Charge Capture in Healthcare: Common Errors & How to Fix Them
The Qualigenix Editorial Team comprises certified medical billing professionals, CPC-credentialed coders, prior authorization specialists, and revenue cycle consultants with more than 40 years of combined hands-on experience serving solo physicians, group practices, hospitals, and ASCs across 38+ specialties in the United States. Every guide, article, and resource published on the Qualigenix blog is researched against current CMS guidelines, Federal Register notices, AMA policy updates, and payer-specific billing rules — and reviewed for compliance accuracy before publication. Our content reflects the same standards we apply to our client work: 99% claim accuracy, 95% first-pass acceptance, and a 30% average reduction in AR days.

Is your healthcare organization losing thousands of dollars before claims even leave your system? Amidst shrinking margins and intense payer scrutiny, charge capture in healthcare has become one of the most expensive failure points in the revenue cycle. According to the Medical Group Management Association (MGMA), healthcare providers lose $125,000 annually due to poor charge capture issues alone. These seemingly small errors, like a missed procedure code, incomplete documentation, or delayed charge entry, can lead to claim denials, payment delays, and permanent revenue loss. But what are the most common healthcare charge capture mistakes costing your practice, and how can you prevent them? Keep reading to find out.
What Is Charge Capture in Healthcare?
Charge capture in healthcare is the process of identifying, recording, and documenting all billable services, procedures, supplies, and treatments provided to a patient. It ensures that every resource used and service provided is accurately tracked for billing and reimbursement.
When executed correctly, charge capture ensures that healthcare organizations receive appropriate compensation for the care they provide. It also helps to maintain compliance with payer regulations and billing standards.
Where Charge Capture Fits in the Revenue Cycle
Charge capture in healthcare is the first step in the revenue cycle. It comes immediately after patient care delivery and before coding and claim submission. The process continues through documentation, coding, and claims submission. Healthcare providers should capture charges in real-time or shortly after the service delivery.
The process involves physician consultations, diagnostic tests, medications, medical devices, and facility charges. If there are any charge capture errors, healthcare organizations cannot bill payers correctly, leading to revenue leakage and billing compliance issues.
Why Accurate Healthcare Charge Capture Matters?
Accurate charge capture in healthcare directly impacts reimbursement, billing compliance, and audit exposure. When done right, it protects revenue and prevents costly denials. But when done poorly, it leads to revenue leakage and regulatory scrutiny. Here’s why accurate charge capture matters:
Maximizes Reimbursement and Revenue
Accurate charge capture ensures every service, procedure, and supply is billed correctly to prevent missed charges and underbilling that permanently affect your revenue.
Reduces Compliance and Audit Risk
Proper documentation and charge audit processes minimize exposure to payer audits. It also helps avoid regulatory penalties and fraud investigations by maintaining billing compliance standards.
Prevents Costly Claim Denials
Capturing charges accurately from the start prevents charge capture errors that could lead to denials. In this way, you can avoid spending on rework and speed up the payment cycles for better cash flow.
Supports Accurate Financial Reporting
Complete charge data gives you a better forecast of your finances so that you can plan your budget and make data-driven decisions to ensure future revenue growth accordingly.
Improves Operational Efficiency
Real-time charge capture reduces administrative burden, redundant charge reconciliation work, and allows staff to focus on patient care rather than billing corrections.
Revenue Leakage vs Compliance Risk
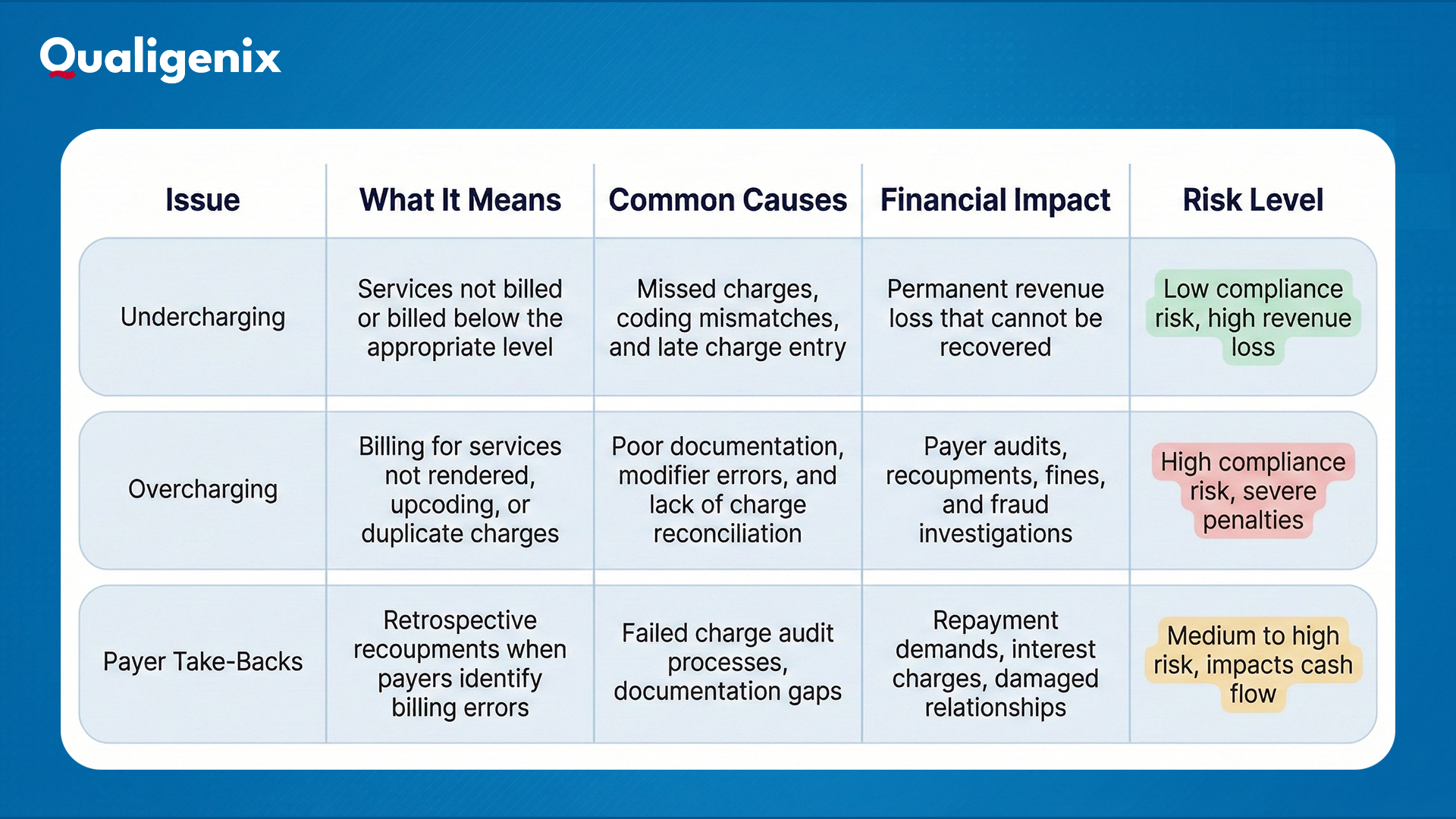
Charge capture errors create problems on both ends of the spectrum. When services are underreported or missed, practices lose revenue through undercharging. When services are overreported, the risk shifts to compliance violations, audits, and payer penalties. The table below highlights how these two issues differ and why getting charge capture right is important for enduring stability.

Common Charge Capture Errors in Healthcare
Most charge capture errors stem from internal operational breakdowns rather than payer-related issues. Here are some common mistakes to look out for to ensure revenue leakage prevention and improve billing accuracy:
Missed or Unrecorded Charges
Missed charges occur when services, procedures, or supplies are provided to patients but are never recorded for billing purposes. This is common in busy healthcare settings where the primary focus is patient care and, in the process, charges are overlooked. Once the billing cycle expires, the charges are lost forever and cannot be recovered.
Late Charge Entry
Late charge entry occurs when billable services are documented days or weeks after the date of service, often missing payer timely filing deadlines. Most payers require claims within 90-365 days of service. But late charges frequently fall outside these windows. Even when submitted on time, delayed charge posting affects cash flow and leads to documentation errors.
Documentation Does Not Support the Charge
Clinical documentation gaps are one of the most common reasons for claim denials and audit failures. When physician notes lack specificity, justification, or detailed procedure descriptions, payers reject charges even if services were legitimately provided. Such weak documentation also increases audit exposure.
Coding and Modifier Mismatches
Coding mismatches occur when the CPT codes or modifiers are not consistent with the services provided or the requirements of the insurance companies. This may occur as a result of using outdated coding information or not adhering to the insurance company’s billing guidelines. Coding inconsistencies may result in automatic rejection of claims.
Charge Description Master Misalignment
Charge description master issues happen when your CDM contains outdated codes, incorrect pricing, or improper code linkages that don’t reflect current procedures. An inaccurate CDM makes it impossible to bill correctly, even when charge capture in healthcare processes is correct.
Duplicate or Incorrect Charges
Duplicate charges occur when the same service is billed multiple times. On the other hand, incorrect charges involve billing for services not provided. Both lead to compliance risk result in payer audits, recoupments, and even fraud investigations. Overcharging damages payer relationships and requires costly refunds that could affect your financial planning.
How Charge Capture Errors Impact Revenue and AR
When charge capture fails, you will face the following consequences:
- Coding Errors and Delays: Clinical documentation gaps and incomplete charge data force coders to query providers. It will delay claims and increase coding mismatches.
- Claim Denials: Missed charges, modifier errors, and incorrect documentation result in denials or underpayments, resulting in expensive rework.
- Collections Challenges: Late claims affect the payment cycle, thereby influencing cash flow and days in accounts receivable.
- Inflated AR Aging: Late charge entry and rework increase receivables beyond 90+ days. It can affect cash flow and increase the risk of write-offs.
- Decreased Clean Claim Performance: Inefficient charge entry affects first-pass acceptance rates and payment cycles.
Downstream Denials and Rework Costs
Charge capture errors cause excess operational workload by forcing staff to rework denied claims, resubmit corrected charges, and appeal rejections. Each denial leads to a rework burden that includes:
- Denial Management: Employees need to analyze denial reasons, collect supporting information, and assess appeal merits for denied claims.
- Claim Resubmission: Claim correction and resubmission prolong the revenue cycle and postpone cash receipts by 30-90 days or longer.
- Appeal Processing: Working on the denied appeals, assembling medical records, and monitoring responses requires extensive administrative effort with no assurance of reimbursement.
How to Fix Charge Capture Issues in Healthcare
To prevent charge capture errors, you need proven strategies that address root causes before they impact revenue. Here are some of our tips to ensure every billable service is captured accurately.
Standardized Charge Capture Workflows
Use the same charge capture process across all departments to avoid confusion and missed charges. When every team follows one clear workflow, it becomes easier to enter charges on time and correctly. Standardization sets clear roles, deadlines, and steps for charge entry. This reduces errors, improves consistency, and helps your organization capture all billable services without delays.
Clinical Documentation Alignment
Clinical documentation helps in charge capture as it relates every service to a medical necessity and procedure description. Train the providers to document their services at the point of care to avoid clinical documentation gaps that lead to denials.
Regular Charge Audits and Reconciliation
Implement charge audit processes and charge reconciliation on a routine basis to identify errors before claims are submitted. This may decrease the risk of denial and, in the end, prevent revenue leakage. Charge audits can identify trends such as delayed charge capture, coding discrepancies, and charge description master issues.
Technology and Automation Controls
Real-time validation systems and automated alert notifications point out errors in charge capture, modifier errors, and duplicate charges as soon as the charges are entered. Technology systems minimize the chances of errors and make sure that the charges are accurate and complete before they are submitted to the billing system.
How Qualigenix Helps With Charge Capture in Healthcare

At Qualigenix, we understand that charge capture errors directly impact your bottom line. Our comprehensive solutions are designed to eliminate revenue leakage before it happens, to ensure every billable service is accurately captured, coded, and submitted. Here’s how we help healthcare organizations optimize their charge capture processes:
- Workflow Standardization and Process Optimization: We implement standardized charge capture workflows to eliminate inconsistencies and ensure best practices across all departments.
- Real-Time Validation of Clinical Documentation: We perform real-time validation of clinical documentation to detect any gaps that could become billing problems.
- Alignment and Accuracy of Coding: We ensure that your coding processes are in line with the latest standards to avoid undercoding, overcoding, and modifier errors.
- Review of Charge Description Master (CDM) System: Our professionals conduct regular reviews of your CDM system to ensure that your charges are accurate and that codes are properly linked.
- Pre-Billing Audits and Quality Assurance: We perform pre-billing audits to detect any problems before the billing process to prevent denials and expedite payments.
Secure Your Revenue with Qualigenix Charge Capture Solutions
Charge capture in healthcare is important for accurate billing and sustainable revenue. Providers who identify and fix capture errors early can protect their bottom line, reduce compliance risk, and improve cash flow stability. Resolving common charge capture mistakes will help you build a resilient financial infrastructure for your organization. Ready to eliminate charge capture errors and maximize reimbursements? Contact Qualigenix today!
FAQs
1. What is charge capture in healthcare?
Charge capture in healthcare is the process of recording all billable services, procedures, and supplies delivered to patients for accurate billing and reimbursement.
2. Why do charge capture errors happen?
Charge capture errors occur due to:
- Workflow breakdowns
- Clinical documentation gaps
- Late charge entry
- Lack of staff training
- Poor communication between clinical and billing teams
3. What departments are involved in charge capture?
An effective charge capture in healthcare requires seamless coordination across all three departments. The departments included in the process are:
- Clinical staff document services
- Coders assign appropriate codes, and
- Billing teams submit claims.
4. How does poor charge capture affect claim denials?
Poor charge capture leads to missed charges, coding mismatches, and incomplete documentation. It could ultimately lead to payer denials, increase rework costs, and delay reimbursement.
5. Can charge capture errors be corrected later?
Some errors can be corrected through claim resubmission or appeals. But missed charges past the filing deadlines result in permanent revenue leakage that cannot be recovered.
6. Can charge capture be outsourced or audited externally?
Of course! You can partner with leading providers like Qualigenix for charge audit processes, charge reconciliation, and workflow improvements that reduce errors, ensure billing compliance, and maximize your revenue capture.