Denial Management in Medical Billing: 7 Common Causes
The Qualigenix Editorial Team comprises certified medical billing professionals, CPC-credentialed coders, prior authorization specialists, and revenue cycle consultants with more than 40 years of combined hands-on experience serving solo physicians, group practices, hospitals, and ASCs across 38+ specialties in the United States. Every guide, article, and resource published on the Qualigenix blog is researched against current CMS guidelines, Federal Register notices, AMA policy updates, and payer-specific billing rules — and reviewed for compliance accuracy before publication. Our content reflects the same standards we apply to our client work: 99% claim accuracy, 95% first-pass acceptance, and a 30% average reduction in AR days.

A patient visits your clinic, receives care, and leaves reassured. The service is documented, the claim is submitted, and everything appears complete. Weeks later, the payment does not arrive. Instead, the claim is denied, flagged for a missing modifier, an eligibility mismatch, or insufficient documentation.
Individually, medical billing claim denials may seem minor. In reality, even a small denial rate can translate into substantial financial loss when applied across thousands of claims. With payers increasing automated reviews and tightening reimbursement rules, denial volumes continue to rise, placing sustained pressure on cash flow and revenue cycle performance. This is where denial management in medical billing becomes critical. In this article, we will learn more about the causes that are related to the denial of a medical bill.
What Is Denial Management in Medical Billing?
Denial management in medical billing refers to the systematic process of identifying, analysing, correcting, and preventing denied claims throughout the revenue cycle. Its objective is twofold: recover revenue from denied claims and reduce the likelihood of similar denials occurring in the future. A comprehensive denial management process typically includes:
- Tracking denied claims across payers and service lines
- Analysing denial codes and explanations of benefits (EOBs)
- Identifying claim denial causes such as coding errors, eligibility issues, or documentation gaps
- Correcting errors and resubmitting claims or filing appeals
- Monitoring trends to address recurring weaknesses in workflows
Effective denial management does not operate in isolation. It connects front-end processes, such as patient registration, eligibility verification, and prior authorization, with back-end functions like coding, billing, and collections. When denial data is used strategically, it becomes a powerful tool for improving overall revenue cycle performance.
Difference Between Claim Rejections and Denials
Understanding the difference between claim rejections and denials is essential for prioritising recovery efforts and designing effective workflows.
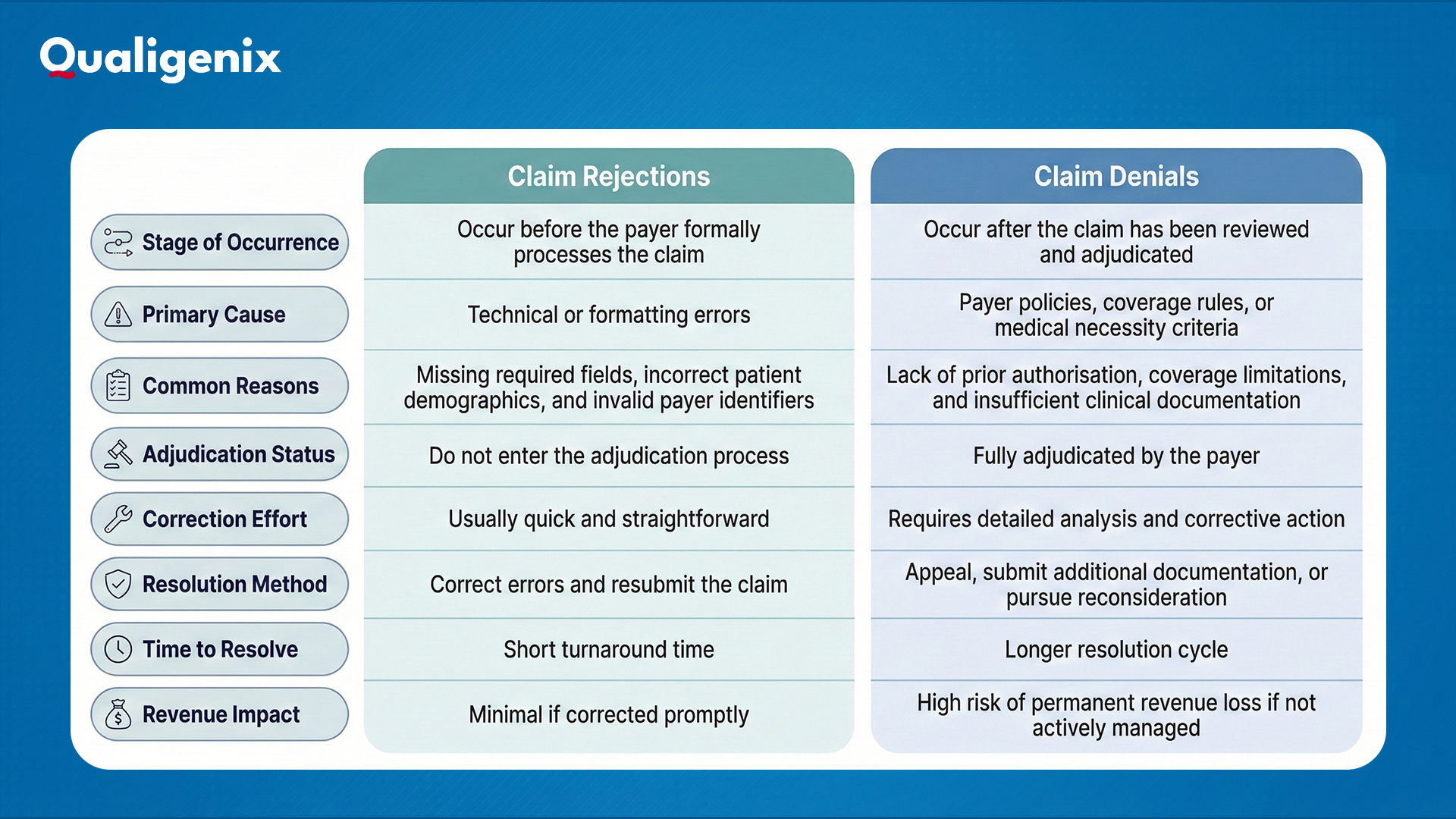
The distinction matters because denials require more time, deeper investigation, and often formal appeals. Without a structured denial management approach, denied claims are far more likely to result in permanent revenue loss.
7 Common Causes of Medical Billing Claim Denials
Denials often feel complicated when you’re dealing with them claim by claim. But when you step back and look at the bigger picture, most medical billing denials come from the same handful of issues repeating again and again. Below are the 7 common patterns of early and tightening processes upstream to prevent them from happening in the first place.
1. Incorrect or Missing Patient Information
Incorrect or incomplete patient information remains one of the most frequent causes of claim denials. Errors involving patient names, dates of birth, policy numbers, group numbers, or payer details can cause claims to fail automated payer checks immediately.
Patient demographic errors typically originate at the registration or scheduling stage. When front-end data capture is rushed or verification steps are skipped, errors flow downstream into billing and result in denials that could have been prevented. Implementing robust patient information verification processes before claim submission significantly reduces this category of denial.
2. Coding Errors and Missing Modifiers
Coding errors are a leading contributor to both claim rejections and denials. These errors include incorrect Current Procedural Terminology (CPT), International Classification of Diseases (ICD), Healthcare Common Procedure Coding Systemcodes (HCPCS), outdated code usage, unbundling issues, and missing or incorrect modifiers.
Payers rely on precise coding to determine coverage eligibility, reimbursement levels, and compliance with policy rules. Even small inaccuracies can trigger denials, underpayments, or requests for additional documentation.
3. Missing Prior Authorization
Prior authorization denials occur when services requiring pre-approval are rendered without obtaining or properly documenting authorization. This is especially common for imaging, surgical procedures, specialty consultations, and high-cost treatments.
In many cases, authorization may have been requested but not approved in time, incorrectly documented, or submitted under the wrong payer guidelines. Unfortunately, many payers do not allow retroactive authorization, making these denials difficult to overturn.
4. Insurance Eligibility and Coverage Issues
Eligibility issues arise when services are billed for patients whose insurance coverage is inactive, expired, or does not include the billed service. Insurance coverage issues also occur when benefit limits are exceeded or when services are excluded under the patient’s plan.
These denials are often preventable through real-time eligibility verification prior to service delivery. Failure to verify coverage places financial risk on providers and can lead to patient dissatisfaction when balances shift unexpectedly. Eligibility verification is a foundational element of strong denial management in medical billing.
5. Timely Filing and Late Submissions
Every payer enforces timely filing limits that define how long providers have to submit claims after the date of service. Missing these deadlines results in automatic denials, regardless of claim accuracy or medical necessity.
Late submissions are commonly caused by internal workflow inefficiencies, unresolved claim edits, documentation delays, or a lack of follow-up on rejected claims. Once the timely filing window closes, recovery options become extremely limited. Maintaining disciplined submission timelines and automated claim tracking is critical to preventing these denials.
6. Duplicate Claims
Duplicate claims occur when the same service is billed more than once, either intentionally or unintentionally. This often happens when claims are resubmitted without proper tracking or when payment status is unclear.
Payers automatically deny duplicate claims, which increases administrative workload and delays legitimate reimbursement. Over time, frequent duplicate submissions can also flag provider accounts for increased scrutiny. Clear claim status monitoring and structured resubmission protocols help eliminate unnecessary duplicate claims.
7. Lack of Medical Necessity Documentation
Denials for lack of medical necessity occur when clinical documentation does not sufficiently justify the service provided. Even when services are clinically appropriate, missing or vague documentation can result in nonpayment.
Documentation gaps may include incomplete progress notes, missing diagnostic support, or a lack of alignment between diagnosis codes and procedures performed. Payers expect documentation to clearly demonstrate why a service was required based on the patient’s condition. Strong, consistent clinical documentation is essential for defending medical necessity during audits and appeals.
How Qualigenix Helps With Denial Management in Medical Billing?

Qualigenix addresses denial management in medical billing by focusing on prevention, visibility, and continuous improvement across the revenue cycle. Rather than relying solely on post-denial appeals, its approach targets the root causes that drive repeat denials.
Key capabilities include:
- Pre-submission validation to identify patient demographic errors and claim submission mistakes before claims reach payers
- Coding accuracy checks to reduce errors related to CPT, ICD, and modifier usage
- Eligibility verification workflows to prevent coverage-related denials
- Prior authorization tracking to ensure required approvals are obtained and documented
- Denial trend reporting and analytics to uncover recurring issues and emerging RCM denial trends
By integrating these capabilities into existing billing operations, Qualigenix enables providers to reduce denial rates, accelerate payment cycles, and improve financial predictability.
Fuel Sustainable Growth with Precision Billing in 2026!
Denial management in medical billing is no longer a reactive process focused solely on recovering unpaid claims. In 2026, it is a proactive, data-driven discipline that directly impacts financial performance.
Healthcare providers who identify claim denial causes early, eliminate documentation gaps, and improve front-end accuracy are better positioned to protect revenue and reduce administrative strain. Strong denial management not only improves cash flow but also strengthens compliance, operational efficiency, and long-term sustainability.
As payer requirements continue to evolve, providers that invest in structured denial management workflows will maintain a competitive advantage in an increasingly complex reimbursement landscape.
FAQs
1. What is denial management in medical billing?
Denial management is the process of identifying denied claims, analysing denial reasons, correcting errors, and resubmitting or appealing claims to recover revenue within the revenue cycle.
2. Why do medical billing claim denials happen so often?
Denials occur due to complex payer rules, coding errors, eligibility issues, documentation gaps, and claim submission mistakes that fail automated or manual payer reviews.
3. What is the most common reason for claim denials?
Incorrect patient information, coding errors, and missing prior authorizations are among the most frequent drivers of medical billing claim denials.
4. How long does it take to resolve a denied claim?
Resolution time varies based on payer requirements and denial type, ranging from a few days for simple corrections to several weeks for documentation-based appeals.
5. Can denied claims still be paid?
Yes. Many denied claims are recoverable if errors are corrected and appeals are submitted within payer-defined timelines with appropriate supporting documentation.
6. How can providers reduce future denials?
Providers can reduce denials by improving eligibility verification, maintaining coding accuracy, securing prior authorizations, and implementing structured denial management workflows.


