Anesthesiology Billing Services That Protect Every ASA Unit
Experience tighter anesthesiology revenue cycle management with Qualigenix, an anesthesiology medical billing company built to improve accuracy, reduce denials, and speed up payments across every case.


Anesthesiology Billing Services That Get ASA Units Right, Every Case
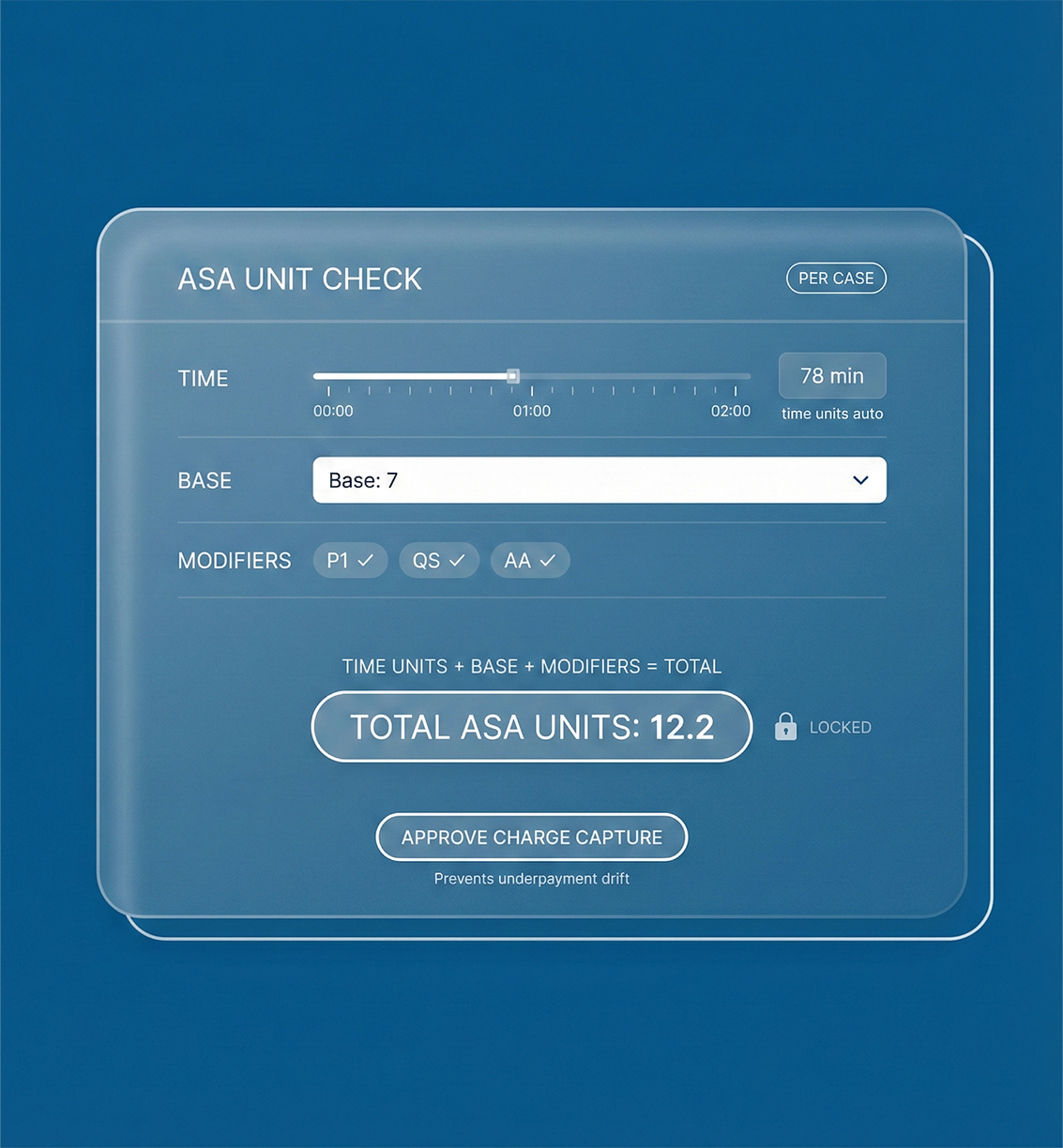
Qualigenix align ASA unit calculation with precise anesthesia time-based billing and tighter anesthesia charge capture, reducing underpayment risk by 25–35% in many practices.
Anesthesiology Billing Services That Improve Coding and Modifier Accuracy
Our anesthesia coding services strengthen anesthesia modifier compliance with complete anesthesia CPT and ICD-10 coding support, often cutting avoidable denials by 15–25%.
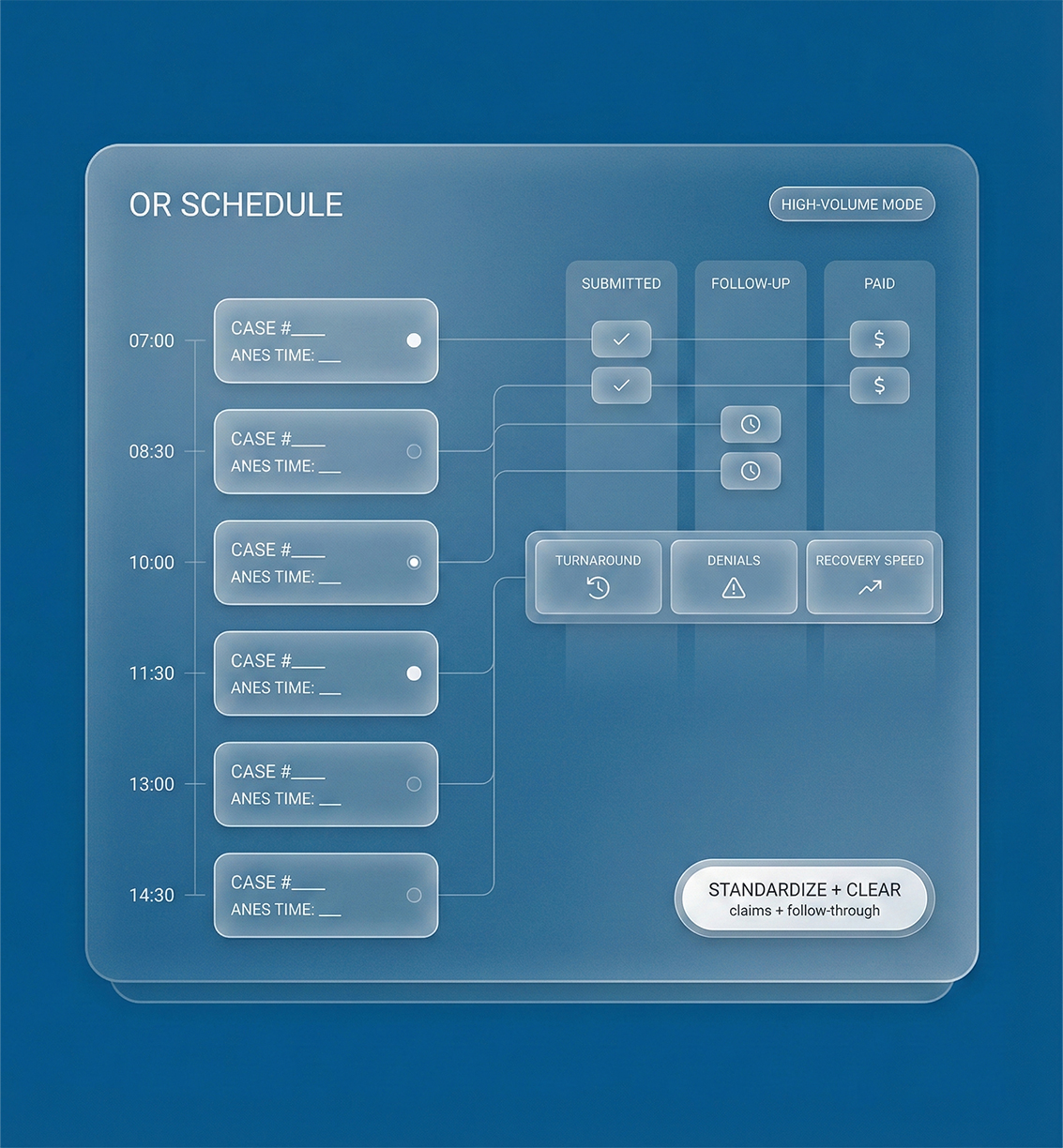
Anesthesiology Revenue Cycle Management Built for High-Volume OR Schedules
We standardize anesthesia claims submission and follow-through with anesthesia denial management, using anesthesia reimbursement analytics to improve payer outcomes and speed recoveries.
Anesthesiology Medical Billing Company Support That Reduces Rework for CRNA Teams
As an anesthesiology medical billing company, we provide CRNA billing support that keeps documentation, coding, and submission aligned, reducing repeat edits and resubmissions by 10–20%.
End-to-End Anesthesiology Billing Services That Protect Every Minute and Unit
Medical Coding Services
Accurate anesthesia coding services with anesthesia CPT and ICD-10 coding support and tight anesthesia modifier compliance to reduce rework and underpayments.
Explore SolutionsCharge & Demographic Entry
Stronger anesthesia charge capture so every case detail is captured cleanly before anesthesia claims submission starts.
Explore SolutionsClaim Transmission
Cleaner anesthesia claims submission with payer-ready formatting to reduce delays from avoidable edits and resubmits.
Explore SolutionsDenial Management
Focused anesthesia denial management that resolves payer issues faster and protects outcomes across repeat denial categories.
Explore SolutionsPre-Authorizations
Pre-auth workflows aligned to case requirements, supported by CRNA billing support to prevent missed approvals and stalled payments.
Explore SolutionsPerformance Reporting (Weekly/Monthly)
Weekly and monthly anesthesia reimbursement analytics tied to units, time, denials, and payer behavior so you can fix leakage early.
Explore SolutionsWhat Makes Our Anesthesiology Medical Billing Company Stand Out
Fee Schedule Optimization
We reduce underpayments by aligning payer contracts to accurate ASA unit calculation and anesthesia time-based billing rules.
Explore SolutionsMonthly A/R Analysis
We pinpoint delays by payer and case type, then prioritize fixes using anesthesia reimbursement analytics and denial trends.
Explore SolutionsEDI Rejection Management
We cut preventable rejections by tightening anesthesia claims submission rules and improving data readiness before transmission.
Explore SolutionsDedicated Account Management
One point of ownership for follow-ups, documentation gaps, and payer touchpoints, supported by CRNA billing support for cleaner resolution.
Explore SolutionsMedical Audit
We validate anesthesia modifier compliance and strengthen anesthesia CPT and ICD-10 coding support to prevent repeat errors.
Explore SolutionsTrusted by Leading Brands Across Healthcare and Beyond



Anesthesiology Billing Services Trusted by High-Volume Teams
Ambulatory Surgical Centers (ASC)
General Surgery
Pain Management
Orthopedic
OB/GYN
Oral & Maxillofacial Surgery
Gastroenterology
Cardiology
Emergency Medicine
Neurology
Frequently Asked Questions
What do anesthesiology billing services include end to end?
Anesthesiology billing services cover documentation checks, anesthesia coding services, and clean anesthesia claims submission through payer-specific workflows. The process also protects revenue with stronger anesthesia charge capture and faster denial resolution.
How does anesthesiology revenue cycle management reduce underpayments?
Anesthesiology revenue cycle management improves accuracy in ASA unit calculation and anesthesia time-based billing, then measures outcomes using anesthesia reimbursement analytics. This reduces payment variance, improves collections, and limits avoidable rework.
How does Qualigenix improve anesthesiology billing services for high-volume groups?
Qualigenix standardizes anesthesiology billing services with tighter anesthesia claims submission, daily charge capture controls, and proactive payer follow-through. The result is fewer edits, cleaner claim movement, and better performance using anesthesia reimbursement analytics.
Why choose an anesthesiology medical billing company instead of general billing support?
An anesthesiology medical billing company specializes in anesthesia modifier compliance and payer behavior across anesthesia billing scenarios. With strong anesthesia CPT and ICD-10 coding support, you reduce denials, prevent undercoding, and protect reimbursement accuracy.
How does Qualigenix support CRNA billing workflows and split cases?
Qualigenix provides structured CRNA billing support for supervision, direction, and team billing rules, while enforcing anesthesia modifier compliance. We pair this with consistent anesthesia time-based billing checks so units and modifiers stay aligned for payment.
How do you handle anesthesia denial management and prevention?
Anesthesia denial management starts with denial categorization, payer-specific corrections, and resubmission with improved coding and documentation. We reinforce prevention through anesthesia coding services, stronger anesthesia charge capture, and continuous anesthesia reimbursement analytics tracking.