Rehab Medical Billing Services That Protect Every Dollar Your Practice Earns
Qualigenix delivers specialized support as a trusted rehab medical billing company, helping rehabilitation providers across the US reduce denials, improve collections, and stabilize cash flow. Our structured rehabilitation billing services ensure every therapy session is accurately coded, submitted, and reimbursed.


Rehab Medical Billing Services Built for High-Volume Therapy Practices
Qualigenix supports rehab providers across the US with structured rehab medical billing services that handle frequent visits, bundled sessions, and payer-specific therapy rules. Our workflows reduce billing friction and ensure consistent reimbursements for physical and outpatient rehabilitation services.
Rehabilitation Billing Services That Reduce Coding and Claim Errors
We strengthen accuracy through expert rehab billing and coding, ensuring correct CPT usage, modifiers, and documentation alignment. This approach helps US rehab clinics lower rejections and improve first-pass claim acceptance.
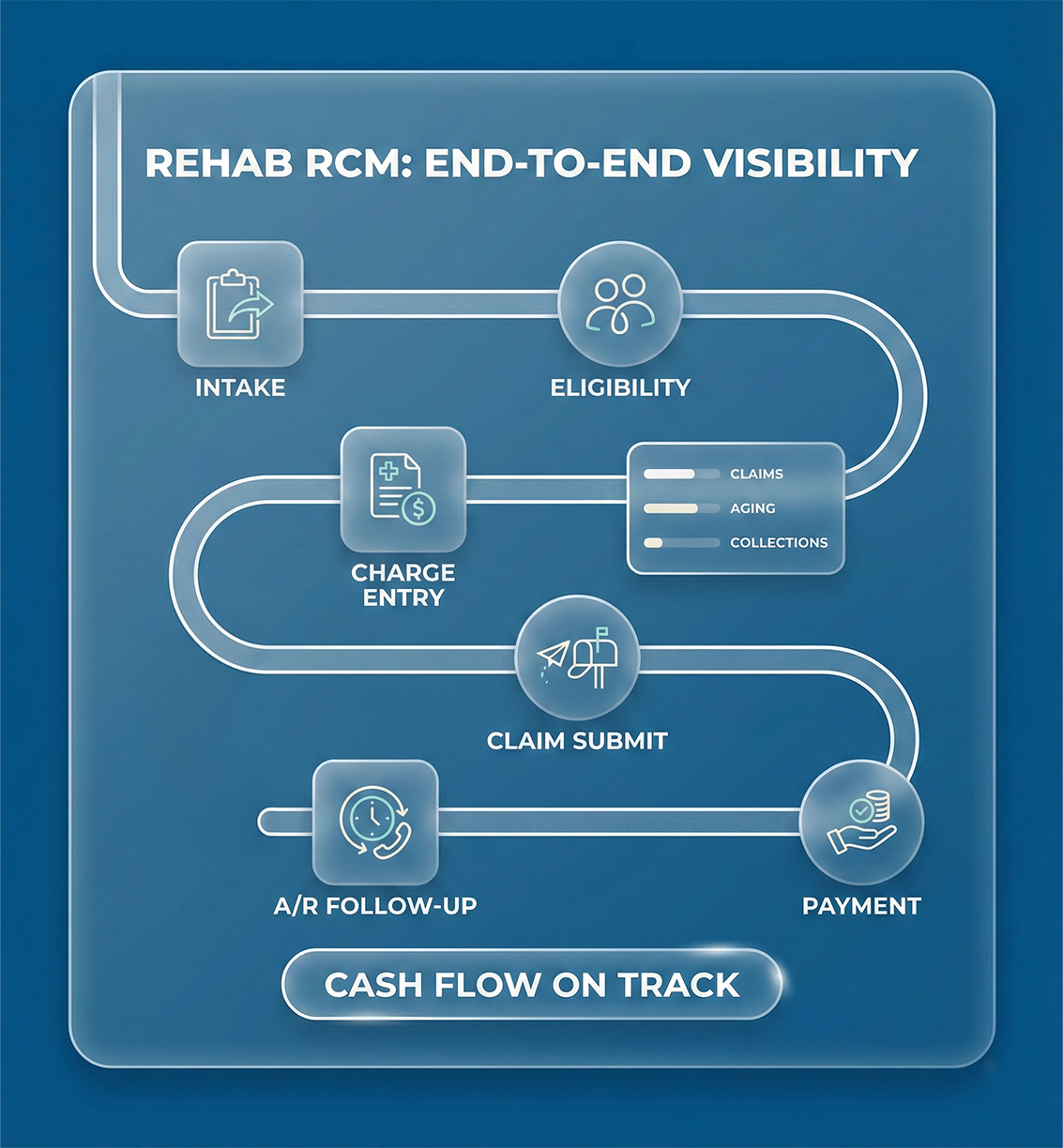
End-to-End Rehab Revenue Cycle Management for US Providers
Our rehab revenue cycle management tracks every claim from intake to payment, giving US practices full visibility into collections and aging. With proactive follow-ups, we help rehab centers maintain predictable cash flow.
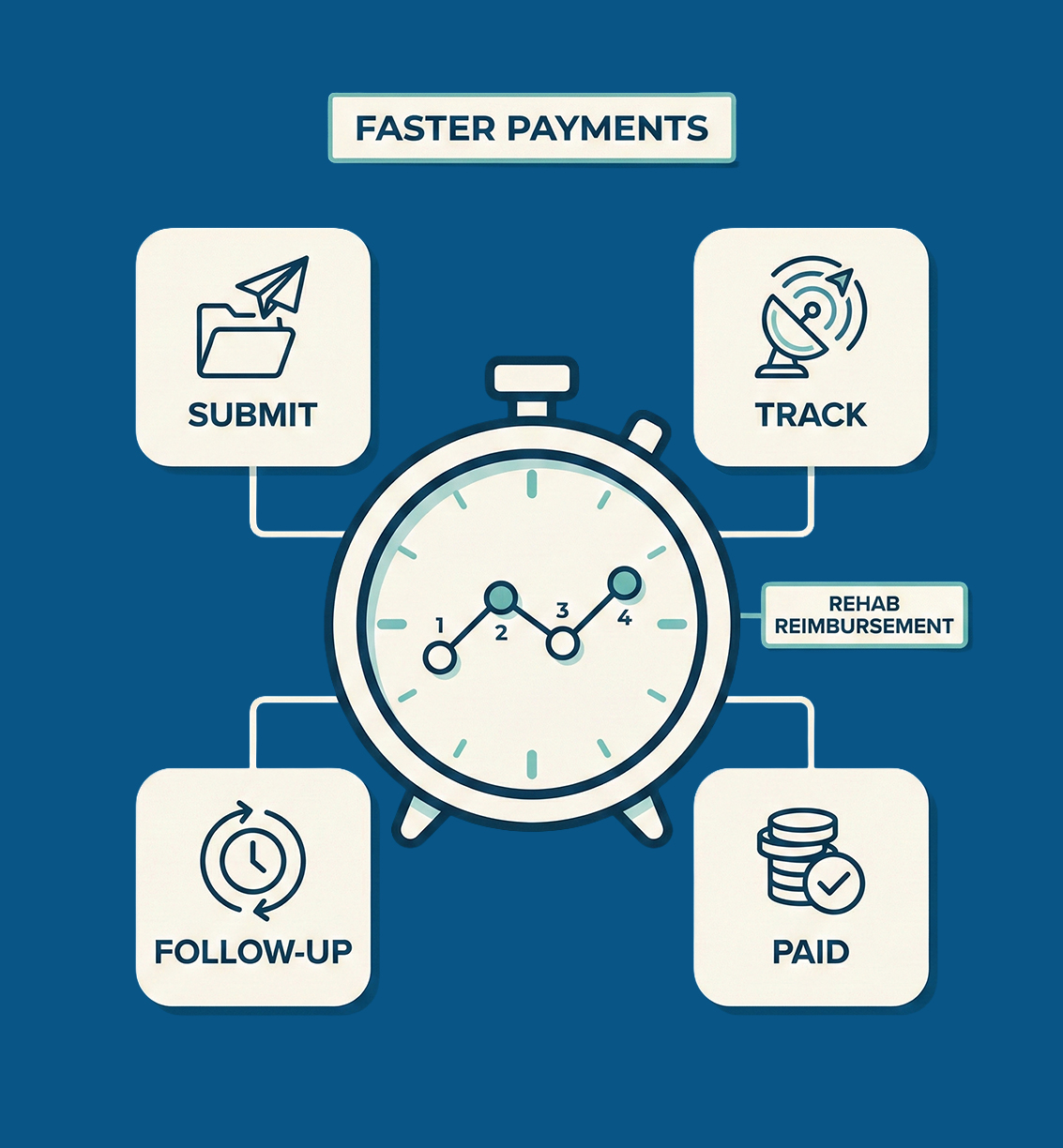
Faster Payments Through Optimized Rehab Reimbursement Workflows
Qualigenix improves payment timelines using structured rehab reimbursement services and real-time claim tracking. US-based rehab clinics benefit from fewer delays and stronger payer compliance across commercial and government plans.
Comprehensive Rehab Medical Billing Services from Eligibility to Reimbursement
Insurance Verification & Benefits
We perform thorough rehabilitation insurance verification before therapy begins, confirming visit limits, copays, and authorization requirements for US commercial and government payers.
Explore SolutionsMedical Coding Services
Our certified coders deliver precise rehab billing and coding for physical therapy, occupational therapy, and multi-session rehabilitation programs.
Explore SolutionsDedicated Account Management
A dedicated specialist oversees your rehab medical billing services, ensuring accountability and consistent communication.
Explore SolutionsEDI Rejection Management
We correct front-end clearinghouse edits quickly, reducing repeated submission cycles and improving claim acceptance rates.
Explore SolutionsDenial Management
Our structured rehab denial management identifies root causes, fixes documentation gaps, and resubmits claims to recover lost revenue.
Explore SolutionsA/R Follow-Up
Through proactive rehab AR follow up services, we track unpaid claims and follow up consistently with US insurers to keep revenue flowing.
Explore SolutionsHidden Billing Breakdowns That Impact Rehab Revenue — and How We Fix Them
Charge & Demographic Entry
Incorrect patient data or therapy unit entry causes immediate claim rejections. Even minor errors can delay rehabilitation claims processing and extend payment timelines across US payers.
Explore SolutionsClaim Transmission
Claims that fail to transmit properly never reach insurers. Broken submission workflows disrupt rehab revenue cycle management and increase A/R days for US rehab providers.
Explore SolutionsEDI Rejection Management
Front-end clearinghouse edits can block claims before payer review. Without fast correction, these issues repeat and weaken overall rehab reimbursement services performance.
Explore SolutionsMonthly A/R Analysis
Without structured review, aging balances go unnoticed. Poor oversight in rehab medical billing services results in revenue leakage and inconsistent cash flow in US therapy practices.
Explore SolutionsPre-Authorizations
Missing approvals for therapy sessions can trigger preventable denials. Strong authorization workflows protect rehabilitation billing services from unnecessary write-offs.
Explore SolutionsTrusted by US Rehab Centers for Reliable Rehab Revenue Cycle Management



Comprehensive Rehabilitation Billing Services Across Therapy Disciplines
Physical Therapy
Occupational Health
Orthopedic
Neurology
Pain Management
Sports Medicine
Chiropractic
Skilled Nursing Facility (SNF)
Home Health
Cardiology
Frequently Asked Questions
What do rehab medical billing services include for US therapy practices?
Our rehab medical billing services cover the entire revenue cycle for rehabilitation providers across the US. This includes insurance verification, therapy unit coding, electronic claim submission, denial management, A/R follow-up, and payment posting. As a specialized rehab medical billing company, we ensure every therapy session is billed accurately and reimbursed according to US payer requirements.
How do rehabilitation billing services reduce denials?
Our rehabilitation billing services strengthen documentation accuracy, improve rehab billing and coding, and apply payer-specific guidelines for therapy services. By proactively identifying coding gaps and authorization issues, US rehab clinics can significantly reduce repeat denials and avoid unnecessary revenue loss.
Can a rehab medical billing company improve cash flow for outpatient rehab centers?
Yes. A structured rehab medical billing company like Qualigenix implements strong rehab revenue cycle management workflows that shorten A/R days and improve reimbursement speed. US outpatient rehab providers benefit from faster collections and more predictable monthly revenue.
How do rehab medical billing services support multi-session therapy billing?
Multi-session therapy programs often require accurate unit tracking and modifier use. Our rehab medical billing services ensure proper documentation alignment and compliance with US commercial and government payer rules, reducing billing errors and improving first-pass claim acceptance.
Do rehabilitation billing services manage AR follow-ups and underpayments?
Absolutely. Our rehabilitation billing services include structured rehab AR follow up services, consistent payer communication, and underpayment tracking. This ensures US rehab practices recover full entitled reimbursements instead of accepting reduced payments.
How do rehab medical billing services stay compliant with US payer regulations?
Our rehab medical billing services incorporate updated coding standards, documentation audits, and payer policy monitoring. As an experienced rehab medical billing company, we help US rehabilitation providers remain compliant while maximizing reimbursement opportunities.