How Choosing a Perfect EMR/EHR For Your Practice Can Streamline Operations?
The Qualigenix Editorial Team comprises certified medical billing professionals, CPC-credentialed coders, prior authorization specialists, and revenue cycle consultants with more than 40 years of combined hands-on experience serving solo physicians, group practices, hospitals, and ASCs across 38+ specialties in the United States. Every guide, article, and resource published on the Qualigenix blog is researched against current CMS guidelines, Federal Register notices, AMA policy updates, and payer-specific billing rules — and reviewed for compliance accuracy before publication. Our content reflects the same standards we apply to our client work: 99% claim accuracy, 95% first-pass acceptance, and a 30% average reduction in AR days.

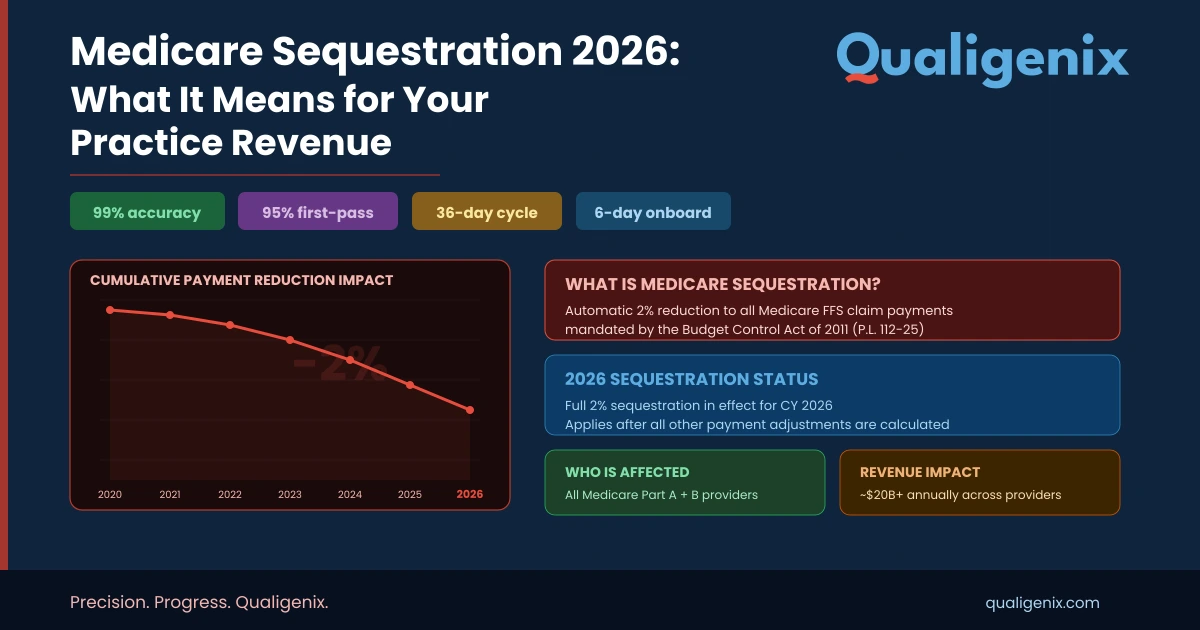
More than one in five medical claims get denied on the first submission, according to recent payer audits. Some specialties even report high denial spikes after coding or eligibility errors. Now here’s the real kicker: how many of those rejections are caused by staff mistakes, and how many are simply system failures?
If your team is copying patient data from one screen to another or manually resubmitting claims because two platforms don’t sync, is it fair to call that human error?
This is where healthcare revenue cycle management software providers prove their worth. Not through fancy dashboards, but through invisible fixes, like real-time eligibility checks, automatic charge capture, and claim edits that prevent denials before they hit payers.
Ask yourself: hw much faster would cash flow move if healthcare revenue cycle management software providers handled corrections before submission? If RCM software solutions cleaned claims at the source, would your billing team finally get ahead instead of reacting all month?
Let’s sort through what’s actually worth buying and what’s just another system waiting to stall your collections.
Why Your EMR/EHR Choice Impacts RCM Deeply?
An EMR that looks efficient on the clinical side can silently drain revenue if it fails to support billing logic. Poor field structure, weak data interoperability, or missing eligibility verification creates rework that billing teams can’t fix on their own.
If healthcare revenue cycle management software providers are layered on top of a rigid EMR, even the best RCM software solutions end up compensating instead of optimizing. That’s why your selection of an EMR directly affects denials, collections and staff workload.
1. Downstream Effects on Billing and Coding Accuracy
Missing modifiers, unchecked CPT mappings, or misaligned documentation fields account for a majority of preventable denials. If the EMR does not prompt for required data at the point of entry, coders and billers are left guessing.
That leads to coding accuracy gaps that stall claims before they even reach the payer. Before evaluating healthcare revenue cycle management software providers, check if your current EMR enforces structured clinical documentation.
Without that foundation, even automated scrubbing tools will struggle to correct upstream errors.
2. Impact on Claim Turnaround and Clean-Claim Ratios
The time between encounter and submission often depends on how well your EMR supports automated charge capture. If providers must manually assign codes or hand off billing through spreadsheets, clean-claim rates suffer.
Integrated RCM platforms that flag missing elements in real time help billers submit once instead of revising the same claim multiple times. Faster submission means faster adjudication and shorter AR cycles.
3. Operational Inefficiencies and Staff Burden
Every manual export, spreadsheet correction or payer login adds minutes that compound into hours. Billing professionals waste time on reconciliation instead of resolution.
When data interoperability is weak, support tickets increase and burnout follows. Pairing EMR selection with healthcare revenue cycle management software providers that sync workflows directly eliminates back-and-forth between departments and cuts down repetitive data entry altogether.
Key Features to Look for in RCM Software and EMR/EHR

Not every system marketed as an RCM software solution delivers true financial improvement. Some platforms automate surface-level tasks but still leave gaps in claim submission, denial management tools, or audit trail visibility.
To avoid another tech purchase that still requires workarounds, assess each vendor against real operational needs rather than feature brochures. The following capabilities set apart healthcare revenue cycle management software providers that contribute to cash flow rather than maintenance overhead.
1. Seamless Integration and Data Flow
The handoff between clinical notes and billing must be frictionless. Every action, from patient intake to eligibility verification, coding suggestions and ERA posting, should move without exporting files or double entries. Ask vendors how their system handles EMR integration and what standards they support for data interoperability, including FHIR and HL7.
2. Automation Tools
Manual follow-ups slow collections. Look for embedded rules engines that enforce payer requirements automatically, check authorizations at scheduling and scrub claims before submission. Platforms with predictive edits reduce denial volume by catching missing attachments, mismatched IDs or incomplete charge capture before they leave your system.
3. Strong Reporting and Dashboards
You can’t improve what you can’t see. Live panels displaying AR days, denial categories, first-pass yield and collection rate trends make performance monitoring a daily habit instead of a quarterly cleanup. A usable dashboard should allow filtering by provider, payer, CPT group or claim status without exporting into spreadsheets.
4. Deployment Options
Cost and maintenance expectations change depending on the setup. Cloud RCM models offer faster scalability with automatic updates, while on-prem configurations give local database control. Practices with multiple locations may opt for hybrid deployment, using hosted RCM with local data archiving.
5. Security and Support
Any RCM platforms handling PHI must offer encryption in transit and at rest, documented audit trails, role-based access, and full HIPAA adherence. Financial systems run on uptime and response time, so prioritize healthcare revenue cycle management software providers with trained support teams who understand payer logic instead of general IT representatives.
RCM Software Solutions vs Pure EMR/EHR Systems
Not every practice follows the same structure, so technology shouldn’t force a single model. Some teams prefer one unified platform for clinical documentation and billing. Others separate both to gain better control over performance metrics. When comparing healthcare revenue cycle management software providers, it helps to understand how these system types differ in function, flexibility, and long-term scalability.
1. Stand-Alone RCM Platforms
These systems are built primarily for billing performance. They often support multi-EMR integrations, stronger denial management tools, advanced claim submission routing and payer-specific logic. Stand-alone RCM works best for groups with mixed specialties or outsourced billing relationships where analytics and audit tracking take priority over physician-facing usability.
2. EMR/EHR with Built-In RCM
All-in-one platforms reduce toggling between clinical notes and billing workflows. Charge data, coding suggestions and claim submission sync without external interfaces. While these systems may lack deeper analytics, they provide tighter alignment between providers, coders and billers, particularly in smaller practices with shared roles.
Here’s a comparison table that simplifies the differences between RCM software and EMR/EHR systems
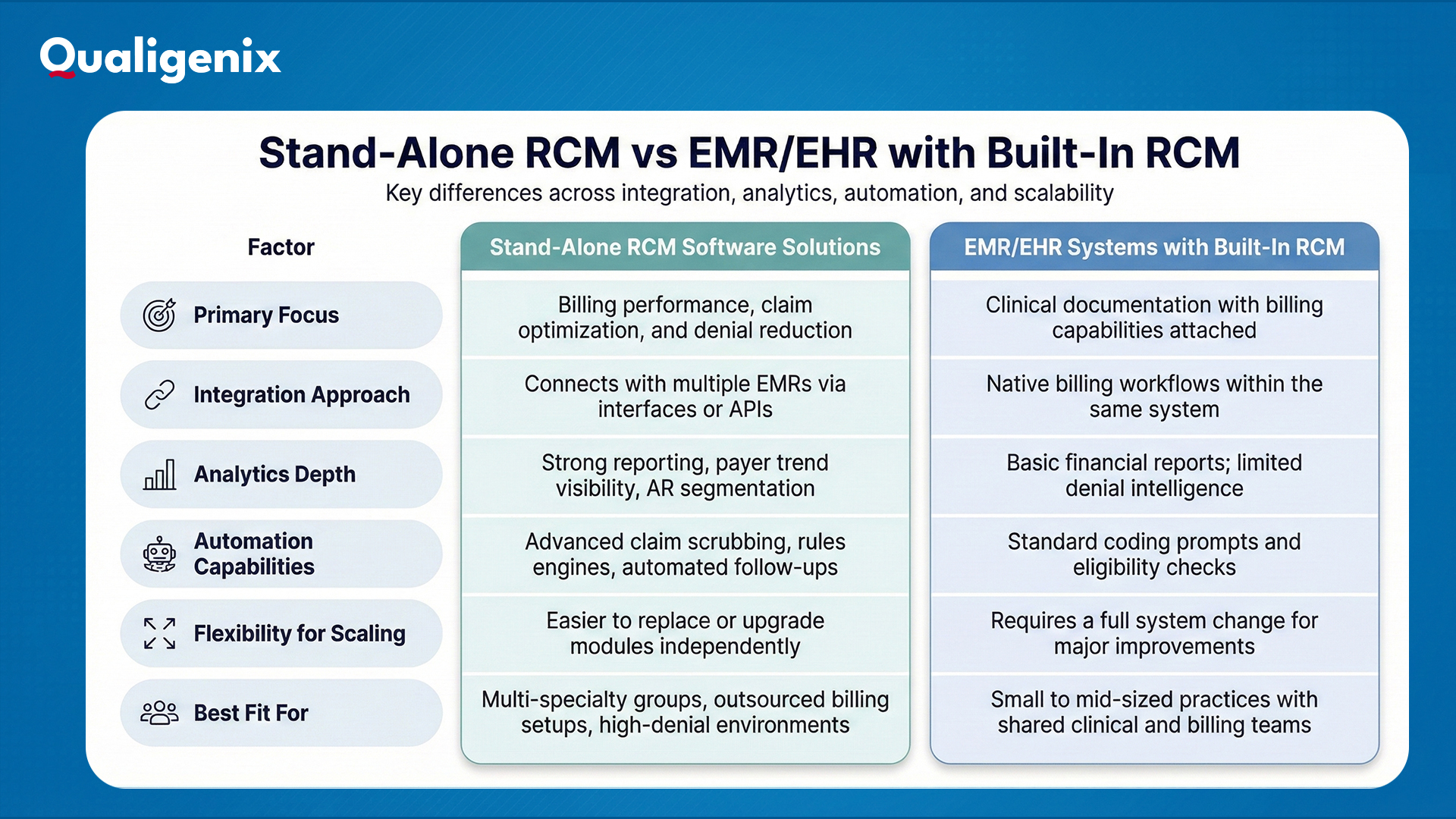
Then, we have hybrid solutions. Some RCM platforms allow modular configuration, where practices can use core EMR functions while plugging in advanced revenue cycle tools from external healthcare revenue cycle management software providers. This setup allows gradual upgrades without a disruptive platform overhaul.
Criteria and Checklist for Evaluating Providers
Comparing healthcare revenue cycle management software providers often becomes a feature chase, but real performance comes down to cost, usability and long-term support. Instead of relying on sales demos, anchor your decision to measurable checkpoints that affect daily billing outcomes.
- Total Cost of Ownership
License fees are only one layer. Factor in data migration, training, interface setup, support renewals and upgrade charges. A lower upfront fee can still cost more if staff spend extra hours compensating for gaps in functionality.
- Vendor Track Record
Prioritize providers with published success stories in your specialty or claim volume range. Look for case studies that disclose improved first-pass yield or AR reduction, not generic satisfaction quotes.
- User Experience
Coders, front-desk teams and billers should complete actions without multi-screen detours. A system that burdens one department will eventually slow everyone else. Ask current users how long it takes to post an ERA, reprocess edits or review denials.
- Interoperability
Systems must connect without custom scripting. Confirm whether the platform supports FHIR, HL7 or API-based EMR integration. Compatibility with clearinghouses and payer portals determines how quickly claims move through review.
How Qualigenix Helps Choose the Right Healthcare Revenue Cycle Management Software
Selecting an RCM platform directly affects documentation accuracy, coding compliance, reimbursement timelines, and staff workload. Qualigenix evaluates your current EMR/EHR setup, payer mix, claim volume, and denial history to shortlist RCM vendors that align with your operational goals.
Instead of generic demos, you get ROI-backed recommendations tied to measurable outcomes like AR reduction, first-pass claim acceptance, and clean claim rate improvement.
Most firms only assess billing inefficiencies or only review clinical workflows; we do both. By evaluating how documentation flows from charting to claims submission, we ensure that your EMR/EHR and RCM system operate as one ecosystem. The result is fewer touchpoints, fewer handoffs, and higher reimbursement velocity.
Also, instead of vague vendor pitches, you receive quantified comparisons, features, contract terms, clearinghouse fees, denial prevention modules, and support SLAs. Every recommendation is benchmarked against your current AR days, denial rates, and collection percentages, so you know exactly what impact to expect before signing.
How Do We Deliver?
Implementation is structured to prevent operational disruption. Core teams run parallel testing while your live billing continues uninterrupted. We ensure that your staff receives role-based training, followed by post-launch dashboards that track first-pass yield, AR aging, denial categorizations, and payer turnaround time in real time.
Conclusion
Software alone doesn’t fix revenue leaks. The right EMR/EHR or RCM platform only works when it supports how your team codes, bills, and follows up on claims. A strong system boosts clean-claim submission, trims AR days, and eliminates rework. Instead of guessing which vendor fits, work with specialists like Qualigenix to turn your software investment into higher collections and faster reimbursements.
FAQs
1. How long should EMR/EHR implementation take?
Most practices complete implementation within 3 – 9 months. Smaller clinics move faster, while multi-specialty groups take longer due to data volume, interface builds, and provider training requirements.
2. Can I migrate from my current EMR without disrupting billing?
Yes, as long as migration includes parallel claims processing, historical data mapping, and end-to-end testing before the switch. The goal is to flip systems without losing active claims or payment follow-ups.
3. What savings can I expect after upgrading my RCM software?
Most organizations report 15–30% fewer denials and faster payments within the first quarter. Additional gains come from reduced manual work and clearer insight into underperforming payers.
4. Should I prioritize cloud or on-premise?
Cloud systems update automatically and scale with growing patient volume. On-premise offers in-house control, but maintenance and upgrades become your team’s responsibility.
5. Which integrations matter most for RCM-centric EMR/EHR?
Eligibility checks, payer edits, coding suggestions, claim scrubbing, denial tagging, and automated ERA posting. Each reduces manual touchpoints and improves first-pass acceptance.