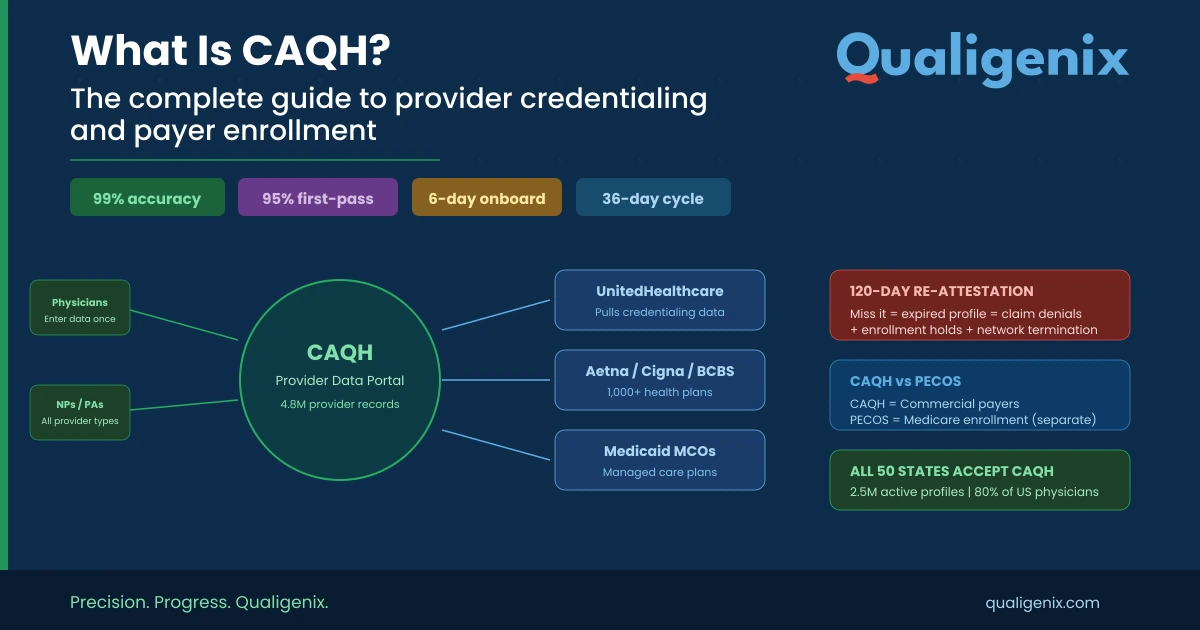
What Is Revenue Cycle Management? A Beginner’s Guide for Healthcare Providers
The Qualigenix Editorial Team comprises certified medical billing professionals, CPC-credentialed coders, prior authorization specialists, and revenue cycle consultants with more than 40 years of combined hands-on experience serving solo physicians, group practices, hospitals, and ASCs across 38+ specialties in the United States. Every guide, article, and resource published on the Qualigenix blog is researched against current CMS guidelines, Federal Register notices, AMA policy updates, and payer-specific billing rules — and reviewed for compliance accuracy before publication. Our content reflects the same standards we apply to our client work: 99% claim accuracy, 95% first-pass acceptance, and a 30% average reduction in AR days.

A family comes to your clinic; the doctor treats them, and the patient leaves satisfied. Weeks later, you’re still waiting for an insurance payment because the claim was denied over a coding error. A 2024 multi-institutional study reported final insurance denial rates between 2.2% and 2.9% across common procedures. On paper, that may look small. In reality, for large practices, this translates to millions in lost or delayed payments every year. This is where revenue cycle management (RCM) becomes indispensable.
But what is revenue cycle management? It’s the system that ensures every service gets billed, all claims are given clear scrutiny, and payments arrive on time. Without strong RCM, practices lose money and face cash flow stress. So, if you are wondering what RCM workflows are or why you should use them, keep reading to get all your answers.
What is Revenue Cycle Management?
Revenue cycle management (RCM) is the process of tracking patient care from the first appointment through the final payment. The revenue cycle management definition covers insurance verification, coding, claim submission, denial management, and payment posting. Every step links medical services with financial outcomes.
When RCM works well, healthcare providers see fewer errors, lower denial rates, and faster reimbursements. Without it, even excellent medical care may not generate reliable revenue. RCM is the financial framework that keeps healthcare providers stable and sustainable.
Why RCM Matters (Benefits)
Running a healthcare practice is not limited to delivering care. Every patient encounter also triggers a financial chain that determines how the provider gets paid. RCM’s meaning is the system that protects margins, supports operations, and maintains patient trust. The key RCM benefits fall into three major areas:
Financial Stability & Cash Flow
RCM speeds up reimbursements, as it minimizes errors and denials. With fewer unpaid claims, providers receive money on time and maintain a steady cash flow. This predictability helps them properly cover salaries, supplies, and even operational costs. It also allows private healthcare practices to plan and invest in long-term growth.
Operational Efficiency
Clear processes can prevent coding errors and make claim submissions more accurate. You can also use automation to reduce repetitive tasks and lower denial risks. With less time spent on corrections, staff can focus on important duties, which improves overall team productivity.
Enhanced Patient Experience
Patients notice when billing runs smoothly. Transparent statements reduce confusion, and fewer denials mean fewer calls about unpaid claims. Any issues that do occur are resolved faster, which makes financial interactions less stressful.
Key RCM Process Steps & Workflows
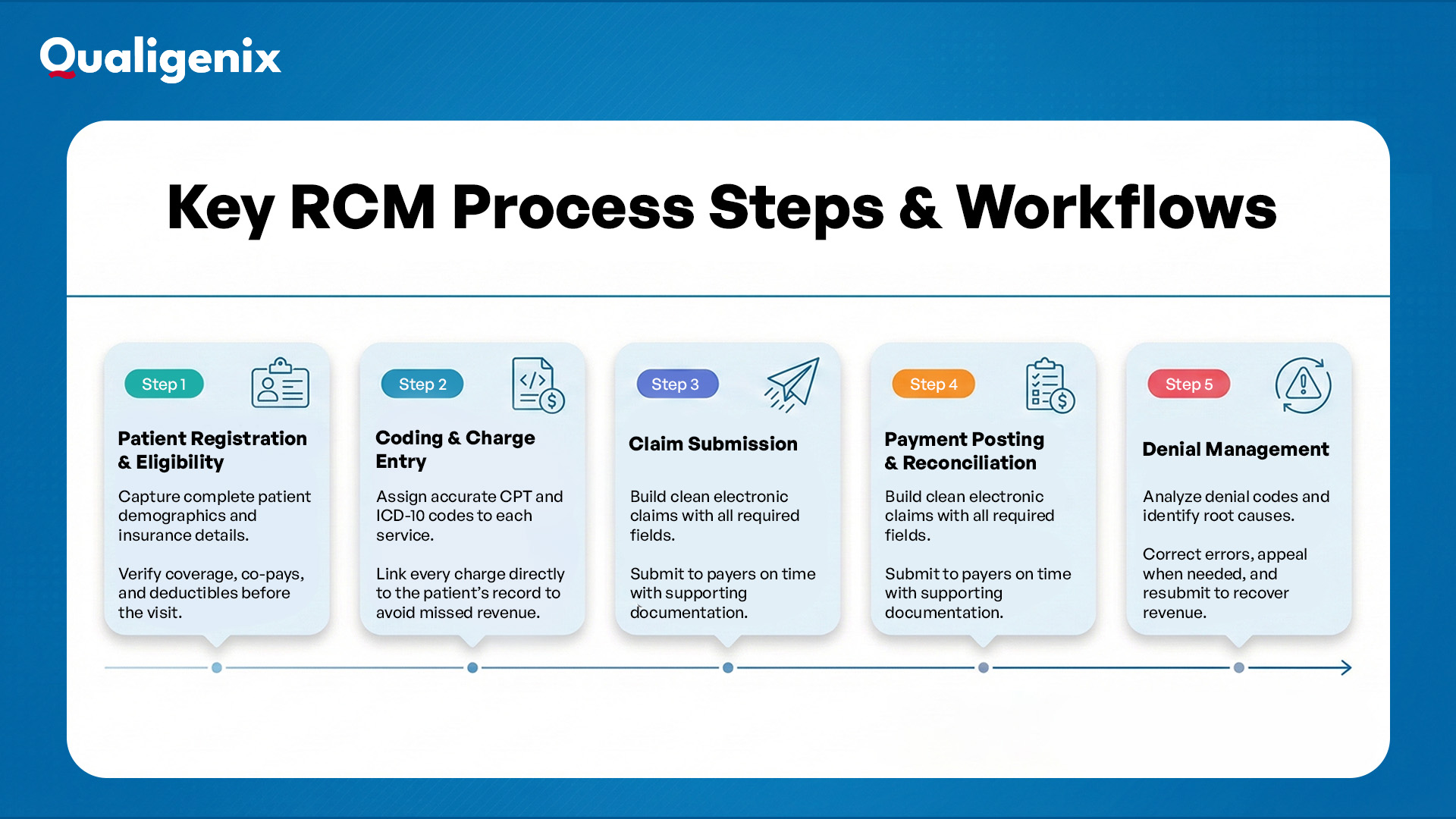
In Medicare Advantage, nearly one in five claims is denied at first submission, which reduces overall provider revenue by about 7%. Therefore, to protect your organization, you need to follow each step of the revenue cycle with care. Here are the common RCM process steps:
Patient Registration & Eligibility
Everything starts when your staff registers the patient. Details like name, date of birth, address, and insurance ID must be correct. Even a small error, such as one wrong digit in a policy number, can stop the claim. So, always verify insurance before the visit. Confirm that the plan is active and check what services it covers. Go over co-pays and deductibles with the patient so there are no surprises later.
Coding & Charge Entry
Once the visit ends, the care you provided must be turned into codes. These codes, Current Procedural Terminology (CPT) for procedures and International Classification of Diseases (ICD-10) for diagnoses, explain to the insurance company what you did and why. Each charge should connect directly to the patient’s record. If codes are missing or incorrect, your claim is likely to be denied.
Claim Submission
The next step is to send the claim to the payer. Most practices now use electronic submission because it is faster and more reliable. But speed means nothing without accuracy. A clean claim has all the right details: correct patient information, proper codes, and required documentation. If anything is missing, the payer will reject it, and you will wait longer to get paid.
Payment Posting & Reconciliation
When the insurance firm pays, your billing team must record it correctly. Each payment should match the charge that was billed. If the insurer pays less than expected or does not pay at all, you need to catch it immediately. Reconciling payments quickly ensures your practice receives the full amount it is owed.
Denial Management
Even well-prepared claims can be denied. What matters is how you respond. Review the denial to see why it happened. It may be a missing document, a coding error, or an eligibility issue. Correct the mistake and resubmit the claim before the deadline. Acting quickly reduces lost revenue and keeps your cash flow steady.
Revenue Cycle Management KPIs You Should Track
If you want to measure the health of your revenue cycle, you need to track a few key performance indicators (KPI). These metrics tell you how quickly money comes in, how many claims get approved, and how much it costs you to collect each dollar. Without them, it’s easy to miss leaks in your system. Here are the common revenue cycle KPIs you must track:
Days in Accounts Receivable (AR)
This measures how many days it takes to get paid after you send a claim. If your AR is high, it means money is tied up, and your practice may struggle with cash flow. Most providers aim to stay under 40 days, though some specialties may vary.
Clean Claim Rate
A “clean claim” shows the percentage of claims accepted by the insurer on the first try. If your rate is 85%, it means 15% of your claims bounce back for corrections. That’s lost time and delayed payment. So, always aim for a clean claim rate of 90% or more. If this number drops, it usually signals mistakes in coding or patient information.
Denial Rate
The denial rate tells you how often insurers reject claims. For example, if 10 out of every 100 claims are denied, you have a 10% denial rate. A rising denial rate means problems with eligibility checks, documentation, or coding. Track the reasons for denials to fix weak spots so the same issues don’t keep repeating.
Net Collection Rate
This KPI shows how much of your expected revenue you actually collect. For example, if you should collect $100,000 but only receive $90,000, your net collection rate is 90%. Strong practices aim for 95% or more.
Cost to Collect
This shows how much you spend to collect every dollar. It includes staff salaries, software, and other overhead. If your cost to collect is high, your process is inefficient. Lower costs mean your practice keeps more of what it earns.
Top RCM Challenges & How to Overcome Them

Denials, staffing shortages, and compliance issues are the three problems that disrupt revenue most often. Here is how each challenge affects your practice and how you can overcome it:
High Denial Rates
Every denied claim delays payment and adds extra work for your staff. Most denials happen because of missing information, incorrect coding, or eligibility errors.
How to Overcome: Use claim scrubbers and audit tools that review claims before they go out. These tools flag errors in patient demographics, coding, or missing documentation. You can also train staff to double-check eligibility during registration.
Staffing Gaps
Billing requires accuracy and speed, but many practices struggle to find and keep skilled billers. Turnover is also common, and when a team member leaves, collections can stall.
How to Overcome: There are two practical solutions. You can outsource part of your billing to a professional RCM company for consistent coverage and access to experienced specialists. In addition, invest in regular training for your in-house staff. Training will build confidence, reduce errors, and create a backup system if a team member leaves.
Compliance Errors
Payer rules and federal regulations frequently change. Missing an update can cost you money or lead to penalties.
How to Overcome: Create a compliance checklist based on your specialty and update it whenever payer rules change. Schedule regular reviews of policies and processes to catch gaps early. Many practices also assign a compliance lead who monitors updates and trains staff. These steps keep your billing accurate, reduce risk, and align your practice with current requirements.
Best Practices for Effective RCM
Strong revenue cycle management doesn’t just happen. It takes consistent effort and the right strategies. Here are the best practices that can make your RCM process steps smoother and more reliable:
Automate Repetitive Processes
Tasks like eligibility checks, claim submissions, and payment reminders take up time but follow the same steps every time. You can automate them with reliable softwares to complete the process faster and with fewer mistakes.
Train Billing Staff Regularly
Insurance codes and payer rules change at times. Without training, staff can fall behind, and mistakes can become frequent in the process. So, train the staff regularly to keep them sharp and reduce errors.
Monitor KPIs Monthly
Review your KPIs every month to get a clear picture of performance. For example, if your denial rate suddenly spikes, you can act quickly to find the cause and fix it. Consistent monitoring keeps problems small before they grow.
Use Analytics for Continuous Improvement
Analytics tools show you trends that may not be obvious in day-to-day work. They highlight patterns in denials, delays, or payer behavior. With these insights, you can refine workflows, reduce costs, and improve collections over time.
Partner with Experts to Strengthen Your Revenue Cycle!
Understanding what revenue cycle management is goes beyond learning a set of financial steps. It is about building a system that supports providers, strengthens financial performance, and keeps patient care uninterrupted. When it falters, stress builds and revenue slips away.
At Qualigenix, we believe healthcare teams should spend less time chasing payments and more time caring for patients. Our mission is to deliver intelligent, efficient, and reliable RCM solutions that ease the administrative burden while improving stability. With innovation and integrity, we help providers reduce denials, secure faster payments, and create room for growth. So, start optimizing your RCM today and give your team the freedom to focus on patient care!
FAQs
1. What is RCM in healthcare?
Revenue cycle management (RCM) is the process that connects patient care with financial outcomes. It includes registration, coding, claim submission, payment posting, and denial management to ensure providers get paid for the services they deliver.
2. What are the steps in revenue cycle management?
The main RCM steps include:
- Patient registration and eligibility verification,
- Clinical documentation and coding,
- Charge capture and entry,
- Claim submission and processing,
- Payment posting and reconciliation,
- Denial management and appeals,
- Patient billing and collections, and
- Reporting and analytics.
3. How can I reduce medical claim denials?
You can lower denials by verifying insurance coverage upfront, coding accurately, and using claim scrubbers to catch errors before submission. Fast follow-up on rejected claims also prevents revenue from being lost.
4. What tools improve RCM performance?
RCM performance improves with automated eligibility verification, claim scrubbing software, integrated Electronic Health Records (EHR) systems, analytics dashboards, and denial management platforms.
5. Which KPIs should I monitor?
Track days in accounts receivable, clean claim rate, denial rate, net collection rate, and cost to collect. These KPIs give a clear picture of financial performance and highlight areas for improvement.
6. How often should RCM be reviewed?
Review your RCM monthly to track KPIs and spot problems quickly. Annual audits provide a deeper check, and with real-time dashboards, you can stay on top of performance throughout the year.