Top 5 Benefits of Automating Your Revenue Cycle Management
The Qualigenix Editorial Team comprises certified medical billing professionals, CPC-credentialed coders, prior authorization specialists, and revenue cycle consultants with more than 40 years of combined hands-on experience serving solo physicians, group practices, hospitals, and ASCs across 38+ specialties in the United States. Every guide, article, and resource published on the Qualigenix blog is researched against current CMS guidelines, Federal Register notices, AMA policy updates, and payer-specific billing rules — and reviewed for compliance accuracy before publication. Our content reflects the same standards we apply to our client work: 99% claim accuracy, 95% first-pass acceptance, and a 30% average reduction in AR days.

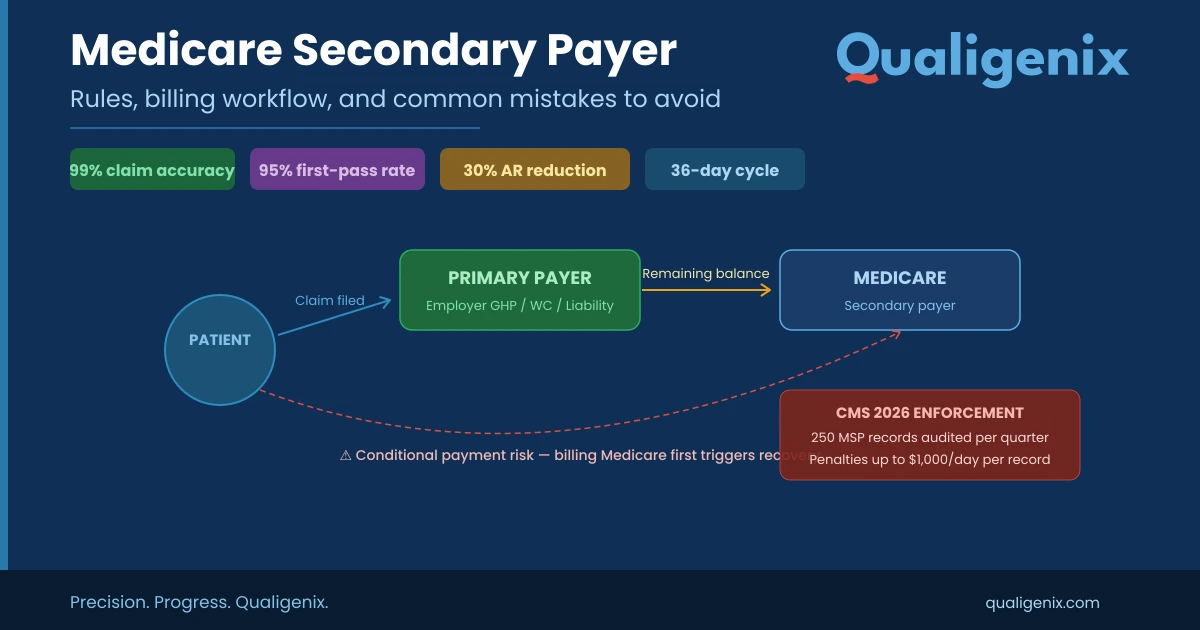
Automation is no longer optional for revenue cycle management. In 2025, leading health systems utilize bots and AI to eliminate manual steps, enforce claim logic, and shrink AR days—all while remaining resilient when payers or tech platforms experience issues. The global healthcare automation market is projected to grow rapidly, and by 2025, 80% of organizations are expected to utilize intelligent automation in operations.
Your revenue cycle should begin before a patient even walks into the clinic. Medical billers must validate insurance and benefits before confirming appointments. That front-loading prevents rejections downstream. So, read on to learn key revenue cycle automation benefits, how automation delivers real, measurable value across eligibility, prior authorization, coding, and claim scrubbing, status tracking, and auto-posting.
Why Automation Matters in RCM
If your team automates only because it “feels modern,” you’ll burn effort without impact. But if you connect automation to real points of failure in your cycle, it’s transformative. These are the pressures pushing RCM teams toward automation, and where automation can pull them out.
Rising Denial Pressures & Capacity Constraints
Healthcare providers now face denial environments that demand responsiveness. Manual denial remediation is labor-intensive and often reactive. Automation helps absorb volume surges and frees up staff to catch patterns instead of putting out fires.
Error Rate from Manual Work
Human entry errors, such as wrong member IDs, typos in procedure codes, and overlooked modifiers, remain consistent denial drivers. Automation reduces common claim errors by checking, validating, and correcting data before submission.
Operational Cost & Staff Burnout
Every billing cycle includes repeated clicks: eligibility queries, payer calls, and remittance posting. Over time, these tasks wear staff down, increase turnover, and inflate cost-to-collect. Automation can offload up to millions of hours of repetitive work.
Visibility Gaps and Reaction Lag
Without real-time dashboards, teams spot error patterns days or weeks later. By then, many denials have aged, appeal windows may close, and AR days are already stretched. Automation gives an earlier signal detection, so you act before trends cascade.
Compliance & Rule Complexity
Payers change rules frequently. Manual teams struggle to keep up with payer edits, Local Coverage Determinations (LCDs)/National Coverage Determinations (NCDs) guidance, or new modifier logic. Automation can centralize payer-specific rules, making updates faster and reducing the “denial fallout” when rules shift overnight.
The Top 5 Benefits of RCM Automation
Automation delivers value not in grand gestures, but in dozens of small accelerations that compound. Below are five key revenue cycle automation benefits that define why automation matters and how it reshapes modern revenue cycle management:
-
Higher First-Pass Yield and Clean Claims
A clean claim decides how fast a provider gets paid. Automation ensures that every claim meets payer rules and reduces avoidable denials before submission.
Pre-Submission Edits Lift Accuracy
Automation checks each claim before submission. It identifies missing patient details, incorrect codes, or invalid modifiers that could trigger denials. Each corrected error improves the chance of first-pass approval and smoother payment cycles.
Payer-Specific Rules Create Precision
Every payer uses its own guidelines. Automation updates these rules continuously and applies them during claim creation. This constant alignment improves compliance, raises acceptance rates, and strengthens the overall clean-claim rate.
Coded Documentation Builds Confidence
Automation confirms that the documentation supports every billed service. It validates medical necessity and matches diagnosis codes to treatment details. Fewer mismatches mean fewer audits and faster reimbursements, ensuring consistency in denial reduction.
-
Lower Cost-to-Collect
Manual work drives up cost and slows down billing. Automation lowers the total cost-to-collect by replacing repetitive steps with accurate digital workflows.
Routine Tasks Become Automated
RPA in RCM tools now handles tasks like eligibility verification, claim status checks, and payment posting automatically. Systems such as AKASA and Thoughtful AI process large volumes of data around the clock, freeing staff to focus on exceptions and value-driven tasks.
Efficiency Reflects in Cost Metrics
Each automated claim requires fewer touches and less time in the queue. These efficiencies reduce rework and administrative overhead. Over time, cost-per-claim metrics improve, which proves automation’s value in measurable financial terms.
Staff Productivity Rises
Automation shifts staff time from data entry to analysis and strategy. Teams can study payer patterns, refine appeal workflows, and improve patient engagement. A more focused workload improves morale and retention while enhancing performance across the billing cycle.
-
Faster Accounts Receivable Turnaround
Cash flow determines how resilient a healthcare organization is. Automation helps move claims from submission to payment faster and keeps the revenue cycle consistent.
Real-Time Status Tracking Keeps Cash Moving
AI billing tools monitor payer portals continuously and update claim status within the billing system. Teams always know which claims are pending, accepted, or denied. This visibility prevents overlooked follow-ups and reduces payment delays.
Intelligent Routing Reduces Aging Claims
Automation assigns delayed claims to the right team member automatically. When a payer exceeds its usual turnaround window, the system triggers a follow-up alert. This proactive workflow lowers AR days and stops claims from aging beyond filing deadlines.
Fewer Reworks Improve Velocity
Clean claims and automated follow-ups lead to quicker approvals and shorter billing cycles. Providers using claim-tracking automation often see a 20 to 30 percent improvement in cash turnaround within the first quarter of deployment.
-
Real-Time Visibility, ROI, and Resilience
Automation brings full transparency into financial operations. It shows where delays begin, how quickly claims move, and where to direct improvement efforts.
Centralized Dashboards Provide Clarity
Automated dashboards present live data on first-pass yield, denial rates, and AR days across departments and payers. This clear visibility allows managers to spot recurring issues early and measure RCM automation ROI through direct results.
Continuous Data Creates Measurable ROI
Automation replaces assumptions with real data. Each process—from eligibility to posting—feeds into unified analytics. Leaders can see precise improvements in acceptance rates, AR cycles, and collection costs, proving automation’s financial impact.
Built-In Redundancy Prevents Downtime
A multi-clearinghouse setup ensures that claim flow continues even if one network experiences downtime. Systems with clearinghouse redundancy reroute and re-queue claims automatically, maintaining uninterrupted billing and steady cash flow.
Security by Default Ensures Trust
Automation systems include strong protection. Multi-factor authentication, encryption, and access control limit exposure. Immutable backups and audit logs create full transparency and guarantee compliance during audits.
-
Improved Staff Performance and Process Efficiency
Automation improves how teams work and collaborate. It gives professionals the tools and time to focus on analysis, accuracy, and problem-solving.
Time Redirected Toward High-Value Work
Automation manages routine verifications, claim tracking, and payment posting. This gives staff time to manage exceptions, improve denial appeal rates, and build stronger payer communication. Teams feel more in control and more engaged.
Process Efficiency Strengthens Culture
Automation creates order within daily operations. Teams work from reliable data, align tasks easily, and maintain visibility across the workflow. Efficiency becomes part of everyday culture instead of a periodic goal.
Automation Supports Scalable Growth
As patient volume grows, automation absorbs additional workload without additional headcount. It keeps billing accurate and consistent, even at scale. This balance ensures growth enhances profitability instead of straining the team.
Building Your Automation Roadmap
Implementing robotic Process Automation (RPA) in RCM can feel overwhelming. A phased roadmap helps you start small, prove success, and scale confidently. The best approach balances technical setup with measurable performance goals.
Identify High-ROI Transactions
Begin with processes that are rule-driven and repetitive. These include eligibility verification, prior authorization, claim status tracking, and auto-posting of remittances. These areas generate quick, visible wins because they reduce errors and increase throughput immediately. Document baseline performance metrics before starting, so improvement is clear later.
Prove Value Within 90 Days
Set specific goals such as a 3 percent improvement in the first-pass claim rate, a 20 percent drop in denial volume, or a 15 percent cut in cost-to-collect. Track these numbers weekly and share progress across teams. Clear results within 90 days build internal confidence and justify expansion.
Scale Through Standardized Playbooks
Once the pilot succeeds, create playbooks that define ownership, escalation thresholds, and review frequency. Expand the automation department by department. Each team can apply the same playbook while tailoring minor details to its workflow. This keeps growth structured and sustainable.
How Qualigenix Powers RCM Automation

At Qualigenix, we combine automation technology with deep RCM expertise to help healthcare organizations transform revenue performance. Its approach blends data analytics, AI-driven bots, and operational support to deliver measurable improvements quickly.
Why Qualigenix
We bring together eligibility and authorization bots, coding quality assurance, and payer-specific claim edits. These features work in sync to improve accuracy and reduce delays. Every automation follows payer compliance rules and updates automatically when regulations change.
What You Get
Clients receive a complete automation program with dashboards that track clean claim rate, denial trends, and AR performance in real time. Exception worklists help teams focus on outliers, whereas automated payment posting ensures remittances are recorded accurately and instantly. The overall effect is fewer denials, faster payments, and cleaner books.
How It’s Delivered
The 30-60-90 day rollout allows seamless integration with your EHR or billing software. SLAs back every project, guaranteeing reductions in AR days and improvement in first-pass yield. Qualigenix also builds resilience through redundant connections and continuous compliance audits, so your automation stays secure and stable.
Turn Every Claim Into Cash Flow with Smarter Automation!
Automation gives healthcare providers control over their revenue again. It replaces guesswork with real-time clarity and makes payments predictable. The right automation strategy reduces denials, shortens AR days, and strengthens staff efficiency.
Start with the processes that create the most friction: eligibility verification, authorizations, claim status checks, and remittance posting. Understand all revenue cycle automation benefits, measure results, refine workflows, and then expand. So, partner with Qualigenix today. Automation will not replace your team. It will help them achieve more with less effort and ensure every dollar of earned revenue reaches your account.
FAQs
1. Which RCM tasks should be automated first?
Start with tasks that involve repetitive manual work and deliver quick results. Eligibility verification, prior authorization, claim status tracking, and payment posting are strong starting points. These processes handle predictable data and high volumes, so automation improves accuracy, reduces turnaround time, and increases staff productivity quickly.
2. How do we measure automation ROI?
Automation ROI is measured by comparing performance before and after implementation. Track AR days, denial rate, first pass claim rate, and cost to collect at consistent 90 day intervals. A reduction in AR days and denials, combined with faster payments, signals that automation is delivering value.
3. Will automation replace staff?
Automation does not replace skilled billing professionals. It removes routine tasks that slow teams down. Staff can then focus on denial analysis, payer pattern review, and patient support. This shift moves billing teams from reactive work to proactive revenue management.
4. Do we need multiple clearinghouses?
Using more than one clearinghouse strengthens revenue cycle stability. If one network faces delays or downtime, claims can be routed through another. This redundancy keeps submissions moving and protects cash flow from system interruptions.
5. What security measures are essential for automated RCM systems?
Key security measures include multi factor authentication, role based access, and encryption for data at rest and in transit. Immutable backups and detailed audit trails for every automated action support compliance and protect against data breaches.