacks this referral source, it is not a clean claim. It will face rejection until the provider supplies the missing link.
Medical Necessity and Documentation Gaps
Payers require clinical justification for every service. The diagnosis codes must tell a story that supports the procedure codes. A claim for a knee X-ray submitted with a diagnosis of a sore throat is illogical. It will fail.
Documentation gaps often lead to back-end denials, but they also trigger front-end rejections if the code combinations flag a “mutually exclusive” edit. Billing accuracy metrics suffer when clinical teams fail to document the specific details required for high-specificity ICD-10 coding.
Best Practices to Improve Clean Claim Rate

Improving your clean claim rate requires a culture of prevention. You must catch errors before they leave your system. Therefore, operational discipline is the key to success.
Front End Verification and Intake Accuracy
Quality begins at the front desk. Staff must verify insurance eligibility for every patient at every visit. They should scan insurance cards directly into the system to avoid transcription errors.
Automated eligibility tools can check coverage in real-time. They confirm the patient’s deductible status and verify the policy is active. This step alone can eliminate a significant portion of clean claims definition failures.
Pre Submission Claim Scrubbing
Technology is your best defense against human error. Claim scrubber tools act as a digital gatekeeper. They review every claim against millions of payer rules before transmission.
These scrubbers catch missing fields. They identify invalid codes and flag age or gender conflicts. Implementing a robust scrubber ensures that only valid files reach the clearinghouse. It is a critical investment for revenue cycle performance.
Coding Audits and Training
Coding rules change annually. Your team’s knowledge must evolve with them. Regular audits of coding accuracy identify knowledge gaps. They reveal if a specific provider or coder consistently makes the same mistake.
Targeted training fixes these issues. Education should focus on the specific reasons for recent rejections. This continuous feedback loop improves the first pass resolution rate over time.
Denial Trend Analysis
You must learn from your failures. Analyze your rejection reports weekly. Look for patterns. Is one specific payer rejecting claims for a missing tax ID? Is one specific CPT code triggering edits?
This denial trend analysis allows you to update your scrubber rules. It helps you fix the root cause so the error does not repeat. It transforms reactive work into proactive system improvement.
How Qualigenix Helps Improve Clean Claim Rate
Qualigenix operates as a strategic partner in your revenue cycle. We understand that a clean claim is the fastest route to revenue. Our comprehensive approach targets every friction point in the submission process.
Automated Eligibility Verification
We deploy advanced technology to verify patient coverage before the appointment occurs. Our system checks active status and benefits details. This rigorous screening prevents eligibility verification impact errors from ever reaching the claim form.
Specialized Coding Validation
Our team consists of certified coding experts who understand specialty-specific nuances. We perform multi-tier audits on your coding workflows and procedure codes align perfectly to support medical necessity and prevent coding and modifier mistakes.
Authorization and Referral Tracking
We do not leave approvals to chance. Our dedicated staff tracks authorization requirements for every scheduled procedure. We ensure the authorization number is present and valid on the claim. This proactive management eliminates rejections due to missing authorizations or referrals.
Clean Claims Build Strong Revenue Foundations!
A high clean claim rate is the foundation of reliable revenue cycle performance. Providers that invest in prevention instead of correction achieve faster reimbursements and lower operational stress. Accurate eligibility checks reduce the claim rejection rate. Strong coding practices improve the claim acceptance rate and raise the first pass resolution rate. Teams that follow medical billing benchmarks also improve billing accuracy metrics and reduce follow-up work. Denial prevention strategies protect cash flow and reduce staff workload. Claim scrubber tools add another layer of quality control before submission. These efforts create consistent payment cycles and better financial stability. Clean claims do not happen by chance. They come from disciplined processes and daily attention to detail.
FAQs
1. What does clean claim mean in medical billing?
A clean claim means a medical claim submitted with complete patient data, correct codes, valid insurance details, and full compliance with payer claim requirements, allowing direct processing without edits or rework.
2. What is a good clean claim rate?
A good clean claim rate usually falls between eighty five and ninety five percent. Top performing practices often exceed this range by following medical billing benchmarks and strict billing accuracy metrics.
3. Why is clean claim rate important for cash flow?
A high clean claim rate speeds up reimbursement cycles, reduces payment delays, lowers follow-up workload, and stabilizes monthly revenue. This directly improves cash flow and overall revenue cycle performance.
4. How can clinics improve clean claim rate quickly?
Clinics can improve clean claim rate by strengthening front desk data accuracy, improving eligibility verification impact, and using claim scrubber tools to catch errors before payer submission.
5. Does clean claim rate affect denial rates?
Clean claim rate has an inverse relationship with claim rejection rate. Higher accuracy reduces denials because fewer claims fail payer edits and compliance checks during initial processing.
6. Can clean claim rate be improved without new software?
Yes. Teams can improve clean claim rate through staff training, standardized workflows, better documentation reviews, and consistent denial prevention strategies that reduce manual errors and submission gaps.