Behavioral Health Billing Services That Maximize Every Reimbursement
Experience smarter behavioral health revenue cycle management with Qualigenix — built for compliance, speed, and results.
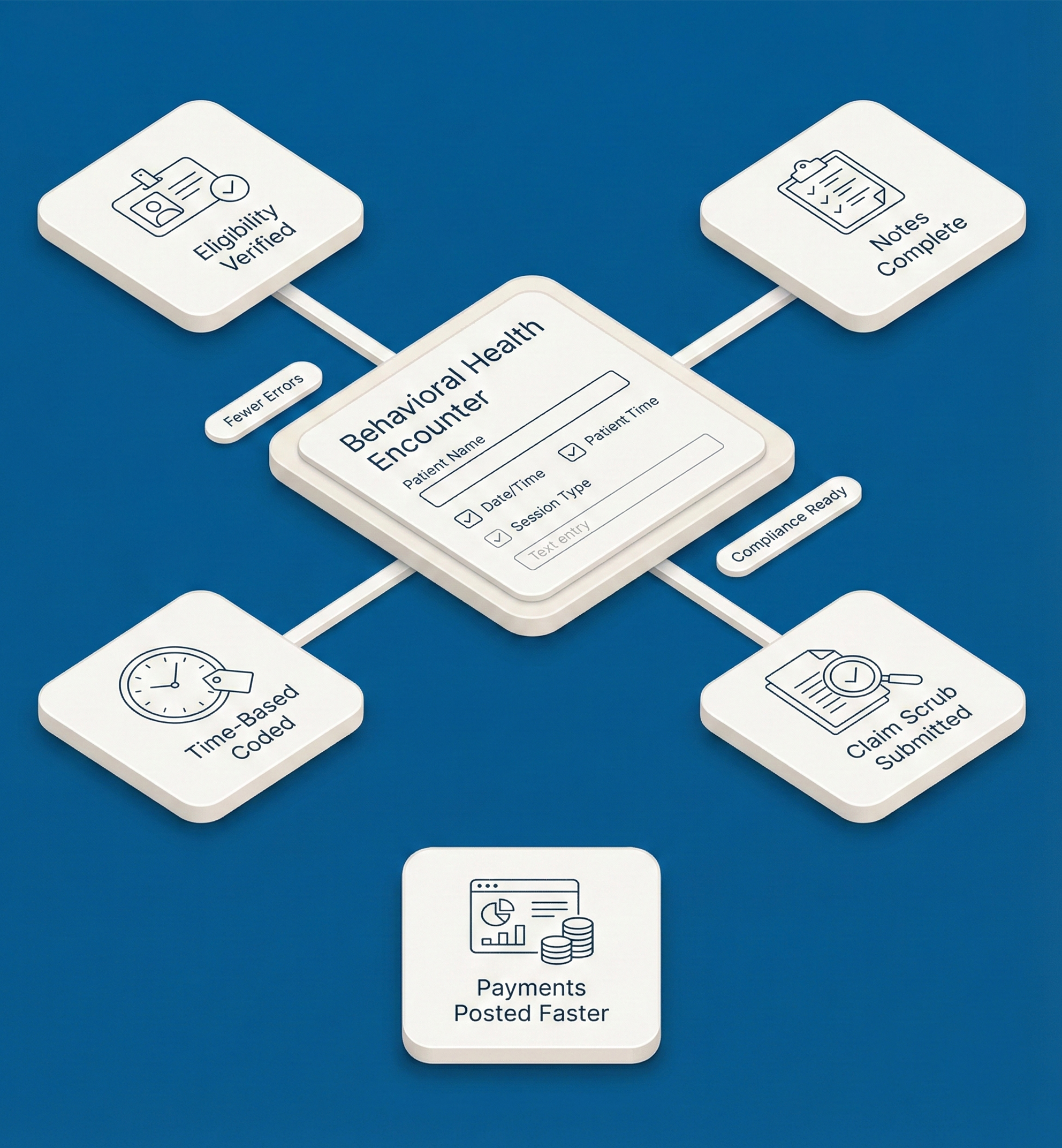

Behavioral Health Billing Services That Simplify Every Step of Your Revenue Cycle
Qualigenix delivers behavioral health billing solutions designed for accuracy, and compliance—reducing claim errors by over 30% and helping practices get paid faster with zero administrative burden.
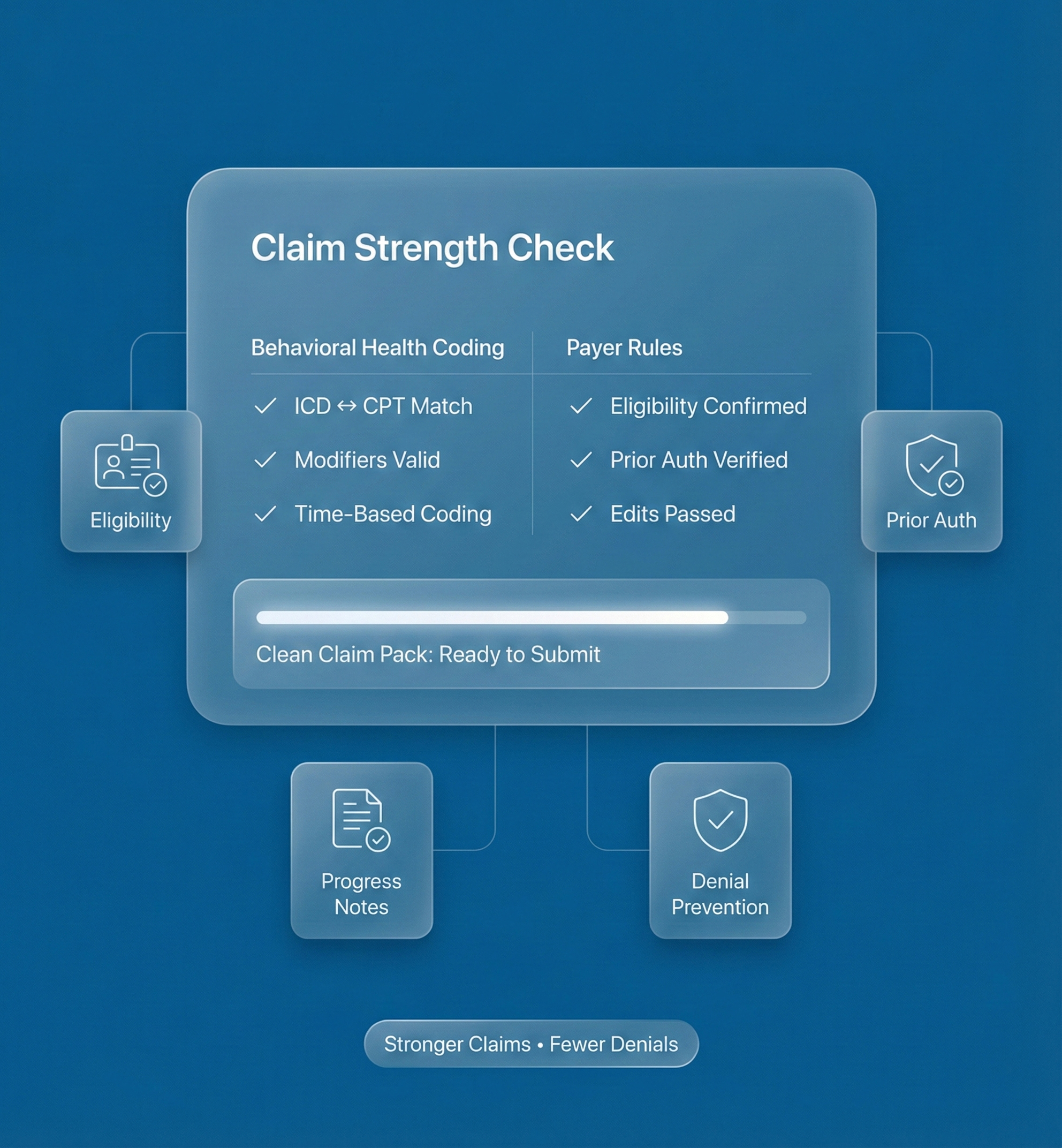
Behavioral Health Billing Services That Strengthen Every Claim You Submit
Our team applies precise coding and payer-specific rules to behavioral health encounters—cutting avoidable denials by 20% on average.
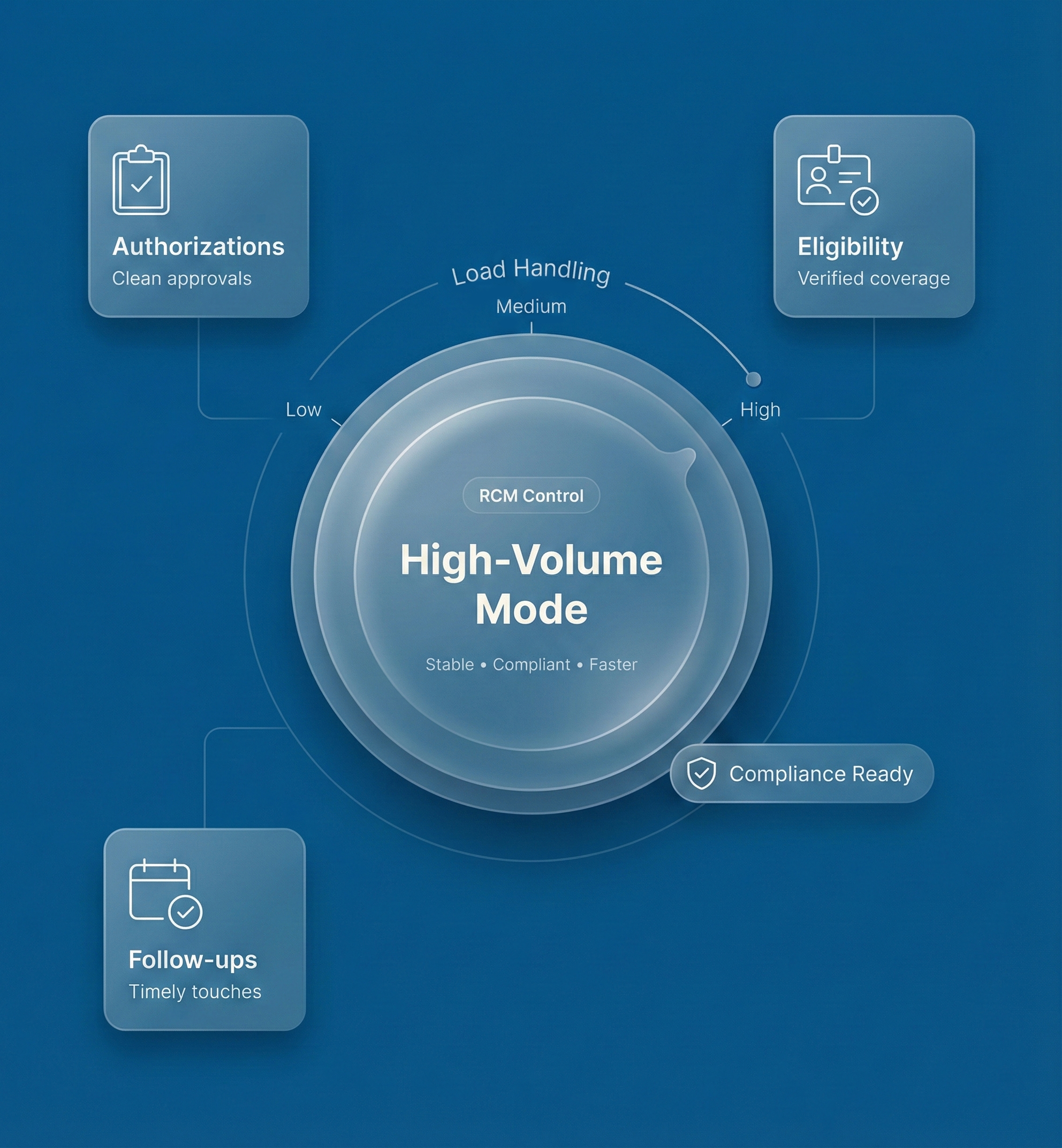
Behavioral Health Revenue Cycle Management Built for High-Volume Practices
We streamline authorizations, eligibility, and follow-ups so behavioral health groups stay compliant and get paid faster without admin overload.
Behavioral Health Billing Company Support That Eliminates Documentation Gaps
We review provider notes in real time to ensure every counseling, psychotherapy, and telehealth session is fully billable and audit-ready.
End-to-End Behavioral Health Billing Services That Keep Your Revenue Flowing
Accurate Coding & Charge Entry
Ensure error-free submissions with expert-led behavioral health coding services that boost claim accuracy and cut denials by up to 28%.
Explore SolutionsSmarter Claims Submission
Streamline billing with advanced behavioral health claims management that cuts denials and speeds up payments by 20%.
Explore SolutionsFaster Reimbursement Process
Achieve consistent cash flow through a transparent behavioral health reimbursement process optimized for quick, accurate payouts.
Explore SolutionsIntegrated Practice Management
Gain end-to-end visibility with behavioral health practice management that connects scheduling, billing, and reporting seamlessly.
Explore SolutionsBilling Workflows
Enhance productivity using behavioral health billing that minimizes manual effort and ensures compliance.
Explore SolutionsQuick Credentialing Assistance
Simplify provider onboarding with reliable behavioral health credentialing that expedites approvals and payer enrollments.
Explore SolutionsWhat Makes Our Behavioral Health Billing Company Stand Out
Denial Management Expertise
Reduce rejections with proactive denial management for behavioral health strategies.
Explore SolutionsBilling Efficiency
Streamline workflows through intelligent behavioral health billing tools.
Explore SolutionsUnmatched Coding Accuracy
Enhance claims with certified behavioral health coding services for zero errors.
Explore SolutionsHIPAA-Compliant Operations
Ensure data safety with fully HIPAA compliant behavioral health billing systems.
Explore SolutionsCredentialing Support Made Easy
Accelerate onboarding via smooth behavioral health credentialing processes.
Explore SolutionsProven Expertise That Transforms Behavioral Health Revenue Outcomes



Billing Expertise Across Every Behavioral Health Specialty
Mental Health
Neurology
Pediatrics
Family Practice
Primary Care
Internal Medicine
Emergency Medicine
Sleep Medicine
Pain Management
Occupational Health
Frequently Asked Questions
What makes behavioral health billing services different from general medical billing?
Behavioral health billing services require deeper coding precision, compliance tracking, and tailored claim handling to manage therapy sessions and multiple payer types effectively.
How does behavioral health revenue cycle management improve collection efficiency?
It streamlines every stage, from eligibility checks to denial follow-ups — ensuring behavioral health providers receive faster, more consistent reimbursements.
How do behavioral health billing services handle multi-visit therapy claims effectively?
Qualigenix’s behavioral health billing services use coding checks and session tracking to ensure accuracy across recurring therapy claims and multi-provider visits.
What makes behavioral health revenue cycle management more complex than general RCM?
Behavioral health revenue cycle management involves multi-tier payer policies, time-based billing codes, and varying documentation rules that require domain-specific expertise.
Why is partnering with a behavioral health billing company crucial for small practices?
A behavioral health billing company like Qualigenix helps smaller providers manage claim volumes, compliance updates, and staffing gaps without impacting cash flow.
How does Qualigenix maintain mental health billing compliance for high-volume practices?
Qualigenix integrates compliance checks within every claim cycle to ensure each submission meets HIPAA and payer-specific mental health billing compliance standards.
How to improve denial prevention in behavioral health billing?
Claim scrubbing, code validation, and real-time error alerts minimize denials and enhance accuracy throughout the behavioral health billing process.
What reporting insights does Qualigenix provide to behavioral health providers?
Qualigenix delivers weekly and monthly dashboards showing collection rates, denial trends, and clean claim percentages to optimize billing performance.