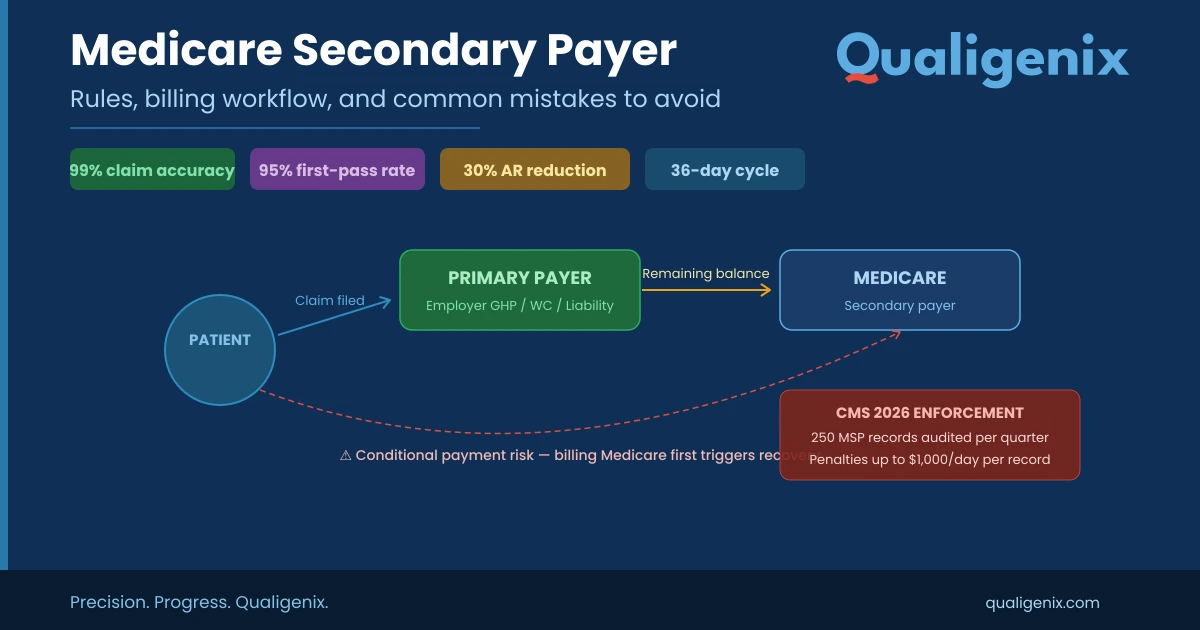
RCM Workflow Demystified: Must Track KPIs for Financial Health
The Qualigenix Editorial Team comprises certified medical billing professionals, CPC-credentialed coders, prior authorization specialists, and revenue cycle consultants with more than 40 years of combined hands-on experience serving solo physicians, group practices, hospitals, and ASCs across 38+ specialties in the United States. Every guide, article, and resource published on the Qualigenix blog is researched against current CMS guidelines, Federal Register notices, AMA policy updates, and payer-specific billing rules — and reviewed for compliance accuracy before publication. Our content reflects the same standards we apply to our client work: 99% claim accuracy, 95% first-pass acceptance, and a 30% average reduction in AR days.

A medical biller’s job begins even before the patient walks into the clinic. Before any appointment is confirmed, insurance verification and benefits checks set the stage for smooth billing later. Therefore, understanding what RCM KPIs are is important to measure how well this entire process, with verification, coding, billing, and collections, works in practice. The data tells its own story: claim denials climbed to 11.8% in 2024, up from 10.2% a few years ago, whereas top performers keep AR days under 40. Each missed check or delayed claim slows cash flow. This guide breaks down major RCM Key Performance Indicators (KPIs), 2025 benchmarks, and automation steps that can help keep your revenue cycle predictable and profitable.
What Are RCM KPIs & Why They Matter?
RCM KPIs show how well your team turns patient care into actual payments. From insurance verification to coding, billing, and collections, these numbers tell you how fast and accurately your process moves.
So when someone asks “what are RCM KPIs?”, a solid answer is: measurable metrics tied to each stage of the revenue cycle that help you gauge performance, spot bottlenecks, and guide process improvements. Metrics like clean claim rate, AR days, and denial rate give you a clear picture of performance at every step. When you track them consistently, you can see where money gets stuck and fix it before it slows you down.
The Financial Consequences of Poor KPI Scores
Strong KPI tracking keeps you informed, steady, and in control of your revenue. However, when KPIs slip, revenue follows, and the impact becomes visible at different stages:
- Every one percent increase in denial rate can mean thousands of dollars lost.
- Each extra day in accounts receivable locks up cash that should already be in your bank.
- Low clean claim rate adds unnecessary rework and delays payments.
Core Revenue Cycle KPI Categories
In every healthy revenue cycle, there are three KPI buckets you need to watch: Operational Efficiency Metrics, Financial Health Metrics, and Patient Responsibility Metrics. Each one ties directly to how smoothly money moves through your system and how much sticks where it should.
Operational Efficiency Metrics
- Clean Claim Rate / First-Pass Yield (FPY)
This measures the share of claims that sail through payers without edits or reworking. The industry standard is to aim at a 95 % clean claim rate, and top performers push toward 98 %. High FPY means fewer corrections, less back and forth, and faster payments.
- Days in Accounts Receivable (AR Days)
This tells you how long the payment is tied up. If your AR days extend past 40, or worse, cross 50, you’re facing real stress on cash flow.
- Discharged Not Final Billed (DNFB) Days
These are services rendered but not yet billed. Keep DNFB under 3 days if you can. Longer lags mean delayed revenue and hidden risk.
- Billing Lag / Unbilled Claims
This tracks the time between care delivery and billing. If that lag grows, you’ll see leakage in the pipeline; revenue waits longer to convert.
Financial Health Metrics
- Net Collection Rate (NCR)
This is how well you turn billed, allowable charges into collected dollars. The ideal benchmark is 95 percent or higher. A higher NCR shows efficiency and payer consistency.
- Cost-to-Collect
You want to keep what you spend collecting as low as possible. Industry norms suggest 2–5 % of collections for hospitals and practices. If your cost to collect is going higher, it means inefficiencies or too much manual labor.
- Denial Rate & Payer Rejection Rate
These measure how many claims are being denied on the first pass. A good benchmark is to stay under 5 – 10 % in total.
- Write-Offs & Revenue Leakage
This is the uncollected money that you’ve decided can’t be recovered. Monitoring it gives you a warning system: if write-offs rise, you’re letting value slip away.
Patient Responsibility Metrics
- Patient Payment Collection Rate
This measures how much of the patient’s balance your team collects. A higher rate shows strong communication and effective payment policies.
- Bad Debt Ratio
This shows the portion of patient balances that remain unpaid after all efforts. A rising bad debt ratio signals gaps in follow-up or patient engagement.
- Payment Plan Compliance Rate
If you offer installment plans, this metric tracks how many patients stick to their schedule. Poor compliance means more collection follow-ups, more write-offs, and a heavier burden on staff.
RCM KPI Benchmarks for 2025
Before you chase numbers, you need to know what “good” looks like. Benchmarks are important, as they help you see whether your performance is lagging, average, or leading.
Below is a table of target ranges for 2025, broken into front-end/mid-cycle, back-end/collections, and emerging priorities.
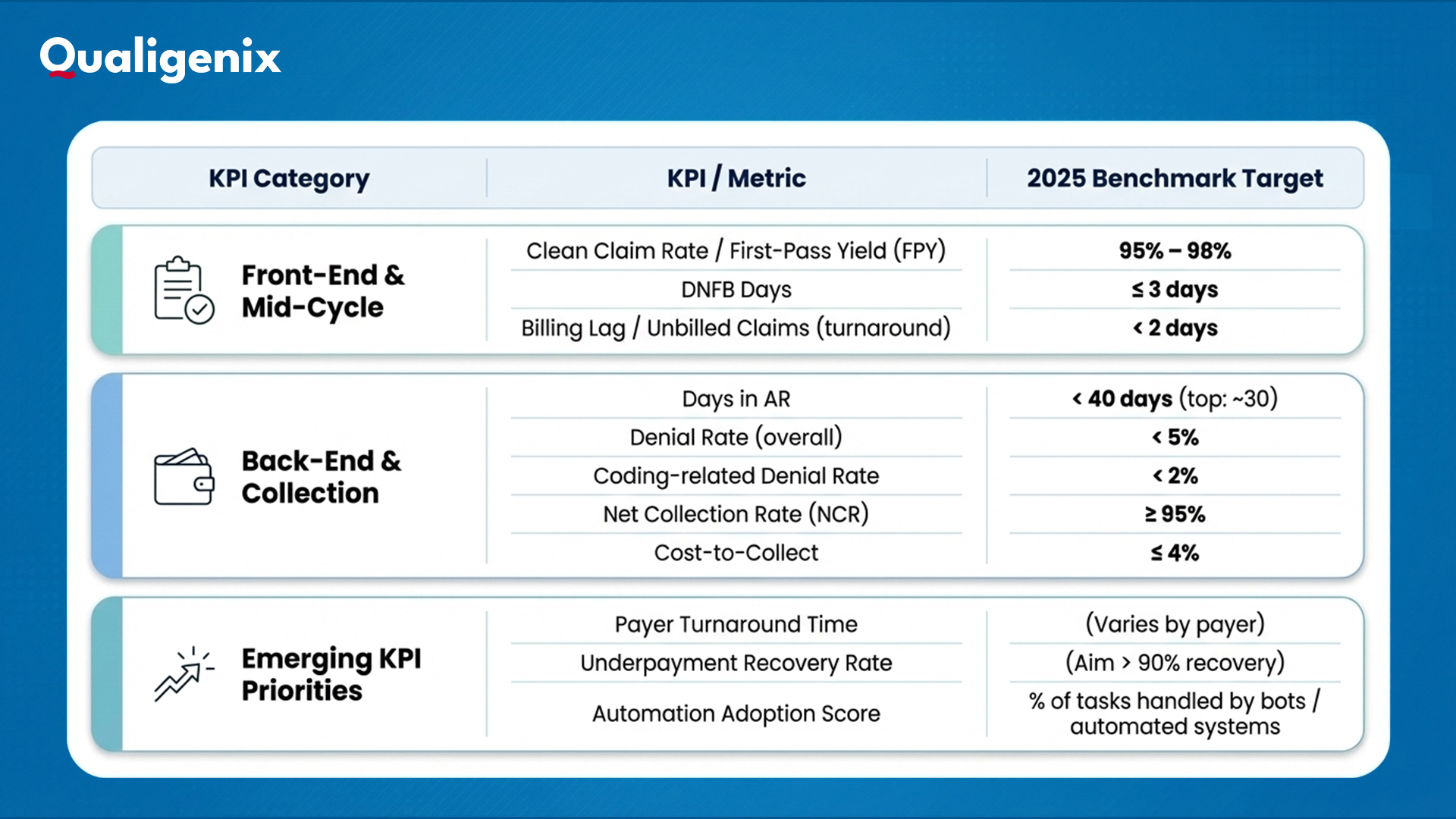

As you use these benchmarks, don’t treat them like rigid laws. Adjust for your payer mix, specialty mix, geography, and size. But if you’re far off these targets in one metric, you now know where to zoom in.
How to Measure and Improve RCM KPI Performance
Knowing the metrics is step one. Driving them upward is where real work begins. Let’s run through a practical framework to measure, monitor, and improve your RCM performance metrics, especially your revenue cycle KPIs, examples as AR days, clean claim rate, denial rate, cost-to-collect, etc.
Build a Centralized RCM Dashboard
Don’t spread your data across silos. Pull data from Electronic Health Record (EHR), claim systems, clearinghouse, and billing platforms into one unified dashboard. Use standard definitions so everyone agrees what “AR days” or “net collection rate” means. A single source of truth prevents confusion and allows trends to show clearly.
Assign Owners and Set SLAs
Each KPI should have an accountable owner (e.g., the billing director owns AR days, the claims manager owns denial rates). For each metric, set thresholds or alert levels. Automate notifications: if AR days climb beyond 45, flag the owner. That clarity pushes responsibility, not ambiguity.
Audit, Analyze, and Adjust Regularly
Metrics alone don’t solve problems. Review dashboards weekly (for operations) and monthly (for financials). Use payer-level heat maps to spot which insurers cause the most denials or delays. For repeated patterns, build root cause playbooks. For example, “coding mismatch for MRI claims” or “missing prior auth for imaging.” Use these playbooks whenever that issue resurfaces.
Automate High-Impact Tasks
Manual work eats time and invites error. Automate eligibility checks, prior authorization tracking, and ERA auto-posting. These bots reduce manual touches, improve first-pass yield, and lower your cost-to-collect. Over time, the automation adoption score itself becomes a KPI you track.
When you combine clear dashboards, ownership, root cause discipline, and automation, you turn passive measurement into active improvement. The difference becomes visible in lower denial rate, shorter AR days, and healthier margins.
Actionable Revenue Recovery Framework
Tracking RCM KPIs is only half the work. The real progress comes when you act on them. This framework turns your KPI list insights into concrete revenue recovery steps that protect margins and improve cash flow.
Identify Leakage Points
Start by using your KPI data to spot where revenue is slipping through the cracks. Common problem areas include unbilled claims, underpayments, and denials that were never appealed. A spike in DNFB days might mean clinical documentation is delayed, whereas a low net collection rate could indicate underpayments from payers. These red flags help you see where attention is needed most.
Prioritize High-Value Fixes
Not every issue deserves the same urgency. Focus first on metrics that directly affect your bottom line, such as your denial rate, AR days, and DNFB days. For example, reducing AR by just ten days can free up significant working capital. Fix recurring denial codes to recover thousands in missed revenue every quarter.
Continuous Feedback Loop
Share insights from denials, payment trends, and coding errors with your front-end and registration teams. This prevents the same mistakes from cycling through the system. Build monthly feedback meetings to review patterns and adjust workflows, so each cycle becomes more accurate and efficient.
How Qualigenix Elevates KPI Performance
Strong KPIs are built on consistent process, automation, and accountability, and that’s where Qualigenix delivers measurable results.
Expertise in KPI Optimization
Our team helps practices strengthen their clean claim rate, reduce AR days, and manage denials with data-backed precision. We apply analytics to uncover process gaps and align your workflows with payer requirements.
Proven Tools & Approach
We provide custom-built KPI dashboards, payer heat maps, and automation modules that simplify complex tasks like eligibility verification, claim scrubbing, and payment follow-ups. These tools transform reactive reporting into proactive revenue management.
Measurable Outcomes & Support Model
With our 30-60-90 day implementation plan, every client gets named KPI owners, performance SLAs, and monthly reviews. The results speak for themselves with higher first-pass yield, lower denial rates, and faster reimbursements. With Qualigenix, you gain a transparent, data-driven approach that keeps your revenue cycle steady and predictable.
Stay Ahead with Data-Driven RCM Performance!
A strong understanding of what RCM KPIs are turns billing from a routine task into a predictive system. Metrics such as clean claim rate, AR days, cost-to-collect, and denial rate reveal the true efficiency of your revenue cycle. Success in 2025 depends on accurate data and consistent measurement, not assumptions. Clear benchmarks, practical automation, and guidance from experts help healthcare providers strengthen reimbursements and maintain financial stability.
So, partner with Quaigenix to experience the real difference. When every metric is measured and managed, cash flow becomes predictable, denials fall, and the entire billing process works as smoothly as patient care itself.
FAQs
1. What are the most critical RCM KPIs to begin with?
The most critical RCM KPIs include clean claim rate, denial rate, AR days, and net collection rate. These metrics give a clear picture of revenue performance and help identify where billing delays or payment gaps occur most often.
2. How often should KPIs be reviewed?
Operational KPIs should be reviewed weekly to catch issues early. Financial KPIs should be reviewed monthly to track revenue movement. A quarterly review helps identify payer trends and confirm that improvements remain consistent across departments.
3. What clean claim rate is considered excellent in 2025?
A clean claim rate between 95 percent and 98 percent is considered excellent in 2025. Maintaining this range reduces rework, shortens payment cycles, and improves first pass resolution with payers.
4. How do high AR days hurt practices?
High AR days restrict cash availability and slow daily operations. As claims age, the risk of write offs and patient dissatisfaction increases. Keeping AR days under 40 supports stable cash flow and stronger financial health.
5. How can automation boost KPI performance?
Automation improves speed and consistency across the revenue cycle. Automated eligibility checks, prior authorization tracking, and claim status updates reduce manual errors, increase accuracy, and raise first pass yield significantly.