The Importance of Eligibility Checks and Benefit Verification in RCM
The Qualigenix Editorial Team comprises certified medical billing professionals, CPC-credentialed coders, prior authorization specialists, and revenue cycle consultants with more than 40 years of combined hands-on experience serving solo physicians, group practices, hospitals, and ASCs across 38+ specialties in the United States. Every guide, article, and resource published on the Qualigenix blog is researched against current CMS guidelines, Federal Register notices, AMA policy updates, and payer-specific billing rules — and reviewed for compliance accuracy before publication. Our content reflects the same standards we apply to our client work: 99% claim accuracy, 95% first-pass acceptance, and a 30% average reduction in AR days.

You would have likely seen how even well-run practices face delayed payments and denied claims. It mostly occurs because eligibility wasn’t checked properly. In fact, problems in registration and eligibility checks cause 26.6% of claim denials. That’s a huge leak you can seal early with eligibility verification in medical billing.
Imagine verifying a patient’s insurance coverage, deductible, copay, and coordination of benefits (COB) before services begin. With tools like EDI 270/271, real-time or batch eligibility checks, and automated verification workflows, your team catches issues early, collects at the point of service, and avoids costly rework. In this guide, you’ll see how a solid benefit verification checklist transforms revenue cycles, strengthens cash flow, and improves patient satisfaction, even long before a claim is ever submitted.
What are Eligibility Checks & Benefit Verification in RCM
Eligibility checks and benefit verification are the foundation of a healthy revenue cycle. Without them, even the most accurate coding and billing can fail because claims may be denied for reasons that could have been caught before the patient visit.
Definition & Purpose
Eligibility verification in medical billing means confirming that a patient’s insurance coverage is active on the date of service and that the plan will pay for the care being provided. Benefit verification goes a step further. It identifies exactly which services are covered and under what conditions. The main purpose is to prevent claim denials, avoid payment delays, and ensure patients understand their financial responsibilities before treatment begins.
Components of Benefit Verification
A complete benefit verification checklist includes:
- Deductibles: How much the patient must pay before coverage begins.
Copays: Fixed fees the patient owes at the time of service. - Coinsurance: The patient’s share of the bill after the deductible.
- Exclusions: Services not covered by the plan.
- Prior authorization requirements: Procedures that need payer approval in advance.
- Coordination of benefits (COB): Determining payment order if multiple plans exist.
How It Fits Into the RCM Workflow
Eligibility checks happen early, during patient registration or appointment scheduling, and may continue with real-time checks at the point of care. This information ensures claims submitted later include the correct payer details and patient responsibility amounts. When done accurately, this step reduces rejections, improves first-pass yield, and sets the rest of the revenue cycle up for success.
Here’s the eligibility & benefit verification workflow:
- Patient Registration: Collect insurance details and demographics.
- Scheduling: Verify active coverage and check plan rules.
- Eligibility Check (EDI 270/271): Confirm plan status, COB, and service coverage.
- Benefit Verification: Review deductibles, copays, coinsurance, and prior auth needs.
- Point-of-Care Confirmation: Re-verify benefits for walk-ins or same-day changes.
- Claims Submission: Use verified details for cleaner, faster-paying claims.
For example, if a patient’s plan requires prior authorization for an MRI, verifying that upfront prevents a denied claim later. Similarly, confirming deductible status helps you collect accurate payments at the time of service (POS collections) instead of chasing balances afterward.
Why Eligibility & Benefit Verification Matter
Eligibility and benefit checks might feel like an early step, but they shape the entire revenue cycle. Skipping them or treating them lightly almost always shows up later as denied claims, lost revenue, and frustrated patients.
Prevent Claim Denials & Rework
Most claim denials trace back to simple issues like inactive coverage or unmet deductibles. By verifying insurance eligibility before the visit, you catch those problems upfront. That means fewer rejected claims, less rework for your team, and faster payments.
Improve Cash Flow & Reduce AR Days
When you know coverage details before care is delivered, billing is more accurate from the start. Clean claims move through payer systems faster, reducing AR days and giving you a steadier cash flow.
Enhance Patient Experience & Trust
Patients want cost transparency. Confirming benefits and discussing copays or deductibles before the visit avoids billing surprises later. That clarity builds trust and improves how patients view your practice.
Boost Operational Efficiency
Your staff spends less time chasing payers or fixing errors when eligibility checks happen early. That frees them to focus on more valuable work and keeps revenue moving without interruptions.
Mitigate Audit Risk & Maintain Compliance
Accurate benefits coverage verification ensures your claims align with payer policies and regulatory requirements. That lowers your audit risk and keeps you compliant, especially when rules change mid-year or vary by state.
Benefit Verification Checklist: What You Must Verify

Before every visit, running through a structured benefit verification checklist helps you catch errors, prevent denials, and set clear expectations with patients. Here’s what you should always confirm during the insurance eligibility verification process:
-
Policy Status & Effective Dates
Verify that the policy is active on the date of service and hasn’t lapsed or been terminated. Check renewal periods to avoid submitting claims on inactive coverage.
-
Covered Services & Exclusions
Confirm which procedures, treatments, and medications are covered under the plan and note any exclusions or limitations. This ensures services provided are reimbursable.
-
Deductibles, Copays, Co-insurance
Review the patient’s remaining deductible amount, required copays, and percentage of coinsurance. This helps you collect the correct amount at the point of service.
-
Preauthorization & Referral Requirements
Identify services needing prior approval or referrals. Missing preauthorization is a leading cause of claim denials, especially for imaging or surgical procedures.
-
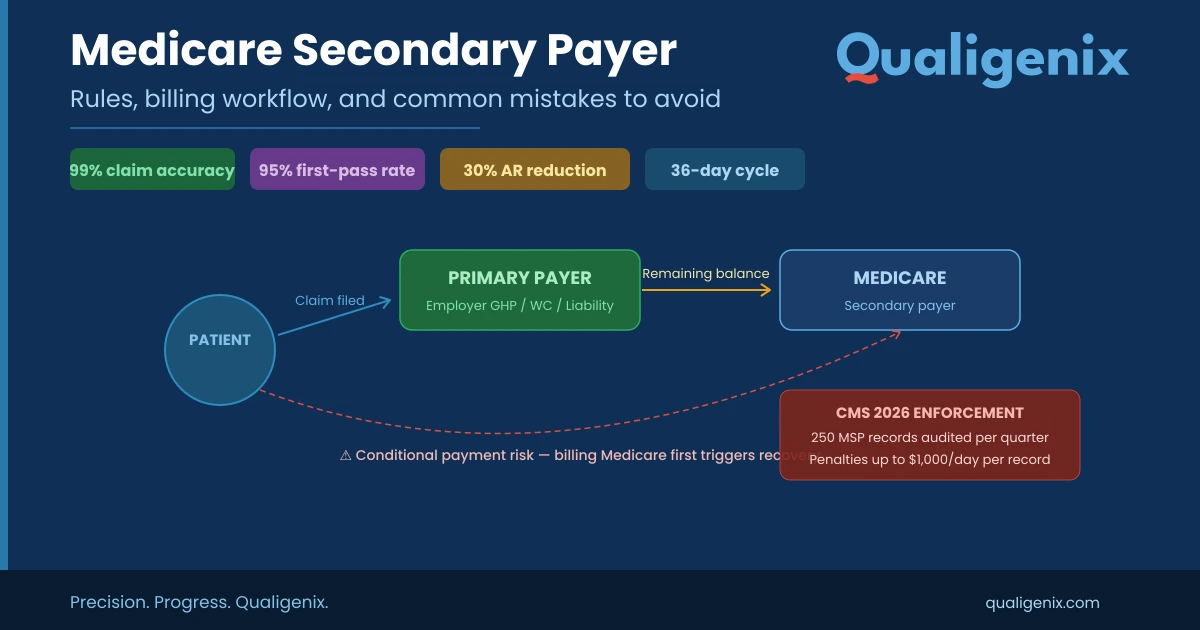
Coordination of Benefits (COB) / Secondary Coverage
If multiple plans exist, determine the primary and secondary payers to ensure proper payment order and prevent delays.
-
Out-of-Network vs In-Network Limitations
Check network participation status for the provider and facility. Out-of-network care often has higher patient costs or reduced coverage.
-
Limits, Maximums & Frequency Caps
Verify any annual or lifetime coverage limits and frequency restrictions, such as the number of therapy visits or lab tests covered per year.
-
Patient Financial Responsibility Amounts
Calculate what portion of the cost the patient must pay out of pocket. Sharing this information upfront avoids billing disputes and builds trust.
-
Benefit Verification Documentation & Audit Trail
Maintain detailed records of all verification steps, including call reference numbers or EDI 270/271 transaction reports. These audit trails protect you in case of payer disputes or compliance checks.
Pro Tip: You can also automate this checklist through eligibility workflow automation tools to reduce manual errors, speed up verification, and ensure every claim is backed by complete and accurate benefit data.
Tools & Methods for Verification
You have several options when it comes to insurance eligibility checks. And using more than one often gives the best results. These tools reduce errors, speed up billing, and improve how quickly you get paid.
Real-Time EDI Checks (270/271)
The fastest way to verify coverage is through EDI 270/271 transactions. These connect directly with payer systems and return eligibility data in seconds, so you know plan status, copays, and deductibles right away.
Batch Eligibility Queries
For large patient volumes, batch eligibility lets you process hundreds of checks at once, usually overnight. It’s efficient for busy practices but should be paired with real-time checks for last-minute updates.
Payer Portal / API Integration
Logging into payer portals or integrating with their APIs gives deeper plan details, like prior authorization requirements or COB information, that automated responses sometimes miss.
Automated Verification Engines & Workflow Automation
Automated tools pull patient data, run eligibility queries, and flag mismatches without manual effort. They also create built-in verification audit trails for compliance and quality tracking.
Manual Confirmation / Payer Calls as Fallback
Some payers don’t fully support automation. Calling them directly may be slower, but it ensures you’re working with the most current information before billing.
Eligibility Monitoring & Reverification at Service Time
Coverage can change between scheduling and the appointment. Always recheck eligibility at the point of service, especially for high-cost procedures, to avoid unexpected denials.
Best Practices & Common Pitfalls
Eligibility verification isn’t just a one-time task. It is a complete workflow. Here are a few best practices you can follow to avoid the mistakes that slow payments and frustrate patients:
Verify At Multiple Touchpoints
Check eligibility at scheduling, again at check-in, and once more before any high-value service. This triple check catches plan changes that happen between booking and visit day.
Use Automation, Not Just Manual Processes
Manual checks are prone to errors. Automation ensures consistent data capture, faster responses, and built-in logs, freeing staff to handle exceptions instead of routine work.
Keep Data Clean & Up-To-Date
Incorrect demographics, outdated policy numbers, or old group IDs can cause denials. Validate patient information at every encounter to keep eligibility data accurate.
Train Staff on Verification Rules & Payer Variances
Every payer has quirks. Training your team to understand different payer rules, prior authorization triggers, and COB logic reduces rework and improves claim success.
Avoid “Assume Coverage” Mindset
Never assume an existing patient’s plan hasn’t changed. Even long-term patients switch plans midyear, and failing to reverify leads to preventable denials.
Audit Verification Logs & Measure Accuracy
Regularly review your verification records and track metrics like first-pass yield and eligibility-related denial rates. These audits show where workflows are strong and where they need tightening.
How Qualigenix Strengthens Eligibility Verification in Your RCM

Why Qualigenix Is Well-Positioned
Qualigenix brings deep expertise in automation, payer-specific rules, and verification accuracy. Our team understands how eligibility decisions impact cash flow, patient experience, and compliance, and we design workflows to prevent errors before they happen.
What You Receive
With Qualigenix, you get real-time and batch verification workflows configured for your systems, a detailed benefit verification checklist customised to your specialties, robust exception-handling protocols, and monitoring dashboards that give you full visibility into verification outcomes.
How We Deliver Impact
Our approach reduces denial rates linked to eligibility errors, boosts first-pass yield, cuts costly rework, and improves patient communication about financial responsibility. The result is a smoother revenue cycle and faster, more predictable payments.
Turn Eligibility Verification Into a Revenue Strength with Qualigenix!
Eligibility verification in medical billing isn’t optional anymore. It is the backbone of a revenue cycle that works. When done right, eligibility checks and benefit verification reduce denials, accelerate payments, save staff hours, and build patient trust. But doing it right takes the right systems and expertise.
Qualigenix helps you build that foundation, from automation setup to audit-ready documentation, so verification becomes a strength, not a risk. Book a demo at Qualigenix today to see how we can transform your eligibility workflows and turn verification into one of your biggest revenue drivers.
FAQs
1. When in the workflow should eligibility be verified?
Eligibility should be verified at three points. First during appointment scheduling. Second before the service to catch plan or coverage changes. Third at check in for high cost or complex procedures. This layered approach lowers denials and improves patient payment accuracy.
2. How much do benefits affect claim acceptance?
Incorrect benefit details contribute to nearly 25 percent to 30 percent of claim denials. These issues are common with prior authorizations, coverage limits, and exclusions. Early benefit verification helps claims meet payer rules and move through adjudication without delays.
3. Is real time eligibility verification necessary?
Real time verification is not mandatory, but it is the fastest way to confirm coverage, copays, and deductibles. Combining real time checks with batch verification or payer API connections keeps eligibility data accurate and current.
4. How often should eligibility re verification occur?
Eligibility should be checked at every visit for patients with frequent insurance changes or complex care plans. For stable patients, quarterly verification is usually sufficient to catch renewals, benefit updates, or new authorization requirements.
5. What metric improves most with eligibility verification?
Strong eligibility verification improves first pass clean claim rates beyond 95 percent, reduces denials by 20 percent to 30 percent, shortens AR days, and lowers staff rework. These improvements create faster and more predictable revenue cycles.